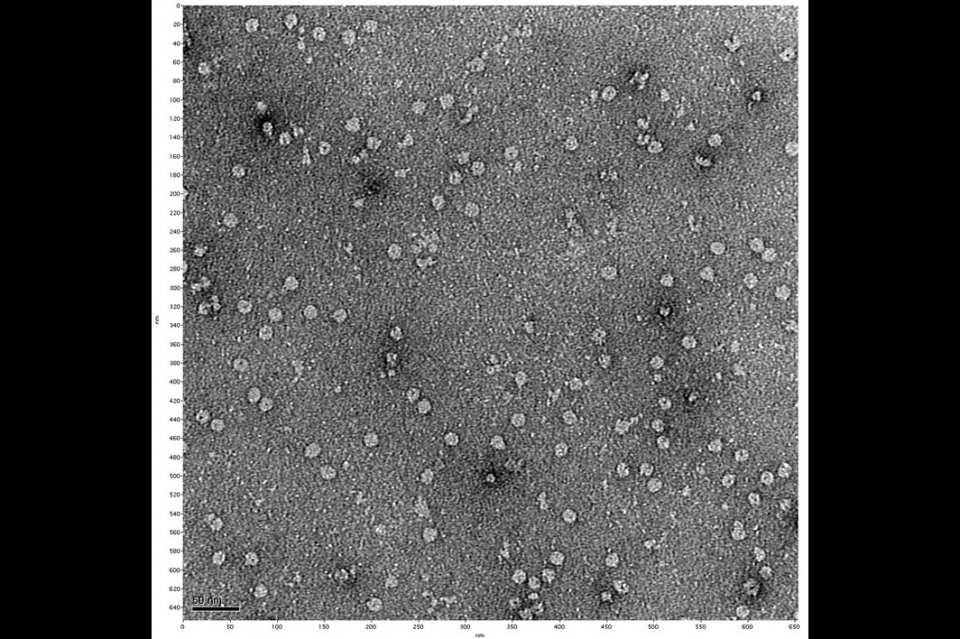
Toxoplasma gondii, an intracellular protozoan organism, is a very “successful” parasite with extremely diverse host base and sophisticated, almost diabolical, methods of survival and proliferation.
It is found worldwide and is capable of infecting most warm-blooded animals as intermediate hosts, including people. It has also been found in some cold-blooded animals, such as fish. Its final hosts, inside which the parasites can sexually reproduce, are felines, including domestic cats. In the environment, toxoplasma can be found in soil, water, and other substances that have come in contact with the parasite, such as fertilizers.
At the moment, the predominant medical opinion is that at least one third of all people on Earth are in some way infected with this parasite1,2 averaging from 11-20% in the United States to 50% or higher in a number of Western European countries, for example in Germany.3 In Germany, the frequency of positive Toxoplasma detection increases from about 20% in the group of 18-29 year-olds, up to 77% in the group of 70-79 year-olds and for over 79 year-olds the frequency is 84%.4
The commonly known infection routes for people are eating uncooked meat, drinking contaminated water, or accidentally ingesting the parasite after cleaning a cat litter box.
While the official word is that most infections are harmless and asymptomatic, the impact of the parasite could be much more devastating than the current mainstream medical convention gives it credit for.
A few physicians and researchers who have been looking into Toxoplasma are challenging the conventional view on several counts. And while a number of “bombshell” scientific works on the topic have been published, the new discoveries have not yet made their way into the everyday medical practice.
It is extremely important that more doctors and researchers look into this right now — especially given the fact that an encounter with the spike protein has been shown to amplify latent or slow-developing biological malfunctions in people, and thus it is possible that “spike protein assisted” Toxoplasma may be wreaking havoc in many unsuspecting patients and contributing significantly to the mysterious “long COVID” or its injection-induced manifestation.
Toxoplasma Life Cycle
With a degree of oversimplification, there are three main forms in which this parasite exists during different phases of its life cycle. They are known as oocysts (eggs), tachyzoites (the actively proliferating adult form), and bradyzoites (tissue cysts).
The sexual reproduction of Toxoplasma gondii occurs within feline hosts. The cycle starts when the host ingests oocysts (“eggs”) or eats an animal infected with bradyzoites (tissue cysts).
Upon ingestion of the cysts, their protective wall is dissolved by proteolytic enzymes in the stomach and small intestine to release bradyzoites. The free bradyzoites then penetrate epithelial cells lining the small intestine where they proliferate to form new generations that can undergo sexual and asexual cycles. Following fertilization of the female gametes, a wall starts to form around the oocysts. The oocysts are then released to the environment along with feces.
Depending on the environment, it usually takes several days for the oocysts in feces to become infectious. Infectious oocysts can survive for up to several years in soil etc., until they are ingested by an intermediate host. Once they are ingested, their protective shield is also dissolved by proteolytic enzymes thus releasing the eggs into the intestine of the intermediate host.
They then penetrate epithelial cells lining the small intestine where they undergo a form of asexual reproduction to form tachyzoites. The newly formed tachyzoites then spread and actively penetrate other cells of the intermediate host where they are surrounded by a parasitophorous vacuole protecting them from the hosts’ immune system.5
The interesting thing about the parasitophorous vacuole is that the parasite uses a part of the membrane of the invaded host cell’s to form it, with the purpose of “hiding” from the host’s immune system.6
From there tachyzoites disseminate throughout the body and reach immunologically protected sites including brain, retina and fetus. In vitro studies revealed that tachyzoites can invade astrocytes, microglia and neurons of the mouse brain with subsequent formation of tissue cysts within these cells.7,8,9,10,11
As they continue dividing, tachyzoites ultimately cause the cell to break, releasing as many as 32 tachyzoites that then infect new cells. However, that activity usually attracts the attention of the immune system, which ultimately slows down tachyzoite multiplication. In response, the tachyzoites convert into bradyzoites (tissue cysts).12
In doing so, they change their surface structure nearly completely, which is a “major factor in the parasite’s strategy of survival” since the host’s immune system identifies microorganisms according to their surface structure, and by modifying its surface structure, toxoplasma increases its chance of successfully tricking the host’s immune system.13,14,15
The tissue cysts are common in a number of body tissues and organs including the eyes, cardiac muscle, neural tissue, and various visceral organs where they can last for the hosts’ entire lifetime.16
Houston, We Have a Problem
The general medical consensus (challenged by a small group of doctor and researchers) is that while the most active form of Toxoplasma, known as “tachyzoites” (the one that multiplies very fast and blasts host cells), can cause significant health issues, predominantly in immunocompromised hosts, the tissue cyst form (“bradyzoites”) is mostly innocuous, and, once the parasite succumbs to the attack by the host’s immune system and retreats into its tissue cysts, it just quietly sits inside those intracellular cysts and does very little.
Per mainstream medial convention, the vulnerable demographics are immunocompromised patients who can succumb to acute toxoplasmosis and develop potentially lethal inflammation of the brain (or become victims of a “reactivation,” where tissue cysts convert back to the fast-proliferating form, to the same effect), and newly infected pregnant women.
However, recent research has shown that bradyzoites, the toxoplasma tissue cysts, are not innocuous at all, and that they do reproduce inside the cysts and can cause inflammation and other issues without converting to tachyzoites, including in otherwise immunocompetent patients.
What complicates the issue even further is that nearly all commercially available tests (antibody blood tests and even PCR tests), are specific to the cell-blasting tachyzoite form of toxoplasma and do not detect the presence of tissue cysts.
And if that is the case — we are looking at a potentially large number of people ailing from “chronic active toxoplasma” that cannot be diagnosed by any of the commonly used methods. As a result — especially given that toxoplasma loves living in the brain — their very real and possibly exhausting physical disease may be classified or psychosomatic or straight out psychiatric.
They could be suffering from slow-developing brain inflammation, autism-like symptoms, dementia-like symptoms, or even pulmonary and heart issues — and the doctors might not even be looking in the direction of toxoplasma or ruling it out, based on negative antibodies.
(In its active form, the parasite has been implicated in ocular issues,17 heart disease,18 pneumonia,19 recurrent headaches,20,21 even cancer22 — as well as in addiction, schizophrenia, epilepsy, Alzheimer’s disease, and various neurological disorders.23,24,25 And even in its latent form, it is believed to cause psychological changes in its hosts, ranging from entrepreneurial26 to suicidal tendencies.27
Among the researchers doing groundbreaking research in Toxoplasma are Dr. Jaroslav Flegr in the Czech Republic, Dr. Robert Yolken and Dr. Vernon Carruthers in the U.S., Dr Uwe Auf der Straße in Germany, and others.
The Work of Dr. Uwe Auf der Straße in Germany
Dr Uwe Auf der Straße is a GP in Germany and the author of the book titled, “Shadow Disease Chronic Active Toxoplasmosis.”28 Here is what he has to say about the “limits of our current laboratory medicine”:
“The current medical opinion is still that a negative IgM excludes an active toxoplasmosis and thus the need of a therapy. Due to research having hinted repeatedly of a significant effect of bradyzoite activity, and due to my own observations, I definitely cannot agree with that.
Tests only react to tachyzoite-specific antibodies and the sensitivity of a standard test system in case of an initial infection is only 81.8%.29 Basic research has done further substantial work which questions the accuracy of Toxoplasma antibody assays.
‘The currently available solid phase immunoassays were developed in the 1970’s to detect strains which were circulating at that time and there are strong indications, that … standard assays may substantially underestimate the prevalence of Toxoplasma infection in a population and its effect on health and disease.’30
Further it has been proven that, in cases of a Toxoplasma infection, tachyzoite–specific IgG, IgM and even PCR can render negative results.31,32,33
In a chronic active course of the disease, reliability of our currently used lab methods has not been proven and these are most likely not suitable to detect Bradyzoites or their activity, let alone the cyst burden.
Research still focuses predominantly on acute rather than chronic toxoplasmosis and it is only a general assumption, that cases with chronically active courses of the disease as presented here could be diagnosed by using the usual antibody assays – to my knowledge this has never been proven.
The number of Toxoplasma carriers without detectable tachyzoites antibodies, who can potentially become ill from a chronic active toxoplasmosis based on an increased activity within the cysts is unclear.
From my observations it can be assumed that the number is significant, otherwise there would not appear so many younger patients in my case collection (about 40%), who suffer from a chronic active toxoplasmosis without any detectable tachyzoite antibodies.
If the immune system ceases to produce Tachyzoite antibodies after some years, the disease will no longer be detectable in the blood. This does not mean that the Toxoplasma in the cysts are inactive.
There are numerous indications that an increased activity in the cysts can trigger a symptomatic illness, since, contrary to older assumptions, bradyzoites do not rest, but can be active and can reproduce and cause illness. This refers to the findings of Fergusson et al. (1989), McLeod et al. (2008) and Watts et al (2015).”34,35,36
Dr. Uwe Auf der Straße has observed that there was no significant difference in observed symptoms between his patients with positive antibody tests and his patients with negative antibody tests in whom he suspected chronic active toxoplasmosis, based on the preliminary diagnostic method he developed and ruling out other illnesses that can produce similar symptoms. (He also took into consideration their positive reaction to toxoplasma therapy.)
“I am convinced that a significant activity within the cysts, predominantly of the bradyzoites, is the decisive reason for the illness in both groups of patients who all have inconspicuous IgM values with regards to tachyzoites, and whose IgG values, if indeed there are any, don’t show any direct correlation to the severity of the illness.
The clinical pictures in both groups are identical, and the toxoplasmosis therapy is even more effective in group B [negative antibody tests]. The bradyzoites, the activity of which we cannot measure, are currently underrated strongly, and our established laboratory values produce only a pretended security.
It is difficult to develop reliable bradyzoite-specific tests, since bradyzoites reveal themselves only rarely to the immune system and only lead to a limited antibody production.”37
“Thankfully, basic research has begun to address this problem, and there are new and promising methods being developed, with the aim of getting a grip on this problem and reveal hitherto not detectable toxoplasma presence and even to determine the cyst burden.”38
Toxoplasma and the Mind
According to Kathleen McAuliffe, author of the book “This Is Your Brain on Parasites,”39 researchers have noticed a strong correlation between toxoplasma infection and schizophrenia and other mental disorders in humans. She also notes studies where anti-psychotic drugs inhibited toxoplasma in vitro.
In fact, the mind-controlling ability is Toxoplasma’s “trademark.” I wrote about it earlier in the article titled, “Don’t Underestimate Mind-Controlling Parasites.”
To quote Dr. Uwe Auf der Straße again, whose book I can’t recommend enough, “symptoms comprise an increased risk for the occurrence of schizophrenia40,41,42,43 psychoses44 or aggressive behaviour, also a doubling of the risk for accidents in cases where Toxoplasma antibodies have been detected.45
Explanations for that may point to the mentioned behavioural changes and the decreasing psychomotor resilience46 due to Toxoplasma infections. It is scary that even an increase in the number of attempted suicides has been correlated with antibody detection in toxoplasmosis.”47,48
“It fits this bill that toxoplasmosis infected rats are known to lose all fear of cats. They literally seek them out in broad daylight, to be eaten in the end, a behaviour that is very advantageous for the spreading of Toxoplasma, but not so good for the rat. The consequence is clear.
When the host is ‘ripe’ and contains many bradyzoite – cysts, it is simply more useful for the parasite when dead instead of alive, particularly if the death is caused by a cat. Death by car accident or suicide are thus somehow “inappropriate”, but can be regarded as a somewhat macabre continuation of such behavioural disturbances in the present.”
Many Tricks of Toxoplasma
The tricks of this parasite are endless. For example, it knows how to hijack the host’s macrophages — and instead of being destroyed by a macrophage,49 take over it and use it as a temporary home to transform into the active form and then use it as a cab to travel around the host’s body!
According to the accepted view, the release of actual “eggs” from the ingested oocysts into the host’s system happens due to the processes in the host’s digestive system. However, a study came out showing that the process can happen in the absence of digestive factors, and that the parasite can not only survive but also transform into its most active form inside macrophages, after being “eaten”:
“Our results show that the oocyst internalization kinetics can vary among a given population of macrophages, but similar processes and dynamics could be observed. Most of the cells manipulate oocysts for ~15 min before internalizing them in typically 30 min … Liberated sporozoites within macrophages then differentiate into tachyzoites within 4-6 h following oocyst-macrophage contact.”
Another paper, titled, “Inhibition of nitric oxide production of activated mice peritoneal macrophages is independent of the Toxoplasma gondii strain,” shows that Toxoplasma is capable of inhibiting nitric oxide production. Nitric oxide, that plays an important role in immune response50,51 and is frequently mentioned in the context of COVID.
It’s an “enzyme that is expressed in activated macrophages, generates nitric oxide (NO) from the amino acid L-arginine, and thereby contributes to the control of replication or killing of intracellular microbial pathogens.”52
The overall mechanism that the parasite uses to invade host cells is beyond of the scope of this article but if you are curious, you can check out the paper titled, “How does Toxoplasma gondii invade host cells?” If you want to learn more about how it modulates host cell’s responses, there is another technical paper titled, “Toxoplasma gondii Modulates the Host Cell Responses: An Overview of Apoptosis Pathways.”
And if you want to learn more about Toxoplasma and brain blood barrier, you can read this paper, “Toxoplasma gondii and the blood-brain barrier.”
Toxoplasma and the Spike Protein: A Possible Connection?
According to Dr. Uwe Auf der Straße, a patient could be potentially simultaneously infected with Toxoplasma and with one or more other pathogens, some of the them kicking in as opportunistic infections.
In that case, the clinical picture may be even more confusing, and the condition of the patient may be more severe, even though Toxoplasma is capable of causing enough trouble if it manages to sufficiently proliferate — whether in its active form or inside the tissue cysts — all on its own.
Dr. Uwe Auf der Straße’s book was published in 2019, so there is nothing about COVID in the book — but it is not illogical to presume that when a person with latent or relatively slowly developing Toxoplasma encounters the spike protein, whether it’s from infection or from the COVID injection, it may create a “perfect storm” and kick Toxoplasma in high gear, creating debilitating and/or mysterious symptoms, resulting in vaccine injury or “long COVID.”53
If the percentage of people with chronic active Toxoplasma is as high as Dr. Uwe Auf der Straße suspects, it is also not illogical to assume that due to the deficiencies in the current diagnostic standards and tools, a lot of people suffering from chronic active Toxoplasma may not be properly diagnosed, and their maladies may be attributed to psychosomatic factors or remain a medical mystery.
An additional complication is that “atypical mixed forms of the known Toxoplasma strains, which are significantly more aggressive than the previously known Toxoplasma strains have been detected in Germany, and this might happen worldwide.”54,55,56
Anecdotally, per Dr. Uwe Auf der Straße, patients with chronic active toxoplasma could experience increased irritability where they “blow up” out of nowhere even though they realize that there is no good reason and don’t feel good about being so irritable — as well as anxiety or depression, with men more prone to irritability, and women more prone to anxiety and depression.
At the same time, also anecdotally, increased irritability has been observed in some recipients of the COVID injection. And while there can be lots of factors causing mood changes, it could be something to look into.
Curiously, there is an overlap between the list of natural remedies that have been studied as potentially treatments against toxoplasma and showed improvements — and the list of “alternative” COVID and “long COVID” treatments.57,58,59,60 Due to the tremendous complexity of the issue and the fact that myriads of factors impact our immune response and reactions to treatments, further investigation of the correlation by honest and curious is urgently needed.
Conventional toxoplasma treatments are considered effective in treating tachyzoites but there is no known conventional treatment for the tissue cyst form.61
Better Diagnostics: Some Hope
According to Dr Uwe Auf der Straße, in his practice, he found one particular testing method to be more reliable than the conventional ones:
“The Lymphocyte-Transformation-Test (LTT) has made my work on Toxoplasmosis easier in the last months, but is not (yet) used for the diagnose of toxoplasmosis on a wider scale. By means of this test, we can detect activity of our immune system’s T-lymphocytes, which react specifically towards certain pathogens.
While the immune system is dealing with certain pathogens, T-lymphocytes become specifically reactive to this pathogen, and the intensity of this reactivity can be measured pathogen-specifically.”
“This is measurable for about 4 weeks, and thus the LTT mirrors the current activity of pathogens. A more than threefold elevated stimulating index (SI) indicates, that specific T-cells are present in the blood and thus an active confrontation of the immune system and the tested germ takes place.
A validation concerning chronic active toxoplasmosis has not yet been performed, but according to both Dr. Hopf-Seidel and my own experiences with patients suffering from a chronic active toxoplasmosis, it is most likely more sensitive than the Toxoplasma IgM.”
Dr Uwe Auf der Straße also speaks highly of the work of Dr. Yolken’s team:
“I consider a new approach of the scientific group led by Professor Yolken in Baltimore to be promising. A paper on this approach has been published in June, 2018.62 The scientists used a known detection method (a Western blot test) for the detection of Toxoplasma proteins, which also give proof of the presence of Toxoplasma.
Of 25 patients, who were suffering from severe psychic disorders, 3 patients (8.2%) were diagnosed as positive with Toxoplasma IgG. Four times as many, 12 patients (35.3%) were then diagnosed with Toxoplasma by detection of Toxoplasma protein in their blood.
The detection of these proteins seems to offer a significantly more sensitive method to diagnose toxoplasmosis than the usual available antibody tests. Until this can be used as a routine procedure, the tests will have to be examined in further studies.”
“The same group of scientists is currently developing another highly-sensitive method, which can detect Toxoplasma cysts in every stage of the disease. This concerns the MAG1 antigen, which occurs in great numbers inside the bradyzoite cysts and in their outer membrane. Antibodies which are directed against this MAG1 antigen can be detected in the laboratory.
The scientist could prove in mice that the amount of MAG1 antibodies detectable in the blood showed a significant correlation to the amount of bradyzoite cysts inside the brain. It was also shown that in case of negative MAG1 antibody detection, no bradyzoite cysts were found.
This marker could possibly be used as a scale for a chronic infection and for the burden with bradyzoite cysts in the future. This would be a huge step for laboratory diagnostics and for affected patients even more so.”
“Another approach is that clues for a disturbed metabolism in patients with Chronic Fatigue Syndrome (CFS) are being investigated intensively. In 2016 it was proven that CFS patients share anomalies in 20 metabolic pathways of their mitochondria.63 One might picture mitochondria best as our cells’ power plants.
The intensity of the illness in CFS patients negatively impacts the activity of the metabolic pathways and the quantity of metabolites, which result from the mitochondria’s work. This “shutdown” of the metabolism has been interpreted as a shifting of the mitochondrial metabolism into “survival mode.”
Toxoplasma can also very severely affect the mitochondria,64 and the intensity of affliction is probably related to the strain of Toxoplasma which has infected the patient.65 It would be of utmost interest if the deviations in mitochondria metabolism during a chronic active toxoplasmosis might resemble those detected in ME/CFS patients, as there is strong overlap in the symptoms of both diseases. They might even be identical in some cases.”
Conclusion
It is possible that due to imperfect diagnostics and insufficient understanding of this parasite in the medical community, a lot of people with chronic active toxoplasma remain undiagnosed or diagnosed incorrectly, and suffer profoundly from the lack of proper treatment.
It is also possible that Toxoplasma is a significant factor, contributing to complications from spike protein toxicity. I believe that understanding this issue is important. It requires time and attention of researchers and doctors, and my prayer is for solid knowledge to come, and for the “mystery” suffering to end.
About the Author
To find more of Tessa Lena’s work, be sure to check out her bio, Tessa Fights Robots.
___________________
For more:
Toxoplasmosis causes many mental issues and psychiatrist E. Fuller Torry believes that 75% of schizophrenia is associated with infections, with Toxo a significant portion. https://madisonarealymesupportgroup.com/2016/05/21/toxoplasmosis/