By Jennifer Crystal
People who haven’t had late-stage Lyme disease sometimes ask what the worst symptom I experienced was.
Without hesitation, it was insomnia. The Lyme bacteria had burrowed so deeply into my nervous system that my brain was on overdrive; despite bone-crushing fatigue, I could not shut my brain off to sleep. At one point, I was awake for three weeks straight. Worse, when I did sleep, I had hallucinogenic nightmares that were more exhausting than my waking hours.
Most of my dreams were non-sensical, and I had so many of them in a night, in such vivid detail, that it was hard to recall them all. But certain ones stick with me to this day. There are the good ones, the ones with meaning, like the recurring dream I described in “Missing the Summer of Life”.
And then there are the awful ones. I’m not talking about the worst of the nightmares, in which I was shot, burned, or raped. Those were traumatic in their own right. But more awful to me were the realistic dreams, those that played out the fatigue I felt in real life, in the context of things I could no longer do. Sometimes I would dream about lying in the middle of my former college campus, too tired to talk to friends walking by. Sometimes I’d be at the bottom of a ski hill, too tired to open my eyes or sit up, as healthy skiers whooshed past. I felt fatigue in my sleep as deeply as I felt it when I was awake. Not only were nights not restorative, but I woke feeling sad and anxious, longing for my old abilities and wondering if life would just pass me.
But as treatment for Lyme disease and the co-infections babesiosis and ehrlichiosis began to work, inflammation in my brain decreased. My waking energy improved, and my dreams shifted. Many nights I still had the awful nightmares, but peppered among them were better dreams about feelings I’d once experienced, but had long forgotten in my years of convalescence. Instead of lying at the bottom of a ski hill, I zoomed down it, without air hunger or a headache. My legs, which had felt so achy and weighted for so long, were light and strong in these dreams. I skied for hours, never tiring. The rush I used to feel from skiing in real life came back to me in these dreams, and I woke smiling.
Other nights my dreams reminded me of the euphoria of being in love, or of the giddiness of being tipsy. I didn’t only feel healthy in these dreams; I also got to experience the emotions that come with joy and fun. I wasn’t yet able to ski, or date, or go to a party in real life, but my dreams made those activities feel within reach. Instead of longing for what I’d lost, I started feeling hopeful about what I might someday be able to do.
I was once again dreaming of living, and those dreams worked as a nice metaphor for the possibilities that opened up to me as I got healthier and healthier. Eventually, I was able to ski, albeit slowly. I started socializing more. I laughed.
My journey to wellness wasn’t linear, and neither was the trajectory of my dreams. When I had physical setbacks, my dreams often mirrored them. Or, sometimes they’d forewarn them. For example, I might dream about driving a car too fast and not being able to hit the brakes. These dreams told me that I was pushing my body a little too hard; if I didn’t slow down, I might crash. As I wrote in this post, sometimes rest was the most important message of my dreams.
Dreaming of the past can be difficult, but it’s a way for us to mourn what we’ve lost. Dreaming of the future gives us hope, and lets us grasp feelings we can’t yet access in real life. Joy, fun, happiness, silliness—they’re hard to come by when you’re sick, but with proper treatment, rest, and time, they can shift from dream to reality.

Opinions expressed by contributors are their own.
Jennifer Crystal is a writer and educator in Boston. Her memoir about her medical journey is on submission. Contact her at lymewarriorjennifercrystal@gmail.com.



 This Global Lyme Alliance (GLA) PSA kicks off our 2021 radio campaign which is aimed at raising awareness for GLA and our mission to serve the Lyme Community! In addition to the Super Bowl spot, GLA will also debut several radio public service announcements (PSA’s) during the Yankees/Mets broadcasts throughout the season.
This Global Lyme Alliance (GLA) PSA kicks off our 2021 radio campaign which is aimed at raising awareness for GLA and our mission to serve the Lyme Community! In addition to the Super Bowl spot, GLA will also debut several radio public service announcements (PSA’s) during the Yankees/Mets broadcasts throughout the season.

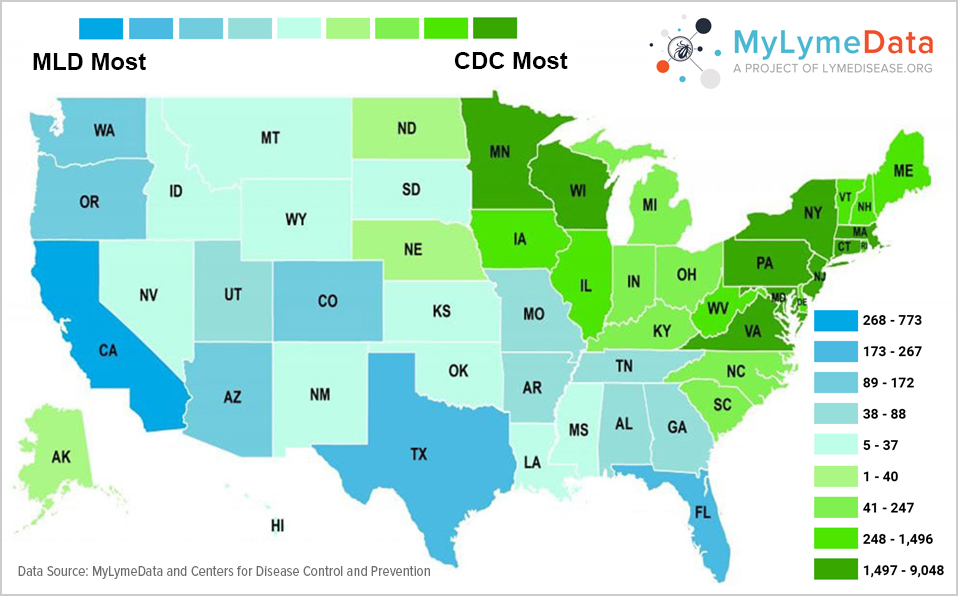
MyLymeData is one of the largest patient-driven registries in the nation, with over 13,500 patients enrolled. It was created by patients, is run by patients and will address the issues that Lyme disease patients care about. MyLymeData Viz provides the community with results from MyLymeData. If you are enrolled in MyLymeData, we thank you for providing the data that will accelerate the pace of research in Lyme disease. If you are not enrolled, please enroll today.