Remember Deer Keds? Study Shows Bartonella Causing Deer Ked Dermatitis in Humans
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC525279/
Isolation of Bartonella schoenbuchensis from Lipoptena cervi, a Blood-Sucking Arthropod Causing Deer Ked Dermatitis
ABSTRACT
Bartonella schoenbuchensis, which commonly causes bacteremia in ruminants, was isolated from the deer ked Lipoptena cervi and was shown to localize to the midgut of this blood-sucking arthropod, causing deer ked dermatitis in humans. The role of B. schoenbuchensis in the etiology of deer ked dermatitis should be further investigated.
________________
**Important Take-aways**
- Deer Ked incidental infestation in humans is well documented
- Skin tests with deer red whole-body extracts were positive in ALL patients
- Testing showed both immediate & delayed reactions
- 57% of patients had elevated serum immunoglobulin E (IgE) levels
- Deer keds appear to be an ideal vector for efficient transmission
- The risk for transmission to humans is apparent
- B. schoenbuchensis is most closely related to B bacilliformis, an important human pathogen also transmitted by a fly (Lutzomyia verrucarum)
- Five variants were found – some of which may pose a larger risk than others
- Clinical scenario of deer led dermatitis resembles a primary manifestation of Cat Scratch disease caused by B. henselae.
- A positive delayed-type hypersensitivity skin test, like that characteristically observed for B. henselae antigens in cat scratch disease (2), was also reported for all cases of deer ked dermatitis when whole deer ked extracts were used for the skin test (14). Also, C3 deposits in dermal vessels like those described for deer ked dermatitis (14) are consistent with infection by vasculotropic bartonellae (8). Taken together, certain clinical and histological characteristics of deer ked dermatitis are reminiscent of human infection by bartonellae, indicating that these pathogens should be considered possible etiological agents of deer ked dermatitis.
In summary, our study has provided evidence that deer keds collected from roe deer and red deer in Germany are commonly infected by B. schoenbuchensis. Furthermore, we have shown that B. schoenbuchensis colonizes the midgut of these arthropods and that this pathogen can be cultured at high titers from surface-sterilized arthropods. Our data suggest an important risk for the transmission of B. schoenbuchensis or related bartonellae to humans by the bite of an infected deer ked and suggest that a potential role of bartonellae in the etiology of deer ked dermatitis should be investigated further.
___________________
**Comment**
Some of you will remember this: http://danielcameronmd.com/swarming-deer-flies-quickly-expose-people-lyme-disease-anaplasmosis/ Entomologists corrected Dr. Cameron and he published, “RETRACTION: STILL NO EVIDENCE THAT DEER FLIES OR DEER KEDS TRANSMIT B. BURGDORFERI OR A. PHAGOCYTOPHILUM.”
Yet, this 2018 study shows the deer ked does carry Bb and Anaplasma: https://madisonarealymesupportgroup.com/2018/10/04/deer-fly-lyme-carrying-ectoparasite-on-the-move/ Although rarely reported in the United States, this vector (Lipoptena cervi, i.e. deer ked), recently has been shown to carry Borrelia burgdorferi and Anaplasma phagocytophylum from specimens collected domestically.
In 2016, Bb and Anaplasma was found via PCR in a Pennsylvanian deer led: https://www.ncbi.nlm.nih.gov/pubmed/27860010
In 2017, Bartonella spp. was found in Polish deer ked: https://www.ncbi.nlm.nih.gov/pubmed/29037227
Besides, Bb and Anaplasma, Bartonella has also been found in Norwegian Deer Flies: https://madisonarealymesupportgroup.com/2018/10/02/bartonella-found-in-deer-flies-deer-moose/ Bartonella, a huge player in Lyme/MSIDS, was found in 85% pools of adult wingless deer ked (n = 59). Two Bartonella lineages were identified based on phylogenetic analysis of the gltA gene and ITS region sequences.
Research is now desperately needed to connect these potential dots of how Lyme/MSIDS patients are acquiring Bartonella and other TBI’s. We need transmission studies done on many, many vectors. The one used by entomologists to downplay other vectors is 30 years old: https://www.ncbi.nlm.nih.gov/pubmed/?term=3170711
And even it shows Bb infection or antibodies in various horse flies & mosquitoes.
https://madisonarealymesupportgroup.com/2017/04/18/bartonella-vectors/
https://madisonarealymesupportgroup.com/2018/11/07/are-mosquitoes-transmitting-lyme-disease/
https://madisonarealymesupportgroup.com/2016/07/23/german-study-finds-borrelia-in-mosquitos/

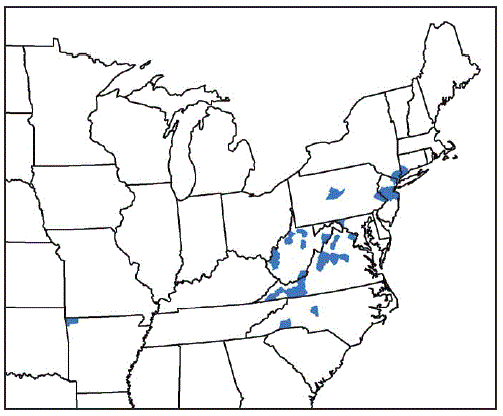 * Benton County, Arkansas; Fairfield County, Connecticut; Washington County, Maryland; Bergen, Hunterdon, Mercer, Middlesex, Monmouth, Somerset, and Union Counties, New Jersey; Davidson, Polk, and Rutherford Counties, North Carolina; Richmond, Rockland, and Westchester Counties, New York; Bucks and Centre Counties, Pennsylvania; Albemarle, Augusta, Carroll, Fairfax, Giles, Grayson, Louisa, Page, Pulaski, Rockbridge, Russell, Scott, Smyth, Staunton City, Warren, and Wythe Counties, Virginia; Cabell, Hardy, Lincoln, Mason, Marion, Monroe, Putnam, Ritchie, Taylor, Tyler, Upshur Counties, West Virginia.
* Benton County, Arkansas; Fairfield County, Connecticut; Washington County, Maryland; Bergen, Hunterdon, Mercer, Middlesex, Monmouth, Somerset, and Union Counties, New Jersey; Davidson, Polk, and Rutherford Counties, North Carolina; Richmond, Rockland, and Westchester Counties, New York; Bucks and Centre Counties, Pennsylvania; Albemarle, Augusta, Carroll, Fairfax, Giles, Grayson, Louisa, Page, Pulaski, Rockbridge, Russell, Scott, Smyth, Staunton City, Warren, and Wythe Counties, Virginia; Cabell, Hardy, Lincoln, Mason, Marion, Monroe, Putnam, Ritchie, Taylor, Tyler, Upshur Counties, West Virginia.