Disseminated Cat Scratch Disease in Pediatric Patients in Hawaii
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7260883/
Disseminated Cat Scratch Disease in Pediatric Patients in Hawaii
Abstract
Cat scratch disease is known to be a generally benign, self-resolving illness associated with non-specific symptoms, including lymphadenopathy, fever, fatigue, anorexia, and headaches. However, it can also cause disseminated disease with a wide range of manifestations, including liver and spleen microabscesses, osteomyelitis, encephalitis, and uveitis.
Eighteen pediatric cases of disseminated cat scratch disease at a single center in Hawaii are described. This case series emphasizes the importance of disease recognition and use of appropriate diagnostic tools and disease management. The disease burden of pediatric patients with disseminated cat scratch disease in the state of Hawaii has a high incidence and should be considered in pediatric patients with prolonged febrile illnesses.
____________________
**Comment**
This is important because few doctors will consider Bartonella in pediatric patients. Like the article states, most doctors consider Bartonella to be a benign, self-resolving disease when nothing could be further from the truth. In fact, I’d go as far to say it can be as bad as Lyme if not worse. It’s very tenacious.
For more: https://madisonarealymesupportgroup.com/category/bartonella-treatment/
https://madisonarealymesupportgroup.com/2019/02/06/uh-study-shows-hawaii-kids-more-vulnerable-to-bartonella/ University of Hawaii study shows Hawaii keiki are more than three times more likely to get severe forms of cat scratch disease than mainland kids.
This is an interesting finding. I wouldn’t blame only cats. Bartonella can be transmitted from many, many things:
Mode of Transmission: Arthropod vectors including fleas and flea feces, biting flies such as sand flies and horn flies, the human body louse, mosquitoes, and ticks; through bites and scratches of reservoir hosts; and potentially from needles and syringes in the drug addicted. Needle stick transmission to veterinarians has been reported. There is documentation that cats have received it through blood transfusion. 3.2% of blood donors in Brazil were found to carry Bartonella in their blood. Bartonella DNA has been found in dust mites. Those with arthropod exposure have an increased risk, as well as those working and living with pets that have arthropod exposure. 28% of veterinarians tested positively for Bartonella compared with 0% of controls. About half of all cats may be infected with Bartonella – as high as 80% in feral cats and near 40% of domestic cats. In various studies dogs have close to a 50% rate as well. Evidence now suggests it may be transmitted congenitally from mother to child – potentially leading to birth defects.
**On a personal note**
If my husband and I have symptoms – they are typically Bartonella symptoms. After years of treatment, we both use Berberine, which has served as a wonderful maintenance treatment for both of us: https://madisonarealymesupportgroup.com/2019/05/05/good-news-for-bartonella-patients-identification-of-fda-approved-drugs-with-higher-activity-than-current-front-line-drugs/

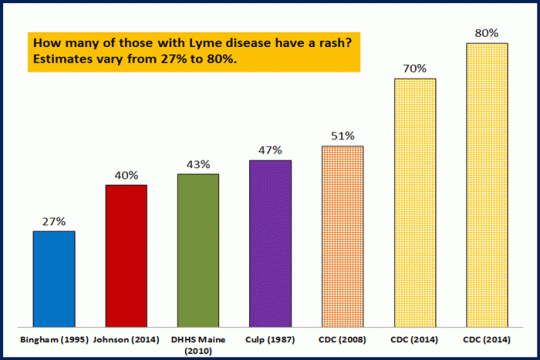 Various studies showing how many get the EM rash.
Various studies showing how many get the EM rash.