Dr. Rawls’ Lyme Treatment Guide
https://rawlsmd.com/treatment-guide
Dr. Rawls’ Lyme Treatment Guide
A-to-Z Lyme Treatment Ratings: From antibiotics to herbal therapy, ozone, and more, find out how Dr. Rawls rates these popular Lyme disease treatments.
As a physician, I often get asked my opinion on various Lyme treatments. While herbal therapy is my preference for the majority of those with chronic Lyme disease, I’m always learning and educating myself on different treatments and therapies that might make it easier for people to get their lives back. Based on my research, experience, and medical opinion, I developed a rating system to evaluate potential treatment options according to safety, efficacy, and cost.
Dr. Rawls’ Lyme Treatment Guide
More Treatments Coming Soon!
In the coming weeks, look forward to treatment additions like colloidal silver, essential oils, stevia, IVIG, methylene blue, peptides, and SOT therapy.
Sign up for our RawlsMD newsletter to find out when new treatments are added.

To evaluate the potential success and pitfalls of various treatments, I use a grading system based on my research, experience, and medical opinion. My criteria includes:
-
- Cost: What are the out-of-pocket expenses for a particular treatment?
- Efficacy: Is there any evidence the treatment works?
- Safety: What’s the potential for the treatment to cause harm to the person who’s using it?
- Ways to administer: What’s the route by which the treatment is given to a person?
Using my rating system, I’ve created a treatment guide so that you can learn about and compare a variety of treatments and therapies. You’re likely to hear some success stories with nearly every intervention or modality on this list. But measuring your options according to efficacy, potential risks, and cost, in partnership with your healthcare provider, will go a long way in helping you make the best decisions for you and your recovery.
Bill Rawls, MD
Medical Director and Cofounder of RawlsMD.com
Dr. Bill Rawls is a licensed physician with over 30 years of experience and a leading expert in Lyme disease, holistic health, and herbal medicine. In the middle of his successful medical career, Dr. Rawls’ life was interrupted by Lyme disease. In his journey to overcome it, he explored a wide range of treatments – from conventional medicine to an array of alternative therapies.
In the more than 10 years since his recovery, Dr. Rawls has helped thousands of patients to recover from chronic illness and maintain wellness. He is the author of the best-selling book Unlocking Lyme, and the Medical Director of RawlsMD.com and Vital Plan, an online holistic health company and Certified B Corporation®.
How to Overcome Chronic Lyme Disease
Aug. 1, 2018
Dr. Bill Rawls overcame chronic Lyme disease with herbal and natural remedies. He reveals the 5 essential elements for recovery here. Learn more about Lyme disease and Dr. Rawls’ story: https://rawlsmd.com/health-articles/m…
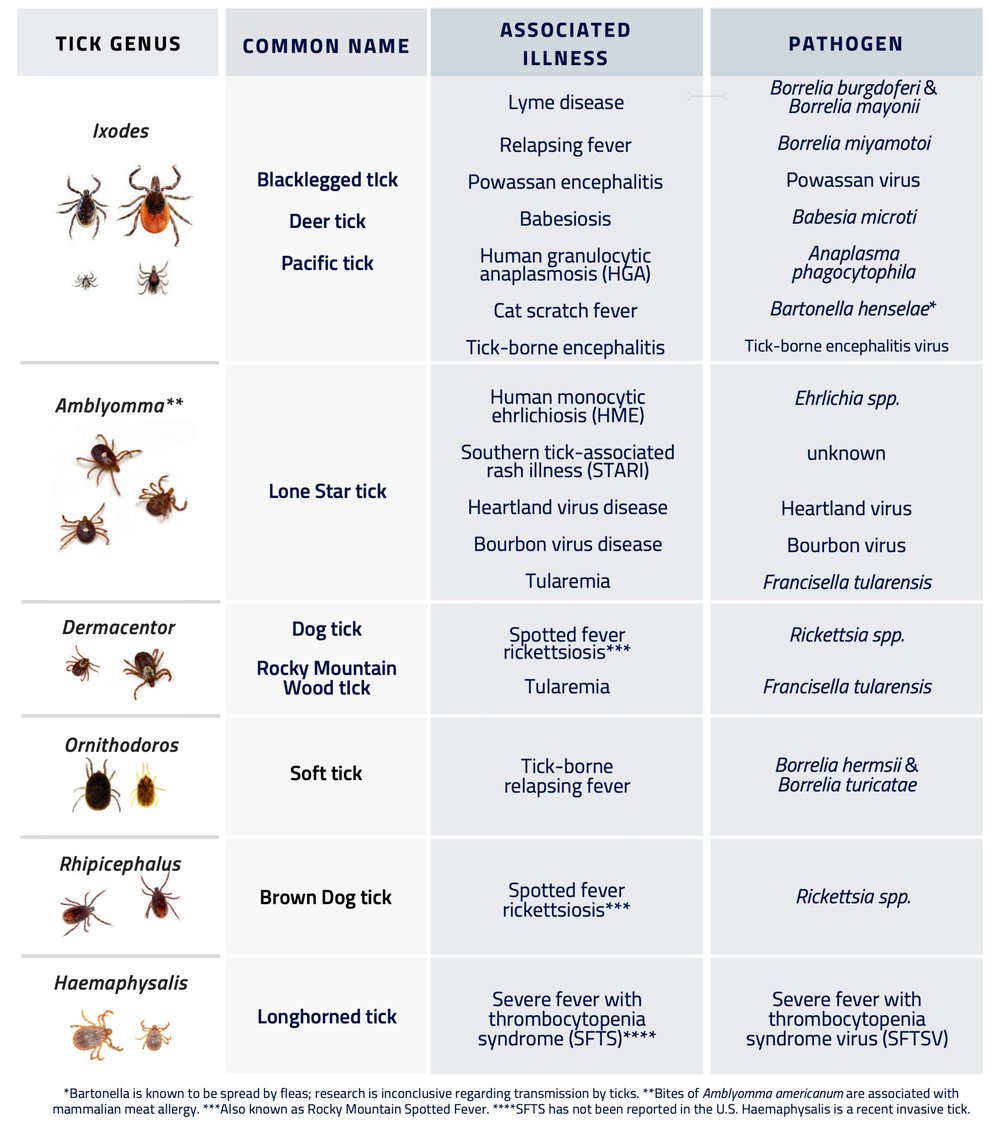
Dr. Rawls recently came out with a nifty coinfection chart worth looking at as well.
____________________
**Comment**
I would dispute a few items on the treatment ratings. I’ve done many of the treatments listed and have found antibiotics to be cheaper and more effective than herbal treatments for both myself and my husband. Dr. Horowitz has found that herbs alone have about a 70% success rate in his office (if I’m remembering correctly). Not many doctors write books on their clinical experience so when they do, I take note.
Please understand I’m not dissing herbs here – just talking brass tacks about money, time, and efficacy. I still use herbs to this day for various issues and know they have helped many patients, but to my knowledge there is no magic cure – including herbs, or I’d be using it. Savvy, layered treatment focused on all forms of borrelia and taking coinfections into account as well as detoxification, immune system imbalances, gut health, diet, exercise, sleep, stress, and more is crucial on this journey. It truly is as individual as the person.
For more:
- https://madisonarealymesupportgroup.com/2016/02/13/lyme-disease-treatment/ The latest kids on the block are disulfiram, the dapsone combination, and liposomal essential oils.
Many are having wondrous results with disulfiram, unfortunately I had to quit it as it caused psychosis for me (not fun, and a $30 drug ended up costing me $20K due to a week long hospital stay because I went completely nuts). Dr. Horowitz has also had good success with the triple Dapsone combination on some of his most refractory patients. I’ve heart there are many side-effects and the need to supplement to mitigate those effects, but for the right patients it may prove to be the thing that helps the most. Regarding liposomal essential oils, my husband and I are currently taking liposomal oregano oil in our Bartonella treatment of Clarithromycin/rifampin, along with garlic, monolaurin, and stevia. Time will tell on this treatment.
Go here to listen to Dr. Frid’s clinical experience using liposomal essential oils. (Unlike antibiotics, she finds LEO’s most effective when pulsed). I found them cheapest on her website.