Dr. Steven Phillips on Chronic Inflammation
http:// Approx. 1 Hour
March 25, 2023
Dr. Steven Phillips Discusses Chronic Inflammation
Dr. Steven Phillips discusses chronic inflammation and its management, especially in the context of long COVID and “vaccine” injuries.
Dr. Steven Phillips’ bio: Steven Phillips, MD is a well published, Yale-trained physician, researcher, and bestselling author, whose focus of medical practice and research is that chronic and autoimmune illness can be caused by underlying infections.
Dr. Phillips’ substack: https://zerospin.substack.com/
Amazon.com: Chronic: The Hidden Cause of the Autoimmune Pandemic and How to Get Healthy Again (Audible Audio Edition): Steven Phillips MD, Dana Parish, Teri Schnaubelt, Thomas Allen, Brilliance Audio: Books https://www.amazon.com/Chronic-Hidden…
Dr. Steven Phillips Discusses Chronic Diseases (Lyme & COVID)
Steven Phillips, M.D. is a renowned Yale-trained physician, author, international lecturer, and media go-to expert. Well-published in the medical literature, he has treated over 20,000 patients with complex, chronic illness from nearly 20 countries. Phillips experienced firsthand the nightmare of an undiagnosed, serious infection after nearly dying from his own “mystery illness,” and having to save his own life when 25 doctors could not.
Here are the questions we will ask Dr. Phillips:
- What is Lyme+?
- What is your own story of Lyme?
- You say that many infections are categorized as Lyme, how do we separate them
- Are there good tests for Lyme+?
- Is it treatable?
- Is there hope for hundreds of thousands of patients of Lyme+?
- How can an infection cause autoimmune disorders?
- What is the role of Th1 and Th2 system in this context?
- Why does it become chronic?
- Do I have a vector borne infection?
- We are seeing the same issue with COVID – Is COVID becoming similarly mismanaged?
- How should patients approach their chronic Lyme+?
- Is there hope?
- How do people get help from you?
- Do you train other doctors with your protocol?
- Do they reach out to you?
- On page 63 you write: Despite my repeatedly negative brucellosis testing at U.S. labs, I shared with my Lyme doctor my ideas for an aggressive combination antibiotic treatment against this infection. Nothing else was working, so my doctor agreed to the plan, and by the second month of treatment I started to improve.
- Tell us about Jarish-Hexheimer reaction
- Before we go, tell us how can people find you?
For more:
- https://madisonarealymesupportgroup.com/2021/02/09/chronic-the-hidden-cause-of-the-autoimmune-pandemic-how-to-get-healthy-again/
- https://madisonarealymesupportgroup.com/2016/07/11/dr-phillips-completely-trounces-cdc/
- https://madisonarealymesupportgroup.com/2016/07/01/unedited-interview-with-dr-phillips-fox-5-ny/
- https://madisonarealymesupportgroup.com/2018/12/22/s-e-x-lyme-msids/
- https://madisonarealymesupportgroup.com/2016/04/03/dr-phillips-does-it-again/
- https://madisonarealymesupportgroup.com/2021/03/24/the-hidden-immune-pandemic/
- https://madisonarealymesupportgroup.com/2021/03/02/autoimmune-pandemic-dr-phillips-dana-parish/
- https://madisonarealymesupportgroup.com/2018/12/22/research-news-dr-steven-phillips/
- https://madisonarealymesupportgroup.com/2021/07/26/research-consortium-aims-to-develop-new-drug-for-bartonellosis/
- https://madisonarealymesupportgroup.com/2017/10/04/dr-steven-phillips-writing-book-on-lyme-and-bartonella-treatment/
- https://madisonarealymesupportgroup.com/2021/12/08/link-between-autoimmune-disease-chronic-fatigue-and-hidden-infections/
- https://madisonarealymesupportgroup.com/2021/04/27/lyme-other-tick-borne-diseases-with-dr-philips-dana-parish/
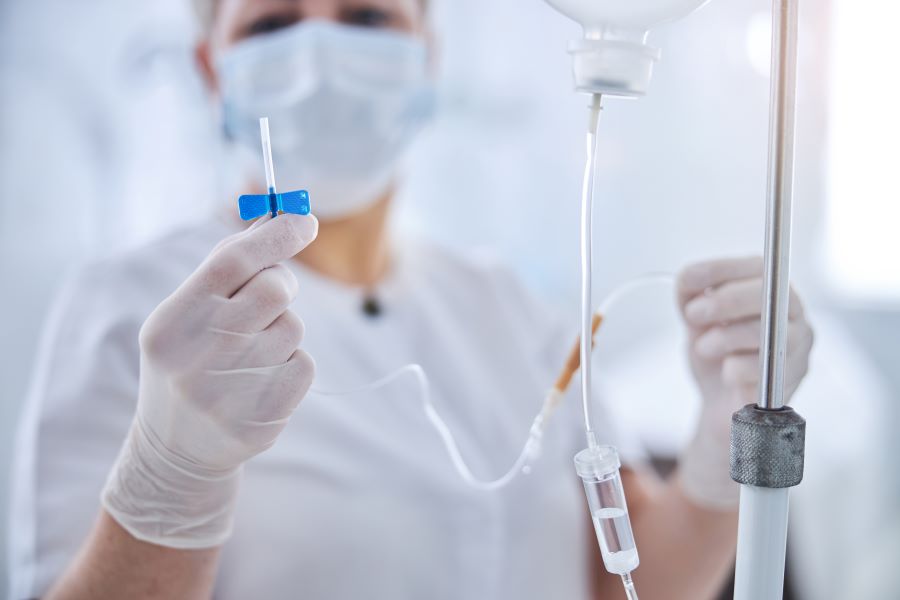
- https://madisonarealymesupportgroup.com/2020/06/08/dr-phillips-dads-recent-covid-19-outrage-triumph/ Since this was written, much data is available on the effectiveness of ivermectin for COVID, but doctors are being attacked, the drug is being censored and banned, and hospitals have become modern day “killing fields,” due to the “Fauci death protocol” using deadly ventilators and dangerous, ineffective remdesivir. The reason for this is two-fold:
- The CARES Act, which provides hospitals with bonus incentive payments for all things related to COVID-19 (testing, diagnosing, admitting to hospital, use of remdesivir and ventilators, reporting COVID-19 deaths, and vaccinations)
- Waivers of customary and long-standing patient rights by the Centers for Medicare and Medicaid Services (CMS) which allows hospitals to “violate the rights of patients or their surrogates with regard to medical record access, to have patient visitation, and to be free from seclusion. This simply means COVID patients are literally prisoners in the hospital, are isolated, and have no say in their treatment.
Hospital payments include:
- A “free” required PCR test in the Emergency Room or upon admission for every patient, with government-paid fee to hospital. This test, like Lyme testing, is an utter farce.
- Added bonus payment for each positive COVID-19 diagnosis, based on a worthless test.
- Another bonus for a COVID-19 admission to the hospital, based on a worthless test.
- A 20% “boost” bonus payment from Medicare on the entire hospital bill for use of remdesivir instead of medicines such as Ivermectin, all based on a worthless test.
- Another and larger bonus payment to the hospital if a COVID-19 patient is mechanically ventilated, all based on a worthless test.
- More money to the hospital if cause of death is listed as COVID-19, even if patient did not die directly of COVID-19, which is all based on a worthless test.
- A COVID-19 diagnosis also provides extra payments to coroners, all based on a worthless test.
CMS implemented “value-based” payment programs that track data such as how many workers at a healthcare facility receive a COVID-19 “vaccine.” Now we see why many hospitals implemented COVID-19 vaccine mandates. They are paid more. Source