FREE Webinar: The State of Lyme Disease Research & Tick-Borne Disease-Related Legislative Action
https://us02web.zoom.us/webinar/register/WN_S4YmYqBvTECf6M5FyHkzMg#/registration Register Here

https://us02web.zoom.us/webinar/register/WN_S4YmYqBvTECf6M5FyHkzMg#/registration Register Here
(LifeSiteNews) — According to a well-known leader in COVID-19 early medical treatments, “conclusive evidence” has been established that “clinically significant shedding” of the mRNA vaccines from the injected to the non-injected is indeed a reality.
Dr. Pierre Kory, who helped pioneer and tenaciously defend the use of “miraculous” ivermectin to treat COVID-19, has published an eight-part series on the question of “shedding,” a medical phenomenon which is defined by the Food and Drug Administration as:
The release of viral or bacterial gene therapy products from the patient by any or all of the following routes: feces (feces); secretions (urine, saliva, nasopharyngeal fluids, etc.); or through the skin (pustules, lesions, sores).
The Wisconsin-based physician, with a specialty in critical care, added the FDA “forgot to mention ‘exhaled breath’” to this list of possible means for transfer of the vaccine substance.
His latest article in the series relates 32 examples of unedited correspondence he has received from some of his 70,000 Substack readers describing “prior episodes of sudden-onset vaccine side effect symptoms after an exposure to vaccinated people.” (See link for article and eight part series)
______________
For more:
https://danielcameronmd.com/full-body-numbness-and-tingling-due-to-lyme-disease/
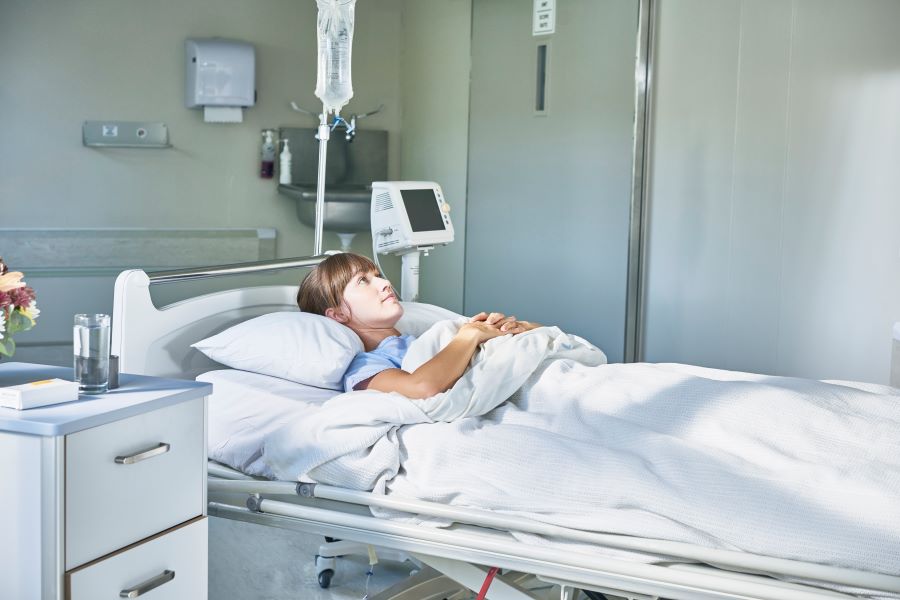
In their article “Lyme Disease Presenting With Interesting Neurological Features of Weakness and Hyporeflexia: A Case Report,” Semy and colleagues describe the unique case of a young woman with Lyme disease who exhibited solely neurologic features of numbness and tingling throughout her body. [1]
The 25-year-old female developed numbness and tingling throughout her torso, which later spread to her entire body. She presented to a neurology clinic with complaints of numbness and tingling that had been ongoing for the past 4 weeks.
She did not recall a rash or tick bite and had not recently travelled.
The woman did not exhibit any of the typical symptoms seen with Lyme disease such as “arthralgia, fever, rash, or regional lymphadenopathy but in fact exhibited decreased reflexes, numbness, and tingling particularly near the hypogastric region making it distinct from the classical presentation,” the authors wrote.
The numbness and tingling began on the right side of her stomach and radiated to her back and later spread to her entire body. “The tingling was not associated with any burning or pins and needle sensation,” the authors point out.
The woman was prescribed steroids and an albuterol inhaler. But her symptoms did not improve.
Motor examination revealed that the patient had “decreased tone more significant in the upper limbs (3/5) than in the lower limbs (4/5) along with hyporeflexia in the biceps, triceps, patellar, and Achilles,” the authors wrote.
A lumbar puncture revealed elevated protein concentration (148 mg/dl; normal: 15-60 mg/dl).
The Western blot test for Lyme disease was positive, and the woman was prescribed IV ceftriaxone for 3 days before transitioning to oral doxycycline.
“At the time of discharge, the patient was able to move all extremities spontaneously and ambulate with a normal gait,” the authors wrote. At her follow-up visit, she exhibited only minimal residuary weakness.
Authors’ Conclude:
Atypical symptoms of Lyme disease: numbness, paresthesias and abdominal wall weakness
_______________
**Comment**
This woman needs long-term follow-up. I wouldn’t be shocked at all if these symptoms came roaring back, which of course would necessitate treatment that our corrupt government states is “dangerous,” even though the alternative is deadly.
For more:
https://greenmedinfo.com/blog/powerful-aspirin-alternative-grows-trees-2
When it comes to aspirin alternatives, one promising contender is pycnogenol, a powerful antioxidant extracted from French maritime pine bark, backed by over 40 years of research, the most compelling of which we have aggregated on GreenMedInfo.com here: Pycnogenol Research. Amazingly, you will find research indexed there showing it may have value for over 80 health conditions
Pycnogenol, like so many other natural interventions, has a wide range of side benefits that may confer significant advantage when it comes to reducing cardiovascular disease risk. For instance, pycnogenol is also:
For more:
For more:
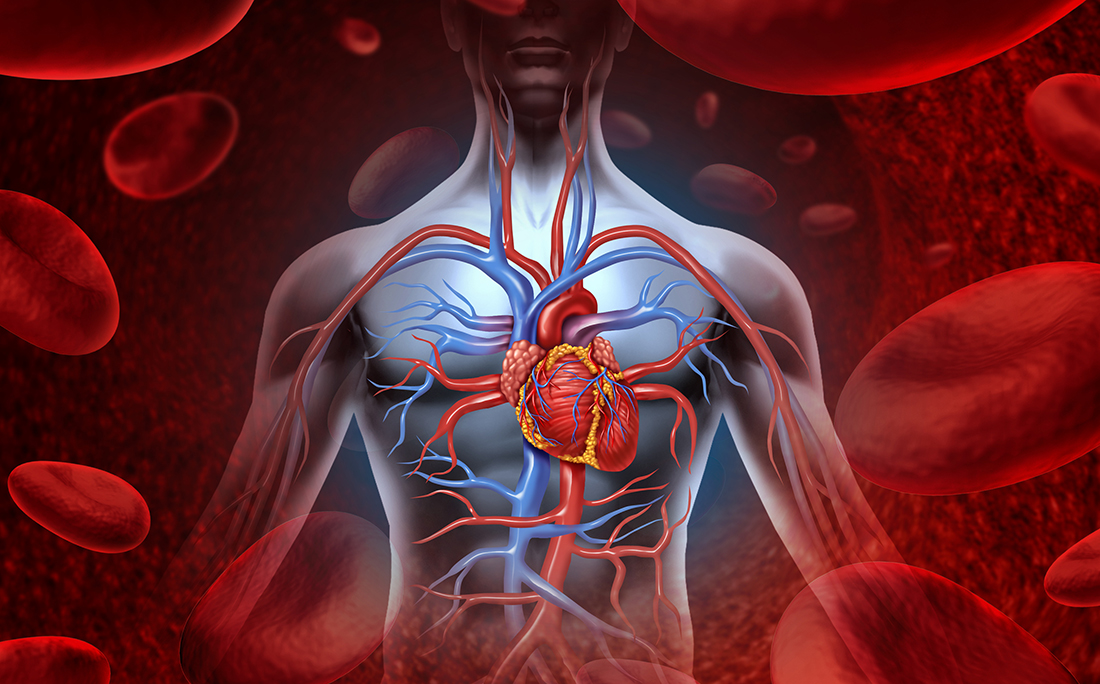
“Although rare, sudden cardiac death caused by Lyme disease might be an under-recognized entity,” according to researchers who describe their findings from an autopsy study on 5 case patients who died from sudden cardiac death and were found post mortem to have Lyme carditis. The cases are discussed in an article entitled Cardiac Tropism of Borrelia burgdorferi: An Autopsy Study of Sudden Cardiac Death Associated with Lyme Carditis, published in The American Journal of Pathology.
Fatal Lyme carditis is rarely identified. In reviewing five post mortem cases, Muehlenbach and colleagues found that Lyme disease was not suspected for one patient who complained of episodic shortness of breath, while the second patient tested negative for Lyme disease. Two other patients did not seek medical care. Details regarding the fifth patient were not released.
 Ultimately, two case patients were diagnosed during unexplained-death investigations at the Centers for Disease Control and Prevention (CDC). Lyme disease was suspected in two of the other cases by cardiac pathology at a tissue bank transplant service. Muehlenbachs and colleagues reassure the readers that cardiac tissue was not transplanted. [1]
Ultimately, two case patients were diagnosed during unexplained-death investigations at the Centers for Disease Control and Prevention (CDC). Lyme disease was suspected in two of the other cases by cardiac pathology at a tissue bank transplant service. Muehlenbachs and colleagues reassure the readers that cardiac tissue was not transplanted. [1]
Spirochetes were present in the heart on all 5 cases. When using immunohistochemistry (IHC), spirochetes were found “within the myocardial interstitial infiltrates, in the subendocardium, and occasionally in pericardial tissue in association with lymphohistiocytic infiltrates.” Muehlenbachs adds, “Rare spirochetes were seen in the leptomeninges of two cases by immunohistochemistry.”
All 5 cases lived in Lyme-endemic areas. Patients resided in counties with a high or moderate incidence of Lyme disease including, New York, New Hampshire (with recent travel to Connecticut), Massachusetts and Indiana.
All 5 cases reportedly engaged in outdoor activities. “Two patients had known exposure to ticks, and one patient reported a recent bite.”
None of the 5 cases met the CDC surveillance case definition for Lyme carditis. This definition includes: recurrent, brief attacks (weeks or months) of objective joint swelling in one or several joints; lymphocytic meningitis; cranial neuritis; radiculoneuropathy; encephalomyelitis; acute onset of high-grade (2nd-degree or 3rd-degree) atrioventricular conduction defects, and myocarditis.
Only 1 of the 5 cases underwent serologic screening for Lyme disease and the results were negative.
All 5 cases were symptomatic prior to their death. “A prodrome was reported for each of the patients that included the following: non-specific viral-like illness, malaise, shortness of breath, and anxiety,” according to Muehlenbachs. “One of these patients also had joint and muscle pain, and the other two patients had joint pain for an unknown duration.”
“No dermatologic lesion was documented or reported for any of the patients, although one patient was evaluated in an emergency department 1 month before death for an arm lesion diagnosed as a possible spider bite from which methicillin-resistant Staphylococcus aureus was isolated in culture.”
All 5 cases were seropositive post mortem according to the CDC’s two-tier criteria. “One sample met both IgM and IgG Western Blot (WB) criteria, with two of the three IgM bands and 6 of the 10 IgG bands reactive. The four remaining samples were positive by IgM WB criteria only, although three were nearly IgG positive with 4 of the 10 bands reactive,” states Muehlenbachs.
Underlying cardiac disease may have played a role in 3 of the 5 cases of sudden cardiac deaths associated with Lyme disease, Muehlenbachs points out, since there was significant underlying heart disease present in two patients, and an additional patient had moderate atherosclerosis, discovered at autopsy.
Physiological cardiac stress was considered a potential factor in 2 of the 5 cases. “In the other two patients, who were otherwise healthy, a degree of physiological cardiac stress likely was present: the woman had given birth 6 months previously and the man was a physically active outdoor enthusiast,” according to Muehlenbachs.
These pathologic findings provide insight into the possible cause behind sudden cardiac deaths associated with Lyme disease. “The findings support the proposed disease mechanism of spirochete cardiac tropism during early disease dissemination, the infiltration of cardiac tissue by inflammatory cells, and involvement of the conduction system, which likely mediates sudden cardiac death.” [1]
“Early diagnosis and prompt treatment for Lyme carditis can be life-saving,” according to Muehlenbachs. “Health care professionals should evaluate all patients with suspected Lyme disease for cardiac signs and symptoms, and obtain an electrocardiogram promptly if carditis is suspected.” Furthermore, “diagnosis is based on clinical suspicion and serologic testing, with the caveat that serology testing may be falsely negative in a patient with recent illness onset.” [1]
Fishe and colleagues describe how early diagnosis and treatment helped save the life of a 15-year-old African-American girl with Lyme carditis. [2] The patient was hospitalized after a 3-day history of intermittent retrosternal and epigastric pain. After treatment was initiated, she developed a heart block. Tests for Lyme disease were positive and she was diagnosed with Lyme disease-associated myocarditis.
The adolescent was empirically started on doxycycline and was concurrently treated with milrinone infusion for afterload reduction and intravenous furosemide for pulmonary edema. Her EKG changed to first-degree heart block by day 2 and resolved completely on hospital day 3.
She recovered and was discharged home on hospital day 7 on oral furosemide, enalapril, and doxycycline, according to Fishe and colleagues.
However, another adolescent was not so fortunate. He died suddenly from undiagnosed Lyme carditis, following complaints of flu-like symptoms. The case is discussed in another All Things Lyme blog, Relying on a Negative Lyme Disease Test Can Prove Deadly.
“In patients with Lyme disease who complain of cardiopulmonary symptoms, clinicians should have a low threshold for obtaining an EKG to evaluate for Lyme carditis,” Fishe points out. Furthermore, clinicians should take note that in “children and adolescents, respiratory and gastrointestinal complaints, with or without chest pain, are the most frequent presenting symptoms.”
References: