French Documentary on Lyme Disease
https://vimeo.com/95647143 Approx. 53 Min
LYME DISEASE A SILENT EPIDEMIC PRODUCED BY FRANCE 5 PUBLIC NETWORK AND GRAND ANGLE DIRECTED BY CHANTAL PERRIN

https://vimeo.com/95647143 Approx. 53 Min
Improved serodiagnostic performance for Lyme disease by use of two recombinant proteins in ELISA as compared to standardized two tier testing
Bradshaw GL, Thueson RK, Uriona TJ.
Journal of Clinical Microbiology, online first, 2017 Aug 2.
https://doi.org/10.1128/JCM.01004-17
Abstract
The most reliable test method for the serological confirmation of Lyme Disease (LD) is a 2-tiered method recommended by the CDC in 1995. The first-tier test is a low specificity ELISA test and the second-tier tests are higher specificity IgG and IgM Western blots. This study describes the selection of two Borrelia burgdorferi-recombinant proteins and evaluation of their performance in a simple 1-tier test for the serological confirmation of LD.
These two proteins were generated from
(a) the full length dbpA gene combined with the invariable region 6 of the VlsE gene (dbpA/C6) and
(b) the full length OspC gene.
The expressed dbpA/C6 and the OspC proteins were useful in detecting anti-Borrelia IgG and IgM antibodies, respectively. A blind study was conducted on a well-characterized panel of 279 human sera from the CDC comparing ELISA tests using these two recombinant antigens with the 2-tiered test method. The two methods (dbpA/C6-OspC vs 2-tiered) compared equivalently in identifying sera from negative control subjects (99% vs 100% specificity, respectively) and in detecting stage II & III LD patient sera (100% vs 100% sensitivity). However, the dbpA/C6-OspC ELISA test was markedly better (80% vs 63%) than the 2-tiered test method in detecting anti-Borrelia antibodies in stage I LD patients.
The finding suggest that these antigens could be used in a simple 1-tier ELISA assay that is faster to perform, easier to interpret, and less expensive than the 2-tiered test method, and which is better at detecting Borrelia specific antibodies in patient sera with stage I LD.
More on testing:
https://madisonarealymesupportgroup.com/2017/04/12/comparing-lyme-testing-with-hiv-testing/
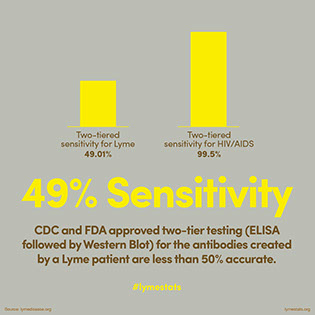


https://www.lymedisease.org/lyme-basics/lyme-disease/diagnosis/ Testing explained and interpreted.
Cases of transfusion-transmitted babesiosis occurring in nonendemic areas: a diagnostic dilemma
LeBel, D. P., Moritz, E. D., O’Brien, J. J., Lazarchick, J., Tormos, L. M., Duong, A., Fontaine, M. J., Squires, J. E. and Stramer, S. L.
Transfusion, online first August 7, 2017.
https://doi.org/10.1111/trf.14246
Abstract
BACKGROUND
Transfusion-transmitted babesiosis (TTB) has been rapidly increasing in incidence since the beginning of the 21st century. Asymptomatic individuals with Babesia infection are able to donate blood in the United States because of the lack of specific blood donation testing. Blood products collected in Babesia-endemic areas are distributed nationally; thus, clinicians in nonendemic states may fail to include babesiosis in the differential diagnosis of a patient who had a recent transfusion history and a fever of unknown origin.
STUDY DESIGN AND METHODS
We report the details of two cases of clinical transfusion-transmitted babesiosis and one asymptomatic infection identified in red blood cell recipients in two nonendemic states (South Carolina and Maryland), which, when combined with three recent additional cases in nonendemic states, totals six recipient infections in three nonendemic states.
RESULTS
Delayed diagnosis of transfusion-transmitted babesiosis places patients at risk for increased morbidity and mortality and may result in clinical mismanagement or unnecessary treatments. A peripheral blood smear should be reviewed in any patient with a recent transfusion and a fever of unknown origin. Prompt communication of the diagnosis among physicians is key to ensuring that patients with transfusion-transmitted babesiosis are treated expeditiously, and a transfusion service investigation is necessary to identify additional recipients from the same donor.
CONCLUSION
TTB is appearing in traditionally nonendemic states because of blood product distribution patterns. Clinicians should include TTB on the differential diagnosis in any patient presenting who had a recent transfusion history and a fever of unknown origin, regardless of where the transfusion took place.
More on Babesia: https://madisonarealymesupportgroup.com/2016/01/16/babesia-treatment/
https://madisonarealymesupportgroup.com/2016/11/19/seroprevalence-of-babesia-in-individuals-with-ld/

Musical about Lyme Disease being created by Wisconsin resident, Audra Cashman
Our next Lyme support meeting will be Friday, August 25, 2017 at 5:30-8:45pm at Pinney Library in Madison.
I would love to see and hear from all of you, plus, my daughter will be in attendance as she is writing a musical about Lyme Disease as well as composing the music, and needs your ideas. Please come and share as who knows – your story may make the stage!
See you soon!