https://www.bca-clinic.de/en/way-know-lyme-disease-gone/
Is There A Definitive Way To Know That Your Lyme Disease Is Gone?

Lyme disease confounds doctors all over the world. There are many reasons for this, all of which compound each other. The end result is a particularly insidious disease that is currently sweeping the globe in a pandemic-like way. Yet doctors simply don’t know enough about the disease to combat it effectively. Chronic Lyme isn’t even regarded as a legitimate condition, a fact that continually muddies the waters of conversation around the disorder. Because of this, patients often feel like there is no light at the end of the tunnel, as their doctors are unable to offer them satisfactory answers. So is there a cure for Lyme disease somewhere in the pipeline? And if there is, how can patients be totally sure that their symptoms are gone, and that they won’t relapse?
What is Lyme Disease?
Lyme disease is a relatively new disorder; it was first named in 1975 in Connecticut, and even today, many people still associate Lyme solely with the north-east of America. It is a condition spread by certain species of ticks and caused by a strain of bacteria called Borrelia burgdorferi. Not all ticks carry the Borrelia strain, but a significant number do. When these ticks find a human host, there is a chance that the bacteria can be transmitted during the feeding process.
There are two forms of Lyme disease: acute and chronic. Acute Lyme produces flu-like symptoms and, more pertinently, a bullseye rash at the site of the bite. When this recedes after a few weeks, chronic Lyme starts to set in. This involves a complicated mix of infection and inflammation symptoms, with the most predominant caused by the body attacking itself.

How Accurate Are Lyme Disease Tests?
Curing chronic Lyme is problematic, but diagnosing it in the first instance can be the bigger challenge. Lyme disease is sometimes known as ‘The Great Imitator’ because its symptoms are often generalised and mimic the manifestations of other long-term, chronic conditions. Therefore, Lyme disease will often be found very low on a doctor’s priority list, if it’s there at all. To compound matters, the blood test traditionally used to diagnose Lyme (known as an ELISpot test) can often return false negatives, especially for the chronic form. The blood test only detects antigens related to active infection. As chronic Lyme is a mix of active infection and self-induced inflammation – the ratio of which differs for every patient – false negatives are, unfortunately, all too common.
Lyme specialists like BCA-clinic have taken measures to combat this ineffective testing by helping to develop their own, much more accurate blood test, called the LymeSpot. This takes into account ‘memory’ antigens (signifiers of an established infection), as well as ‘attacking’ antigens. The end result is a much clearer and more specific snapshot of the state of the disease.
How Do I Know If Lyme Disease Is Gone?
The key to eradicating an infection in the body is the immune system. There is no other way to achieve it. The predominant issue with Lyme is that it compromises the immune system by overwhelming it with bacteria. The immune response then misfires, resulting in a whole new set of symptoms that will become locked in a negative feedback loop over time. This is why we see some patients who have very little traces of infection left in the system, but are still suffering from a high degree of inflammation symptoms. Although this is still classified as Lyme, antibiotics will not work in this case.
Lyme specialists are acutely aware of this dichotomy, and places like BCA-clinic treat both strands of the disease simultaneously. The bacterial population is eradicated with antibiotics, while the inflammation symptoms are addressed by supporting the body’s natural defences through nutritional regimes.
It might sound simple to say, but with a disease as complex as Lyme, the only indicator of recovery is good health – that is, the eradication of symptoms. BCA-clinic considers this the definitive measure of how successful a patient’s treatment was. It is impossible to test every cell or tissue for traces of bacteria. There is no test in the world that can achieve this. Instead, BCA-clinic tests the response (or absence of a response) the body has against a particular pathogen, and the clinical status of the patient.

Is It Possible to Live Symptom-Free?
Some good news: yes, it is absolutely possible to live free from the symptoms of Lyme. BCA-clinic has treated many patients who have lived happily and healthily after recovering from the disease. You might ask the question ‘Can Lyme disease come back?’, but recent studies suggest that resurgences of the disease are down to new infections, not relapses. Many patients are encouraged to maintain healthy lifestyles after their bout with Lyme in order to preserve their immune system in the face of new viruses or infections, and to maintain good general health.
If a patient does not recover after prolonged treatment, BCA-clinic believes there is another reason – possibly co-infections that have not been addressed, genetic mutations that inhibit the effectiveness of the treatment, or inappropriate treatment from previous doctors. When a patient comes to BCA-clinic after years of outside treatment, the team begins by looking at factors like these before devising their own plan.
Featured image by freddie marriageonUnsplash
________________
**Comment**
I completely and wholeheartedly disagree that resurgence of disease is only due to new infections and not due to relapses. My husband and I, as well as many patients have suffered relapses and antibiotics completely cleared these relapses up giving us our health back.
There is something called “molecular memory,” and you never, ever forget what it feels like when you are infected. The old symptoms come roaring back with a vengeance making life unbearable. It’s at this point when you wave the white flag and go back on treatment.
In fact, in this article, I outline Dr. Burrascano’s success with “cycling” therapy where you purposely go off all antibiotics when you’ve been symptom-free for a number of months and then hit hard with antibiotics when symptoms return. He found this cycling approach to work for himself and many of his patients after 3-4 cycles they remained symptom-free: https://madisonarealymesupportgroup.com/2019/02/22/why-mainstream-lyme-msids-research-remains-in-the-dark-ages/
The “recent” studies mentioned in this article consist of ONE study done in 2012. I don’t consider a study conducted eight years ago “recent.”
The other glaring issue with this 2012 study is it focused on the EM rash, when research has shown those getting the rash vary considerably with many never getting it:
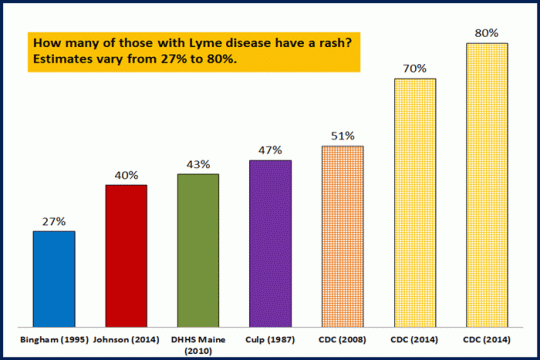
Only a quarter of patients from the first ever patient group back in the 70’s got the rash: 1976circularletterpdf
What many don’t realize is the EM rash is mandatory entrance criteria to get into research studies, despite many patients never having the rash. This myopic and highly stringent criteria has been hurting patients for over 40 years as the research does not reflect a majority of patients yet is used with abandon.
Entrance into research studies have also required a positive on 2-tiered serology, which research has proven serology testing to be abysmal in detecting Lyme: https://madisonarealymesupportgroup.com/2018/10/12/direct-diagnostic-tests-for-lyme-the-closest-thing-to-an-apology-you-are-ever-going-to-get/
Excerpt:
“These serologic tests cannot distinguish active infection, past infection, or reinfection.”
In plain English, these tests don’t show squat yet are required research study entrance criteria.
Even this ancient 1995 shows a patient with repeated neurologic relapses despite aggressive antibiotic therapy, with obvious Jarisch-Herxheimer reactions with each course of therapy who NEVER had detectable free antibodies to Lyme in serum or spinal fluid: Seronegative Chronic Relapsing Neuroborreliosis https://www.ncbi.nlm.nih.gov/pubmed/7796837
And advocate Carl Tuttle is absolutely correct in stating that this disease has been pigeon-holed into a narrowly defined parameter so that research yields a pre-determined outcome: https://madisonarealymesupportgroup.com/2019/11/22/wormsers-junk-science-deliberate-avoidance-of-chronically-ill-patients-a-letter-him-asking-why/
Excerpt:
WORMSER ET AL DO NOT DISCUSS THE CONSEQUENCES OF UNTREATED LYME DISEASE IN THEIR PLOS PUBLISHED PAPER. WHY DO YOU THINK THAT IS THE CASE DR. HEBER?
Post Treatment Lyme Disease Syndrome after early treatment and untreated late stage Lyme of months, years or decades are two distinctly different disease states with the later going unrecognized for over three decades. The absence of a bulls-eye rash after tick bite allows patients to progress to severe neurological disease instead of obtaining a prompt diagnosis and early treatment. Purposely avoiding the advanced stage of disease hides the horribly disabled and anyone unable to see this is somewhat naïve. Avoiding the seriously disabled Lyme patient population hides the severity of the disease as exposed in the “Under our Skin” documentary.
And please remember the 700+ peer-reviewed papers showing pathogen persistence: Peer-Reviewed Evidence of Persistence of Lyme:MSIDS copy, as well as this 2019 evidence based chronic Lyme disease definition: https://madisonarealymesupportgroup.com/2019/12/17/chronic-lyme-disease-an-evidence-based-definition-by-the-ilads-working-group/
Excerpt:
Conclusion: This evidence-based definition of chronic Lyme disease clarifies the term’s meaning and the literature review validates that chronic and ongoing Bbsl infections can result in chronic disease.
