North America is “Ground Zero” For Babesiosis
https://www.lymedisease.org/ground-zero-babesiosis/

https://www.lymedisease.org/ground-zero-babesiosis/
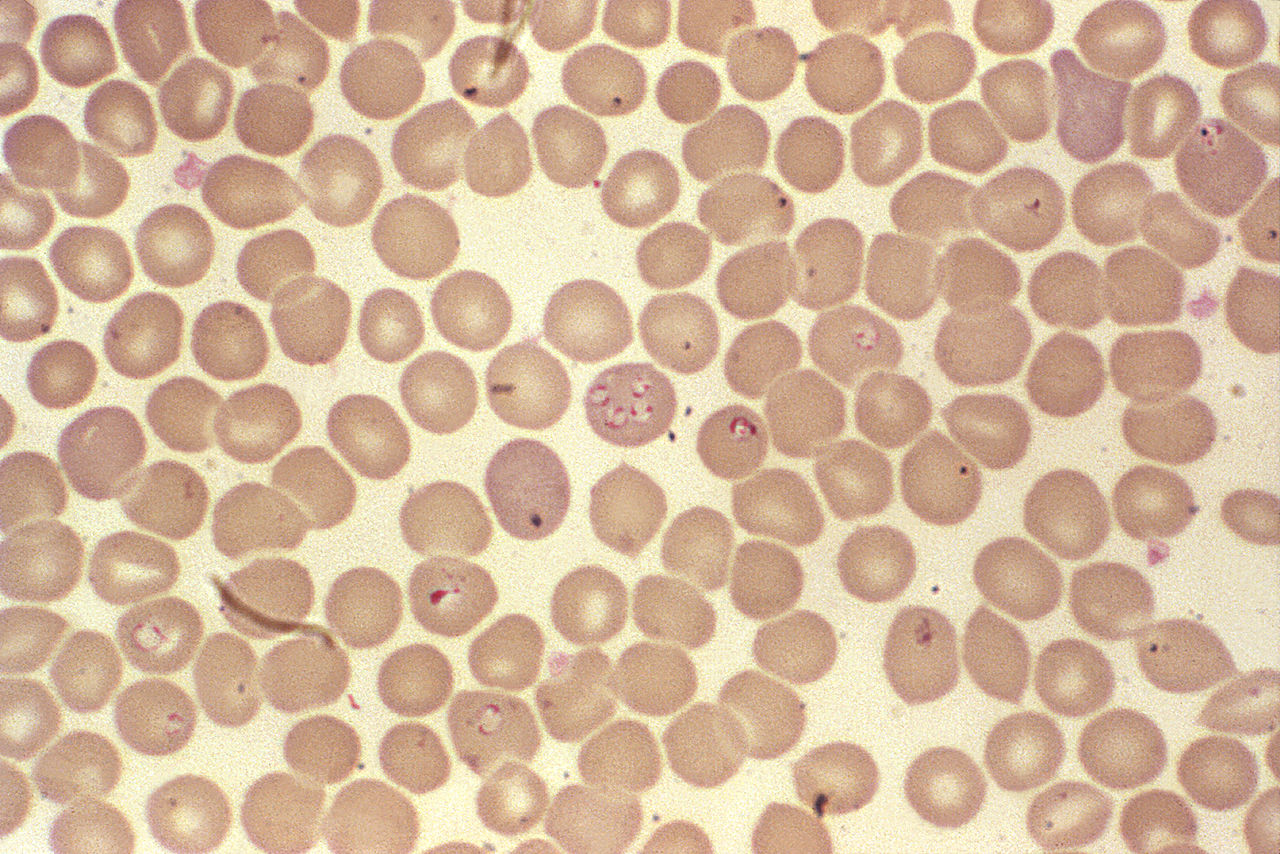
Photo Credit: Content Providers(s): CDC/ Steven Glenn; Laboratory & Consultation Division – This media comes from the Centers for Disease Control and Prevention’s Public Health Image Library (PHIL), with identification number #5943.
Approx. 2 min. Published on May 8, 2012
Brittany Goff found out that not only was she suffering from Lyme disease, she also had Babesiosis, a parasite that invades red blood cells.
Approx. 2:50 min on Jul 28, 2009
This 3 minute video demonstrates the life cycle of Babesia microti, starting in the blood of white-footed mice. Follow the parasite as it is ingested by deer ticks, and finally is transmitted to humans through tick saliva. Special thanks to Rick Smith at The University of Rhode Island for narration; Rick’s brother was recently diagnosed with Lyme disease.
Babesia is a genus of protozoan that enters red blood cells at the sporozoite state causing a parasitic, hemolytic disease. Over 100 species have been identified but only a few have been documented to infect humans, although Dr. Schaller states that there are new Babesia species emerging every one to four months with a new protozoan that while it looks like Babesia, when genetically sequenced, isn’t – it’s a new infection entirely called FL1953 or Protomyxzoa Rheumatica. Horowitz says studies are showing a worldwide epidemic of babesiosis, and similar to Lyme, can persist. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1925019/ http://lymebytes.blogspot.com/2011/09/bartonella-and-babesia-symptom.html
http://www.lymediseaseblog.com/babesia-common-lyme-disease-coinfection/ In the red blood cell, the protozoa continue to split until the cell bursts and releases the micro-organisms into the blood where the freed protozoa find new red blood cells to keep producing. This causes decreased oxygen, and hemoglobin is released into the blood plasma which can cause jaundice. Broken cell fragments can start to accumulate which can cause serious hyper coagulation (thick blood). Proper treatment needs to address these issues to be effective.
http://www.lymefight.info/ticks-101/ticks-tick-borne-diseases/co-infections-babesia/ In the US, B. microti is the most common strain and people who contract it suffer from malaria-like symptoms such as:
*Irregular and/or high fever and chills in some patients
*Severe fatigue and lethargy
*Global headaches, like a hat is too tight (severe pressure-like headaches – sometimes in ears
*Eye pain
* Sensitivity to light, touch, sound, or smells
*Body aches, muscle pain
*Fevers of up to 104 degrees
*Chills, sweats, especially night sweats
*Breathing problems, “air hunger” or shortness of breath, or frequent sighing
*Occasional dry cough
*Chest pain
*Poor balance
*Encephalopathy (brain disease, damage or malfunction)
*Hemolytic anemia (red blood cells burst apart)
*Hypercoagulation (thick blood often requiring a blood thinner as the patient can’t get enough oxygen which can cause fatigue not to mention the inability to get nutrients and antimicrobials where they need to go) http://www.anapsid.org/cnd/diffdx/hypercoagulation.html
*jaundice
*hemoglobinuria (free hemoglobin in the urine – resulting in a reddish-yellow to fairly dark red color)
*Mood disorders such as depression, mood swings, and anxiety are worsened
*Flushing
*Nightmares and/or vivid dreams
*Insomnia
*Loss of Appetite
*Abdominal pain
*Enlarged liver
*Swollen spleen
For a more complete checklist, please go to: https://madisonarealymesupportgroup.wordpress.com/2011/09/25/the-babesia-checklist-copyrighted-2011-james-schaller-md-mar-version-20/
Besides being transmitted by ticks, Babesia has been spread via blood transfusions, organ transplants, stem cells (Buhner, 2015), and congenitally. http://www.cdc.gov/parasites/babesiosis/epi.html
http://www.ncbi.nlm.nih.gov/pubmed/19402971
Going back to 1998, it was known that when a patient has Lyme and Babesia, Lyme is found three-times more frequently in the blood, causing greater symptoms, disease severity, and duration of illness: https://reference.medscape.com/medline/abstract/8637139
https://madisonarealymesupportgroup.com/2017/06/28/concurrent-babesiosis-and-lyme-in-patient/ Great example of a previously healthy 39-year-old male presenting to the emergency department (ED) with generalized severe headaches for eight days and fever for four days. Abdominal examination was normal except for a swollen spleen.
http://www.lymepa.org/c07%20Lyme%20disease%20and%20Babesiosis%20coinfection.pdf It also suggests a synergistic inflammatory response to both a parasitemia and an increased spirochetemia. In addition, babesial infection enhances Lyme disease myocarditis in mice, which suggests that coinfection might also synergize spirochete-induced lesions in human joints, heart, and nerves.
Telling quote:
Persistent and debilitating fatigue characterized coinfection.
https://www.sciencedirect.com/science/article/abs/pii/S0020751918302406
Similar to humans, B. microti coinfection appears to enhance the severity of Lyme disease-like symptoms in mice. Coinfected mice have lower peak B. microti parasitaemia compared to mice infected with B. microti alone, which may reflect attenuation of babesiosis symptoms reported in some human coinfections. These findings suggest that B. burgdorferi coinfection attenuates parasite growth while B. microti presence exacerbates Lyme disease-like symptoms in mice.
Dr. Horowitz warns that due to this immune suppression, patients with Rheumatoid Arthritis or Lupus and are on immunosuppressant drugs, if they have Babesia, could get much worse. The strain, B. divergens, causes a higher mortality rate and more severe symptoms, and if left untreated, this strain can develop into shock-like symptoms with pulmonary edema and renal failure.
The challenge with diagnosis, as always, is the testing which is poor as these organisms are not often found in high enough numbers in the blood, as well as people present subclinically. In other words, their Lyme case is more severe and they have malarial-type symptoms, but they can’t find Babesia in the blood in a Giemsa stain. It takes a trained eye to identify Babesia, which produces a Maltese Cross form, which may or may not be present in a particular smear. Also, doctors have been taught that besides the day and night sweats and chills, patients are supposed to get hemolytic anemia and their liver functions go up or their platelet count might go down (thrombocytopenia). The fly in the ointment is that only certain strains of Babesia do this. Many strains do not cause these symptoms – but doctors aren’t educated on these finer points. Also, to hide from the immune system, the various species produce offspring that have different exterior proteins, or genotypes. http://www.townsendletter.com/July2015/babesia0715_2.html According to Schaller, there is immense variation and pre-2015 treatments were “weak and showed ignorance of the power of Babesia – it is vastly harder to kill than malaria.”
According to Dr. Horowitz there is a form of Babesia called ARDS, acute respiratory distress syndrome, or adult respiratory distress syndrome. There are cases of folks with this in the hospital who were given steroids, which suppress the immune system, and have died. (Steroids suppress the immune system and are NOT to be given when a person has a raging infection such as Babesia, Lyme, or other TBI) https://madisonarealymesupportgroup.com/2019/01/11/22-with-babesia-8-develop-acute-respiratory-distress-syndrome-3-die/
Great article on Babesia: https://suzycohen.com/articles/lyme_babesia_treatment/ Table obtained from Dr. Suzy Cohen’s link above:

The challenge with treatment is most doctors are under the impression that 10 days of an antimalarial will cure babesiosis. Horowitz states that Babesia is one of the most dangerous and tenacious co-infections he deals with and treats for 9-12 months.
https://www.ncbi.nlm.nih.gov/pubmed/18181735 Even this 2008 study states that,
“Immunocompromised people who are infected by B. microti are at risk of persistent relapsing illness.”
If you find a doctor willing to be properly educated on tick borne illness, please give them this link: https://madisonarealymesupportgroup.com/2017/06/20/help-doctors-get-educated-on-lyme-and-tick-borne-illness/
Babesia Treatment: (FOR EDUCATIONAL PURPOSES ONLY. PLEASE DISCUSS ALL TREATMENTS WITH YOUR MEDICAL PROFESSIONAL)
In order to beat Babesia it is important to improve the immune system, correct sleep issues, supplement any imbalances with vitamins, minerals, bioidentical hormones, remove yeast, and decrease pain.
Standard treatment used to be clindamycin and quinine for seven days – the same treatment for malaria; however the side effects are as bad as the disease and due to the need to often treat for months rather than days, new regimens were discovered out of necessity. Also, length of treatment for Babesia is similar to all the other tick borne infections and can take much longer than the 7-10 day course the CDC specifies. In fact Buhner (2015) states, “Failure to treat for longer than 7-10 days risks disease recurrence, often with worsening symptoms, including death.”
The most recent research shows that the antimalarial drug Tafenoquine & the anti-fungal/anti-parasite drug Atovaquone achieves radical cure and confers sterile immunity in experimental models of human Babesiosis. Two points to keep in mind: 1) this work was done on cultured human cells in a petri dish and then in a mouse model. The jury’s out on how it performs in actual humans. 2) Babesia rarely comes alone and patients typically have other pathogens requiring different medications for a longer period of time.
http://www.treatlyme.net/treat-lyme-book/kills-babesia-a-brief-guide
According to Dr. Marty Ross, Babesia treatment requires four to five months – one month longer than the average length of time a red blood cells lives after it is made by the bone marrow. And similarly to his Bartonella treatment he has three tiers of treatment, each with varying success. Horowitz advises 9 months to a year of treatment.
Recently, Dr. Ross gave an update, found here: https://madisonarealymesupportgroup.com/2022/03/24/kill-babesia-treatment-guide-update/ The main update I can see is his focus on “Babesia Nests” and a blood clotting protein called fibrin which limits blood flow to tissues and may inhibit antimicrobials as well as the immune system. He uses:
Also in this update he addresses Babesia microti specifically and that tafenoquine, a newer anti-malaria medication approved in 2018 has good effects against in the lab and in a recent case report.
He also states that research on those who have Babesia WITH Lyme is nonexistent. Most LLMD’s treat Babesia for 3 weeks on and one week off treatment.
Tier 1: (85% success rate)
Atovaquone/proquannil 250mg/100mg. Start atovaqune/proquanil at 2 pills 2X/day for 3 days then decrease to 1 pill 2 times a day. Combine with one of the following:
*azithromycin (Zithromax) 500mg 1 time a day,
*clarithromycin (Biaxin) 500mg 1 pill 2 times a day,
*doxycycline 100mg 2 pills 2 X/day, or *minocycline 100mg 1 pill 2 times a day.
In addition if these combinations are not working he sometimes adds:
*sulfamethoxazole/trimethoprim 800mg/160mg (Bactrim DS or Septra DS) 1 pill 2 times a day to create a 4 drug regimen. (Atovaqone/proquanil (Malarone) is two drugs in one pill)
Atovaquone Combination
Atovaquone (Mepron) 750mg/5ml 5ml two times a day. In 1 to 2 months if night sweats or other babesia symptoms are not improving then increase the dose to 10ml two times a day. Combine it with one of the following:
*azithromycin (Zithromax) 500mg 1 time a day,
*clarithromycin (Biaxin) 500mg 1 pill 2 times a day,
*doxycline 100mg 2 pills 2X/day, or
*minocycline 100mg 1 pill 2 times a day.
In addition if these are not working he sometimes adds:
*sulfamethoxazole/trimethoprim 800mg/160mg (Bactrim DS or Septra DS) 1 pill 2 times a day to create a 4 drug regimen. (Atovaquone/proquanil (Malarone is two drugs in one pill)
*Atovaquone can cause temporary liver damage. Blood tests for liver function must be used regularly. Some recommend omitting CoQ10, ALA, and vitamin E because they are fat soluble antioxidants that some think neutralize the pro-oxidance effects of atovaqyone against Babesia. Some doctors disagree with this. Be sure to take atovaquone with enough fat to avoid nausea or diarrhea and to increase absorption. Choices include cheeses, avocados, nuts, nut butters, oils, and yogurt.
**Update** Here’s a 2002 study showing that doxycycline and artemisinin may together work synergistically against malaria. The authors speculate that much of the problem with drug resistance in malaria is due to the long half-life of many drugs and that drugs with a short half-life like art and doxy (or its derivatives) would be advantageous. Doxy and art work more slowly and that is helpful with slow growing and dividing pathogens like malaria and quite possibly Babesia. Please remember this study is in vitro: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC126969/
Tier Two: (75-80% success rate)
Artemisinin 100mg. Start with 2-3 pills 2 or 3X/day for 3 days then take 11 days off. Continue this 14 day cycle. The goal is to take 5 pills 3X/day on the 3 days the medication is taken. Ross states that there is an enzyme in the intestine that destroys Artemisinin if it is used longer than 3 days. He also combines it with atovaquone, atovaquone/proquanil, or mefloquine if it is not working well.
Mefloquine 250mg (Lariam) – start at 1 pill daily for 5 days and then take 1 pill every 5 days. Since Mefloquine is stored in fat, it only needs to be taken every 5 days after the initial daily dose.
Combine it with one of the following:
*azithromycin (Zithromax) 500mg daily,
*clarithromycin (Biaxin) 500mg 1 pill 2 times daily,
*doxycycline 100mg 2 pills 2 times a day, or
*minocycline 100mg 1 pill 2 times a day.
If those combinations are not working he sometimes adds:
*sulfamethoxazole/trimethoprim 800mg/160mg (Bactrim DS or Septra DS) 1 pill 2 times a day to create a 4 drug regimen. (Atovaquone/proquanil (Malarone is two drugs in one pill).
*Mefloquine can cause depression, hallucinations, or psychosis. Ross only uses it if there aren’t other affordable options.
Cryptolepis, according to Ross, works about 75% of the time. Take 5ml 3 times a day.
Artemether/lumefantrine 20mg/120mg (Coartem) – take 4 pills 2X/day for 3 days. On the first day take the second dose 8 hours after the first dose. On the 2nd day and 3rd day take each dose 12 hours apart. The 1st dose of the day on all three days should be at the same time. Coartem can be repeated every 2, 3, or 4 weeks. He usually starts every 2 weeks and increases the time between each cycle as long as symptoms do not return on the off antibiotic days.
Tier Three: (Success 75-85%)
Nitazoxanide 500mg (Alinia) 1 pill 2X/day.
Clindamycin 300mg (Cleocin) and either Hdroxychloraquine 200mg (Plaquenil) or Quinine Sulfate 324mg
Option 1: Clindamycin 300mg 2 pills 3 times a day and Quinine Sufate 324mg 2 pills 2X/day. If muffled hearing or other neurologic symptoms other than ringing in the ears develop, then decrease the quinine sulfate to 1 pill 2 times a day.
Option 2: Clindamycin 300mg 2 pills 3X/day and Plaquinil 200mg 1 pill 2 times a day.
Relapse Prevention:
In Ross’ experience, 95% of people with Babesia and Lyme can be cured of it; however, some do relapse. If a person recovers but then relapses, he will put the patient on a preventative program.
Option 1: Atovaquone/Proquanil 250mg/100mg (Malarone) 1 pill daily.
Option 2: Cryptolepis 5ml 3X/day for 2 or 3 weeks on each 4 weeks. Find the frequency that works best.
Option 3: Artemisinin 100mg 2 or 3 pills 3 times a day for 3 days in a row of each 14 days. Repeat cycle continuously.
Dr. Horowitz’s Latest treatments for Babesia: (Horowitz. “Why Can’t I Get Better? Solving the Mystery of Lyme and Chronic Disease.” 2013, pp, 468-469)
Mepron 750mg 1-2 tsp 2X/day, with high fat meal and Zithromax 500mg daily (or Biaxin 500mg 2X/day), Plaquenil 200mg 2X/day, and nystatin tablets 500,000 U 2X/day.
Septra DS one 2X/day may be added if resistant (only if not allergic to sulfa) or if Bartonella is involved. Antimalarial herbs such as artemisinin (approx 1 3X/day), cryptolepis (1 tsp 3X/day – lower if sensitive, 3X/day), or neem (30 drops 3-4X/day) may be layered onto this regimen, again if a case is resistant. Dosing varies by weight. These herbs are typically used one at a time and may be rotated.
Malarone 4 tablets a day for three days as a loading dose, followed by one tablet two times per day. Some with severe symptoms require two tablets 2X/day – Horowitz has not seen adverse effects with this higher dosage. Malarone may be used alone but Mepron should always be used with a macrolide to prevent drug resistance.
Patients who fail Mepron or Malarone should be rotated to clindamycin. Cleocin 300mg, 2 2X-3X/day with plaquenil 200mg, 1 2X/day, Zithromax 250 mg 2X/day, and nystatin 500,000 U 2X/day +/- Septra DS 1 2X/day is one effective combination. Mepron, Malarone, and/or herbs can be layered onto this regimen for severe symptoms or resistance.
Coartem can be used alone or with Daraprim 25mg, 2 daily for three days in the severely ill and/or in combination with doxycycline.
*He recommends lowering the parasitic load by rotating the drug regimens.
*Another “standard,” used by LLMD’s is using a three weeks on, one week off Babesia medications.
Alternative Treatments:
Artemisinin, Cryptolepis, Neem, Sida acuta, Alchornea cordifolia,
Red Root, Ailanthus, Yarrow, Cat’s Claw, Stephania,
Curcumin, Bidens, pilosa, Astragalus, L-Arginine, Heparin
http://aac.asm.org/content/48/1/236.full.pdf
Similarly with Bartonella, some respond miraculously to Heparin, which is a blood thinner. In the above link, heparin was found to inhibit Babesia growth. Horowitz also found it helps clear the parasites from the body.
*According to Buhner, (2015) Babesia infection depletes the body of arginine. Supplementing with L-arginine counters this, but it also helps the endothelial cells to produce NO (nitric oxide), a potent innate antimicrobial substance. He states that studies have shown that just supplementing with L-arginine in itself will reduce or eliminate Babesia.
http://buhnerhealinglyme.com Master Herbalist, Stephen Buhner’s Babesia protocol: take 1/4-1/2 tsp of each 3X/day (Source: Woodland Essence)
Sida acuta
Cryptolepis
Alchornea cordifolia or
C.S.A. Formula (Crypto, Sida, and Alchorn blend) – 1/4-1/2tsp 3X/day
*You can also add Artemisinin tablets to hit all angles
**Artemisinin has been found to fight Mycobacterium tuberculosis by attacking a molecule called heme found in the Mtb oxygen sensor which stops the disease’s ability to sense how much oxygen it is getting, prohibiting it from becoming dormant in response to a low oxygen environment. The use of Artemisinin for Mtb is hoped to shorten the course of therapy because it can clear out the dormant, hard-to-kill bacteria. http://www.nature.com/nchembio/journal/vaop/ncurrent/full/nchembio.2259.html
https://www.springboard4health.com/notebook/nutrients_artemisinin.html Dr. Rowan reports that Chinese researchers claim Artemesia’s success against Malaria is due to a peroxide linkage in its active molecule which kills the malarial parasite due to the excess iron that accumulates in the parasite which eventually become free, allowing the artemisinin to work like a bomb against the parasite. Dr. Singh found 100% of breast cancer cells in vitro were killed in hours by Artemesia: https://www.spandidos-publications.com/10.3892/ijo.18.4.767
Artemisinin has anticancer activity in a wide variety of laboratory cultured cancer cells, but shows no resistance.
Read the Dr. Rowan’s springboard link above for more information about cancer therapies. He recommends the Allergy Research Brand of Artemisinin http://www.allergyresearchgroup.com/quality-artemisinin, which is what my husband and I used with great success against Babesia along with Mepron and Azithromycin. http://www.nejm.org/doi/full/10.1056/NEJM200011163432004. Even though it appears to have cured Babesia in 3 months (no parasites seen in microscopy) in the research, it is a tenacious pathogen which Dr. Horowitz says is the worst coinfection he deals with. Since it is persistent many recommend treatment of 9 months to a year.
Mepron, or liquid gold, is expensive. ($800-$1,200 per bottle last I checked). To apply for a patient assistance program: https://www.rxresource.org/prescription-assistance/bridges-to-access.html (Income and tax info required)
Research is still pending on ELQ: https://madisonarealymesupportgroup.com/2016/12/05/babesia-cure-update/ If you hear the results before me, please contact me with the information.
We used the 3 weeks on, 1 week off approach. I too recommend the Allergy Research Brand of Artemisinin (I have no financial interests). It’s very powerful. We took 500mg twice a day. I had herxes that felt like heart-attacks and it gives you a metallic taste in your mouth. We did pulse ART MWF so it gave me a chance to recover in between doses and boy was I thankful for that.
Along with the pulsed artemisinin, we took Mepron daily 750mg 1-2 tsp 2X/day, with a high fat meal as well as pulsed an intracellular drug that worked against both Babesia as well as Lyme. We also pulsed in Tinidazole on TH and FR as well as diflucan 1-2 times a week to mop up any yeast.
Regarding Tinidazole: https://www.dovepress.com/evaluation-of-in-vitro-antibiotic-susceptibility-of-different-morpholo-peer-reviewed-article-IDR Metronidazole led to reduction of spirochetal structures by ~90% and round body forms by ~80%. Tigecycline and tinidazole treatment reduced both spirochetal and round body forms by ~80%–90%. In terms of qualitative effects, only tinidazole reduced viable organisms by ~90%. Following treatment with the other antibiotics, viable organisms were detected in 70%–85% of the biofilm-like colonies.
For a great article on air-hunger, a common Babesia symptom: https://madisonarealymesupportgroup.com/2018/03/22/what-is-air-hunger-anyway/ My husband and I also had chest pressure/pain and dizziness. I felt like a vice was squeezing me like a giant bear hug around my arms and chest. (Imagine someone picking you up by grabbing around your arms and lifting you up – only it never let up)
Babesia is no simple pathogen and coupled with Lyme and/or other coinfections like Bartonella, Mycoplasma, and various viruses it’s one tough mother. I want to offer hope here as both my husband and I treated this for a solid year and have NO Babesia symptoms. We have been symptom-free from Babesia for years now with no relapses. Experience has shown me that Dr. Horowitz is spot on by stating Babesia needs a solid 9-12 months of treatment. I’ve also heard that once you start treating for it, you should continue until you are finished because stopping part way through makes it tougher to treat in the future.