Healing Lyme Summit 2.0
|
|

|
|
https://www.lymedisease.org/missouri-bill-ags-and-lyme/
By Meg Muckenhoupt
3/27/25
Missouri State Representative Matthew Overcast, Esq. has introduced a bill to add alpha-gal syndrome (AGS) and Lyme disease to that state’s list of mandatory reportable conditions.
AGS is an allergy to red meat and meat-related products that is triggered by a tick bite.
HB 986 also requires the Missouri Department of Health and Senior Services to submit annual reports on the incidence of AGS and Lyme disease to the federal Centers for Disease Control and Prevention.
Overcast says that alpha-gal syndrome profoundly impacts many individuals and families in his district. However, he needs hard data to persuade his fellow legislators to help solve this problem.
Many states at the epicenter of the AGS explosion don’t even mention AGS in their information about tick-borne diseases. If they do mention AGS, they don’t give a figure for the number of cases. Thanks to research by the US military, though, we can estimate the number of AGS cases in several states. That number is frighteningly large.
By testing the blood of 3,000 recruits for the allergic antibody to alpha-gal, researchers were able to identify AGS hot spots. In the most impacted states–like Arkansas, Oklahoma, Missouri, and Kansas–more than 20% of recruits tested positive. In some areas of these states, almost half the recruits had the antibody.
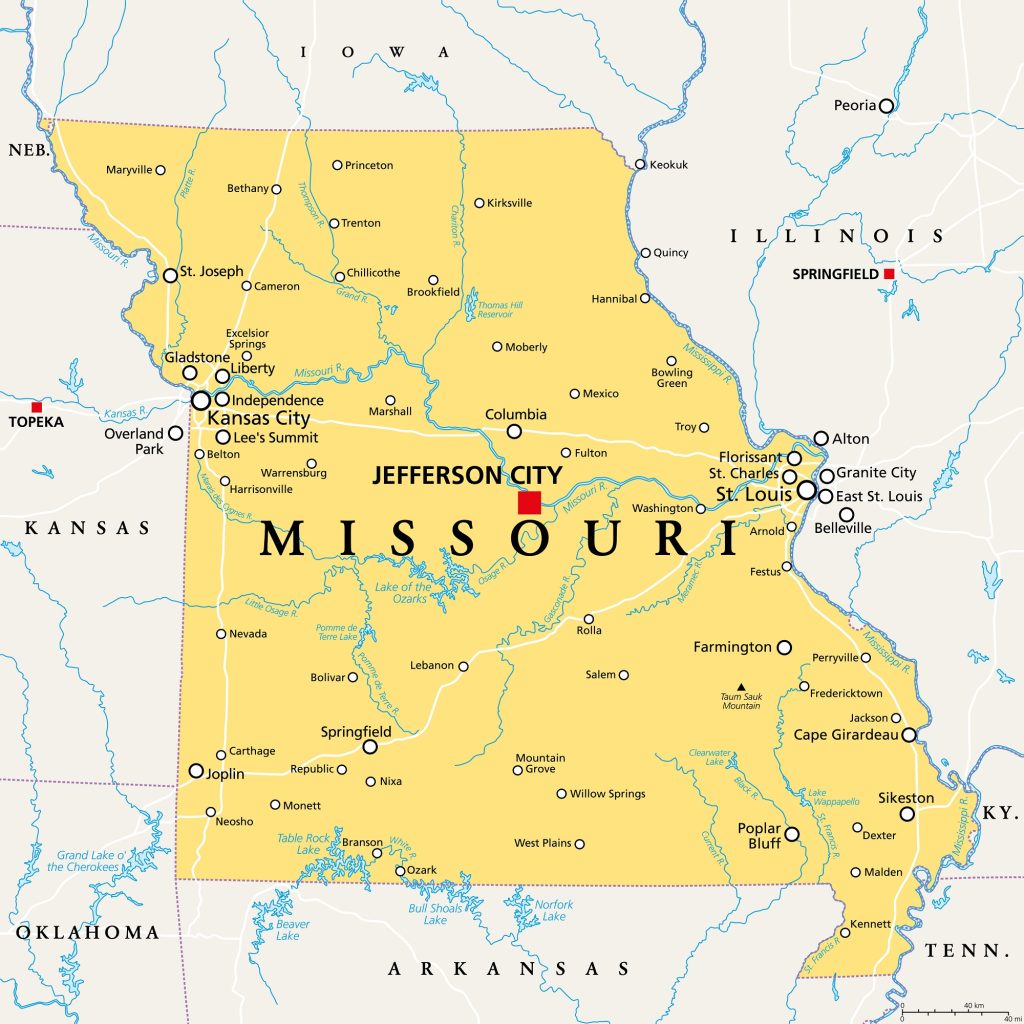
In Missouri, almost 30% of recruits had the alpha-gal allergic antibody. Extrapolating from this data, an estimated 80,000 Missourians may have AGS.
Documenting the extent of AGS and Lyme disease and tracking their expansion is the first step in attracting the public health resources needed for provider education and other help for people with AGS and Lyme.
If you are a Missourian affected by AGS and/or Lyme disease, please contact your state representative now to help pass HB 986.
Meg Muckenhoupt works with Alpha-gal Information, an Alpha-gal Alliance project.
For more:
https://www.medrxiv.org/content/10.1101/2025.03.03.25323258v1
Abstract
Lyme disease (LD) is an illness caused by the spirochete Borrelia burgdorferi (B. burgdorferi). Borrelia is known to disseminate through organs, including the skin, joints, spinal cord, bladder, and heart, leading to Lyme arthritis, neuroborreliosis, and Lyme carditis. While previous studies have investigated the impact of LD on pregnancy in both mice and humans and have found the presence of B. burgdorferi in the uterus of mice, we studied the impact of LD on the non-pregnant female reproductive tract. We use a mouse model for LD and find an ongoing and severe infection of the reproductive tract of female mice, which persists up to 15-months post-inoculation. This infection results in uterine glandular cysts and endometrial hyperplasia as well as vaginal epithelial thickening, polymorphonuclear and mononuclear cell epithelial infiltration, and epithelial desquamation into the vaginal lumen. Strikingly, we find that age has an impact on the extent of gynecologic pathology such that aged female mice (1-year old) that are reproductively senescent have more gynecologic pathology with infection compared to young mice (15-weeks old) when infected for the same length of time. Using large-scale electronic healthcare record data, we report that LD additionally results in increased infection-associated risk of:
Underreporting of gynecological outcomes is pervasive throughout many different infectious diseases, and LD-associated gynecological pathologies may have been similarly underappreciated in the field. This work suggests that further study of the female reproductive tract and the effects of B. burgdorferi infection therein will help clarify and expand the knowledge of myriad LD outcomes.
For more:
Please see the following inquiry that will most likely go unanswered. Note that Dr. John Aucott is a coauthor of this study who often says he believes in chronic Lyme disease but only at Lyme disease events held by advocacy groups.
———- Original Message ———-
From: CARL TUTTLE <runagain@comcast.net>
To: “aghirsch@geisinger.edu” <aghirsch@geisinger.edu>
Cc: “aejustice1@geisinger.edu” <aejustice1@geisinger.edu>, “cmnordberg@geisinger.edu” <cmnordberg@geisinger.edu>, “nsjosyula@geisinger.edu” <nsjosyula@geisinger.edu>, “jaucott@jhmi.edu” <jaucott@jhmi.edu>, “alison.rebman@gmail.com” <alison.rebman@gmail.com>, “bschwar1@jhu.edu” <bschwar1@jhu.edu>, “bmcinfectiousdiseases@biomedcentral.com” <bmcinfectiousdiseases@biomedcentral.com>, “irina.masalagiu@springernature.com” <irina.masalagiu@springernature.com>, “rauf.bhat@springernature.com” <rauf.bhat@springernature.com>
Date: 03/01/2025 12:04 PM EST
Subject: A comparison of genome-wide association analyses of persistent symptoms after Lyme disease, fibromyalgia, and myalgic encephalomyelitis – chronic fatigue syndrome
A comparison of genome-wide association analyses of persistent symptoms after Lyme disease, fibromyalgia, and myalgic encephalomyelitis – chronic fatigue syndrome
https://bmcinfectdis.biomedcentral.com/articles/10.1186/s12879-024-10238-x
Annemarie G. Hirsch, Anne E. Justice, Amy Poissant, Cara M. Nordberg, Navya S. Josyula, John Aucott, Alison W. Rebman & Brian S. Schwartz
To: Annemarie G. Hirsch, Corresponding Author
I read your manuscript with great interest and wanted to share a comment on your article I received from a fellow researcher who has experienced first-hand the devastation of Lyme disease. I added HTML links (references) to his statement and included my own comment. Additionally, I have a question for you and your co-authors.
Comment received:
“With respect may I say as Lyme and PTLD victim, Borrelia has the following characteristics:
Or, maybe it’s as the authors claim that PTLD is associated with:
“Our top index single nucleotide polymorphism (SNP), rs77857587, is in high linkage disequilibrium with a long-range protein quantitative locus SNP, rs111774530, for the MARC2 (Mitochondrial Amidoxime Reducing Component 2) protein.”
Carl Tuttle’s comment:
If I’m interpreting his comment correctly, it would appear that we have been dealing with an antibiotic resistant/tolerant superbug and essentially, “the emperor has no clothes.”
Question:
What academic discipline would you encounter if your department acknowledged chronic Lyme disease and began focusing on finding effective antimicrobial treatments for all borrelia forms; round body, biofilm etc.?
A response to this inquiry is requested.
Carl Tuttle
Independent Researcher
Hudson, NH
Cc: Rauf Bhat, Senior Editor
Stefan Baral, Senior Editorial Board Member
Letter to the Editor of the BMJ published June 2020
https://www.bmj.com/content/369/bmj.m1041/rr-1
(It should be noted that the corresponding author refused to reply after repeated requests by BMJ Editor Fiona Godlee)
For more: