New Hampshire Man Tests Positive For Jamestown Canyon & Powassan Viruses
DHHS: Kingston Man Tests Positive for Rare Viruses Carried By Ticks, Mosquitoes

Public Domain photo
NH health officials say protect yourself from mosquito bites.
“From spring until fall, New Hampshire residents and visitors are at risk for a number of different infections from the bite of mosquitoes and ticks, and this case highlights the risk from both,” said Dr. Benjamin Chan, State Epidemiologist.
“In addition to Jamestown Canyon virus and Powassan virus, there are a number of other viral and bacterial infections that can be transmitted by mosquitoes and ticks in New Hampshire, and we recommend that residents and visitors continue to take basic steps to prevent mosquito and tick bites in order to stay healthy.”
Jamestown Canyon virus is a mosquito-borne pathogen that circulates widely in North America primarily between deer and a variety of mosquito species, but it can also infect humans. First reported in the early 1970s, reports in humans are rare but have been increasing over the last several years. This is New Hampshire’s seventh case of JCV since the first report of the disease in 2013. Most reported illnesses caused by JCV have been mild, but moderate-to-severe central nervous system involvement has been reported.
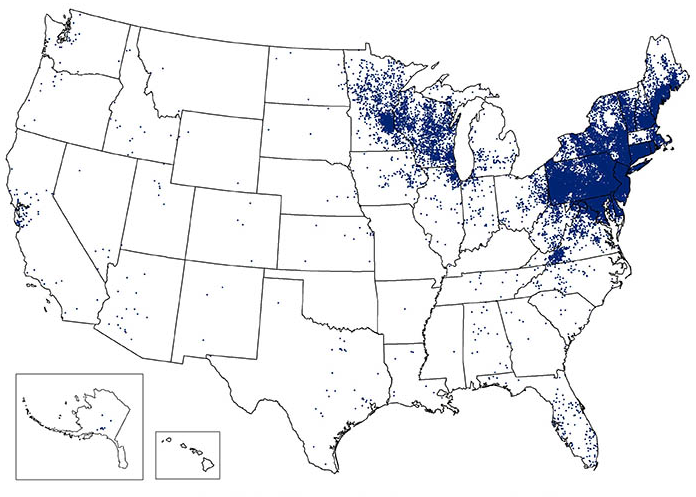
Powassan virus infection is similar to mosquito-borne viruses like JCV, West Nile virus (WNV), and Eastern equine encephalitis (EEE), but is transmitted to people by infected ticks. POW was identified as a cause of human illness in the late 1950’s. In the last decade, 144 cases of POW have been detected in the United States. This is New Hampshire’s fourth case of POW, also since 2013. In New Hampshire, the blacklegged tick is the most likely to transmit this virus to people. A tick needs to be attached to a person for only 15 minutes to transmit POW. Some people who are infected may experience mild illness or no symptoms. Powassan virus can also infect the central nervous system causing brain inflammation, which may be disabling or fatal.
The Kingston resident had no recent history of travel outside our state and spent a great amount of time outdoors. Residents and visitors to New Hampshire should protect themselves and their family members by:
· using an effective mosquito and tick repellant containing DEET (20-30%), Picaridin, or oil of lemon eucalyptus
· wearing protective clothing, tucking shirts into pants and pants into socks
· removing standing water from around your house so mosquitoes do not have a place to breed
· being mindful of tick habitat keeping grass cut short, and
· performing frequent and daily tick checks with immediate tick removal.
Vitamin B, ultrasonic devices, incense, and bug zappers have not been shown to be effective in preventing mosquito- or tick-borne diseases.
Other mosquito- and tick-borne illnesses that have been documented in New Hampshire include WNV and EEE from mosquitoes, and Lyme disease, anaplasmosis, babesiosis, and Borrelia miyamotoi from ticks. Biting mosquitoes will continue to be a disease concern until there are two, statewide, hard frosts. Risk of tick bites exists when temperatures are above freezing and ticks are not covered by snow.
People can be infected and not develop any symptoms, or only develop very mild symptoms. Early symptoms can include flu-like illness including fever, muscle aches, headaches, and fatigue. People infected with JCV, EEE, WNV, and Powassan can develop more serious central nervous system disease, including meningitis or encephalitis. If you or someone you know is experiencing flu-like symptoms, including fever and headache, contact your local medical provider.
Anyone with questions about vector-borne illnesses can call the DHHS Division of Public Health Services Bureau of Infectious Disease Control at (603) 271-4496 between 8 AM to 4:30 PM, Monday through Friday. More information can also be found online at www.dhhs.nh.gov and www.cdc.gov.
News story here: https://www.wmur.com/article/new-hampshire-adult-infected-with-jamestown-canyon-virus-powassan-virus/28647142
________________
**Comment**
Pathogens have a certain proclivity for their vectors. It’s always interesting to me to entertain the possibility that perhaps there is cross over.
For instance, borrelia has been found in mosquitoes and many patients claim to have become infected with Lyme after a mosquito bite:
https://madisonarealymesupportgroup.com/2018/11/07/are-mosquitoes-transmitting-lyme-disease/
https://www.ncbi.nlm.nih.gov/m/pubmed/26631488/ Excerpt:
…results show that DNA of Borrelia afzelii, Borrelia bavariensis and Borrelia garinii could be detected in ten Culicidae species comprising four distinct genera (Aedes, Culiseta, Culex, and Ochlerotatus). Positive samples also include adult specimens raised in the laboratory from wild-caught larvae indicating that transstadial and/or transovarial transmission might occur within a given mosquito population.
BTW: THE LAST STUDY ON THE POTENTIAL OF OTHER BUGS TRANSMITTING LYME (MINUS THE GERMAN STUDY ON MOSQUITOS) WAS DONE OVER 30 YEARS AGO. AND, WHILE NO SPIROCHETES WERE ISOLATED FROM THE HAMSTERS, ANTIBODIES WERE FOUND – EVEN BACK THEN.
Therein lies the hang up. The presence of antibodies does not prove infection. It’s interesting that the current CDC 2-tiered testing relies upon antibodies…..
The transmission of Bartonella from ticks is also still being quibbled about with some just stating emphatically that it is: https://madisonarealymesupportgroup.com/2016/01/03/bartonella-treatment/ while others take a more conservative approach and say the science isn’t settled: https://madisonarealymesupportgroup.com/2019/07/13/suspected-insect-and-arthropod-vectors-for-bartonella-species-galaxy/
This issue of what is being transmitted by whom seems to me to be a very important and practical issue. Why isn’t the science being done?
Also, while the media continues to inform us all of this is “rare,” please remember that many of these pathogens are not mandatorily reported, and we have no idea on prevalence. Coppe Lab out of Wisconsin emphatically states Powassan is NOT rare:
http://www.coppelabs.com/blog/why-is-powassan-virus-infection-still-described-as-rare-and-mysterious/ Please read the following excerpt by Coppe Lab here in Wisconsin,
For the last two years, Coppe Laboratories has dedicated a significant amount of time and resources to dispelling the myth that infection with Powassan virus, a virus transmitted by tick bite, is rare. The Centers for Disease Prevention and Control (CDC) reports only 100 cases of Powassan virus infection in the United States in the last 10 years. Indeed, that statistic gives the illusion that Powassan infection is rare. However, did you know that the only infections reported to CDC are those that are life-threatening, particularly cases causing severe inflammation of the brain like the case reported in LiveScience? Coppe has published three new papers in the last year that clearly show Powassan virus infection is not rare are at all,and until testing for this virus is included as part of tick-borne disease screening panels infections will continue to be underreported. Coppe’s Powassan Guide, which can be downloaded from the website, summarizes the findings from both tick and human Powassan prevalence studies, as well as defining the patient populations that would benefit most from Powassan testing.
To my knowledge, not only are there few current studies on what transmits what, but nothing has been done on transmission time when multiple pathogens are being transmitted concurrently. Everyone’s stuck on climate change….