https://imprimis.hillsdale.edu/marijuana-mental-illness-violence/?
The following is adapted from a speech delivered on January 15, 2019, at Hillsdale College’s Allan P. Kirby, Jr. Center for Constitutional Studies and Citizenship in Washington, D.C.
By Alex Berenson
Author, Tell Your Children: The Truth About Marijuana, Mental Illness, and Violence
Seventy miles northwest of New York City is a hospital that looks like a prison, its drab brick buildings wrapped in layers of fencing and barbed wire. This grim facility is called the Mid-Hudson Forensic Psychiatric Institute. It’s one of three places the state of New York sends the criminally mentally ill—defendants judged not guilty by reason of insanity.
Until recently, my wife Jackie —Dr. Jacqueline Berenson—was a senior psychiatrist there. Many of Mid-Hudson’s 300 patients are killers and arsonists. At least one is a cannibal. Most have been diagnosed with psychotic disorders like schizophrenia that provoked them to violence against family members or strangers.
A couple of years ago, Jackie was telling me about a patient. In passing, she said something like, Of course he’d been smoking pot his whole life.
Of course? I said.
Yes, they all smoke.
So marijuana causes schizophrenia?
I was surprised, to say the least. I tended to be a libertarian on drugs. Years before, I’d covered the pharmaceutical industry for The New York Times. I was aware of the claims about marijuana as medicine, and I’d watched the slow spread of legalized cannabis without much interest.
Jackie would have been within her rights to say, I know what I’m talking about, unlike you. Instead she offered something neutral like, I think that’s what the big studies say. You should read them.
So I did. The big studies, the little ones, and all the rest. I read everything I could find. I talked to every psychiatrist and brain scientist who would talk to me. And I soon realized that in all my years as a journalist I had never seen a story where the gap between insider and outsider knowledge was so great, or the stakes so high.
I began to wonder why—with the stocks of cannabis companies soaring and politicians promoting legalization as a low-risk way to raise tax revenue and reduce crime—I had never heard the truth about marijuana, mental illness, and violence.
***
Over the last 30 years, psychiatrists and epidemiologists have turned speculation about marijuana’s dangers into science. Yet over the same period, a shrewd and expensive lobbying campaign has pushed public attitudes about marijuana the other way. And the effects are now becoming apparent.
Almost everything you think you know about the health effects of cannabis, almost everything advocates and the media have told you for a generation, is wrong.
They’ve told you marijuana has many different medical uses. In reality marijuana and THC, its active ingredient, have been shown to work only in a few narrow conditions. They are most commonly prescribed for pain relief. But they are rarely tested against other pain relief drugs like ibuprofen—and in July, a large four-year study of patients with chronic pain in Australia showed cannabis use was associated with greater pain over time.
They’ve told you cannabis can stem opioid use—“Two new studies show how marijuana can help fight the opioid epidemic,” according to Wonkblog, a Washington Post website, in April 2018— and that marijuana’s effects as a painkiller make it a potential substitute for opiates. In reality, like alcohol, marijuana is too weak as a painkiller to work for most people who truly need opiates, such as terminal cancer patients. Even cannabis advocates, like Rob Kampia, the co-founder of the Marijuana Policy Project, acknowledge that they have always viewed medical marijuana laws primarily as a way to protect recreational users.
As for the marijuana-reduces-opiate-use theory, it is based largely on a single paper comparing overdose deaths by state before 2010 to the spread of medical marijuana laws— and the paper’s finding is probably a result of simple geographic coincidence. The opiate epidemic began in Appalachia, while the first states to legalize medical marijuana were in the West. Since 2010, as both the epidemic and medical marijuana laws have spread nationally, the finding has vanished. And the United States, the Western country with the most cannabis use, also has by far the worst problem with opioids.
Research on individual users—a better way to trace cause and effect than looking at aggregate state-level data—consistently shows that marijuana use leads to other drug use. For example, a January 2018 paper in the American Journal of Psychiatry showed that people who used cannabis in 2001 were almost three times as likely to use opiates three years later, even after adjusting for other potential risks.
Most of all, advocates have told you that marijuana is not just safe for people with psychiatric problems like depression, but that it is a potential treatment for those patients. On its website, the cannabis delivery service Eaze offers the “Best Marijuana Strains and Products for Treating Anxiety.” “How Does Cannabis Help Depression?” is the topic of an article on Leafly, the largest cannabis website. But a mountain of peer-reviewed research in top medical journals shows that marijuana can cause or worsen severe mental illness, especially psychosis, the medical term for a break from reality. Teenagers who smoke marijuana regularly are about three times as likely to develop schizophrenia, the most devastating psychotic disorder.
After an exhaustive review, the National Academy of Medicine found in 2017 that “cannabis use is likely to increase the risk of developing schizophrenia and other psychoses; the higher the use, the greater the risk.” Also that “regular cannabis use is likely to increase the risk for developing social anxiety disorder.”
***
Over the past decade, as legalization has spread, patterns of marijuana use—and the drug itself—have changed in dangerous ways.
Legalization has not led to a huge increase in people using the drug casually. About 15 percent of Americans used cannabis at least once in 2017, up from ten percent in 2006, according to a large federal study called the National Survey on Drug Use and Health. (By contrast, about 65 percent of Americans had a drink in the last year.) But the number of Americans who use cannabis heavily is soaring. In 2006, about three million Americans reported using cannabis at least 300 times a year, the standard for daily use. By 2017, that number had nearly tripled, to eight million, approaching the twelve million Americans who drank alcohol every day. Put another way, one in 15 drinkers consumed alcohol daily; about one in five marijuana users used cannabis that often.
Cannabis users today are also consuming a drug that is far more potent than ever before, as measured by the amount of THC—delta-9-tetrahydrocannabinol, the chemical in cannabis responsible for its psychoactive effects—it contains. In the 1970s, the last time this many Americans used cannabis, most marijuana contained less than two percent THC. Today, marijuana routinely contains 20 to 25 percent THC, thanks to sophisticated farming and cloning techniques—as well as to a demand by users for cannabis that produces a stronger high more quickly. In states where cannabis is legal, many users prefer extracts that are nearly pure THC. Think of the difference between near-beer and a martini, or even grain alcohol, to understand the difference.
These new patterns of use have caused problems with the drug to soar. In 2014, people who had diagnosable cannabis use disorder, the medical term for marijuana abuse or addiction, made up about 1.5 percent of Americans. But they accounted for eleven percent of all the psychosis cases in emergency rooms—90,000 cases, 250 a day, triple the number in 2006. In states like Colorado, emergency room physicians have become experts on dealing with cannabis-induced psychosis.
Cannabis advocates often argue that the drug can’t be as neurotoxic as studies suggest, because otherwise Western countries would have seen population-wide increases in psychosis alongside rising use. In reality, accurately tracking psychosis cases is impossible in the United States. The government carefully tracks diseases like cancer with central registries, but no such registry exists for schizophrenia or other severe mental illnesses.
On the other hand, research from Finland and Denmark, two countries that track mental illness more comprehensively, shows a significant increase in psychosis since 2000, following an increase in cannabis use. And in September of last year, a large federal survey found a rise in serious mental illness in the United States as well, especially among young adults, the heaviest users of cannabis.
According to this latter study, 7.5 percent of adults age 18-25 met the criteria for serious mental illness in 2017, double the rate in 2008. What’s especially striking is that adolescents age 12-17 don’t show these increases in cannabis use and severe mental illness.
A caveat: this federal survey doesn’t count individual cases, and it lumps psychosis with other severe mental illness. So it isn’t as accurate as the Finnish or Danish studies. Nor do any of these studies prove that rising cannabis use has caused population-wide increases in psychosis or other mental illness. The most that can be said is that they offer intriguing evidence of a link.
Advocates for people with mental illness do not like discussing the link between schizophrenia and crime. They fear it will stigmatize people with the disease. “Most people with mental illness are not violent,” the National Alliance on Mental Illness (NAMI) explains on its website. But wishing away the link can’t make it disappear. In truth, psychosis is a shockingly high risk factor for violence. The best analysis came in a 2009 paper in PLOS Medicine by Dr. Seena Fazel, an Oxford University psychiatrist and epidemiologist. Drawing on earlier studies, the paper found that people with schizophrenia are five times as likely to commit violent crimes as healthy people, and almost 20 times as likely to commit homicide.
NAMI’s statement that most people with mental illness are not violent is of course accurate, given that “most” simply means “more than half”; but it is deeply misleading. Schizophrenia is rare. But people with the disorder commit an appreciable fraction of all murders, in the range of six to nine percent.
“The best way to deal with the stigma is to reduce the violence,” says Dr. Sheilagh Hodgins, a professor at the University of Montreal who has studied mental illness and violence for more than 30 years.
The marijuana-psychosis-violence connection is even stronger than those figures suggest. People with schizophrenia are only moderately more likely to become violent than healthy people when they are taking antipsychotic medicine and avoiding recreational drugs. But when they use drugs, their risk of violence skyrockets. “You don’t just have an increased risk of one thing—these things occur in clusters,” Dr. Fazel told me.
Along with alcohol, the drug that psychotic patients use more than any other is cannabis: a 2010 review of earlier studies in Schizophrenia Bulletin found that 27 percent of people with schizophrenia had been diagnosed with cannabis use disorder in their lives. And unfortunately—despite its reputation for making users relaxed and calm—cannabis appears to provoke many of them to violence.
A Swiss study of 265 psychotic patients published in Frontiers of Forensic Psychiatry last June found that over a three-year period, young men with psychosis who used cannabis had a 50 percent chance of becoming violent. That risk was four times higher than for those with psychosis who didn’t use, even after adjusting for factors such as alcohol use. Other researchers have produced similar findings. A 2013 paper in an Italian psychiatric journal examined almost 1,600 psychiatric patients in southern Italy and found that cannabis use was associated with a ten-fold increase in violence.
The most obvious way that cannabis fuels violence in psychotic people is through its tendency to cause paranoia—something even cannabis advocates acknowledge the drug can cause. The risk is so obvious that users joke about it and dispensaries advertise certain strains as less likely to induce paranoia. And for people with psychotic disorders, paranoia can fuel extreme violence. A 2007 paper in the Medical Journal of Australia on 88 defendants who had committed homicide during psychotic episodes found that most believed they were in danger from the victim, and almost two-thirds reported misusing cannabis—more than alcohol and amphetamines combined.
Yet the link between marijuana and violence doesn’t appear limited to people with preexisting psychosis. Researchers have studied alcohol and violence for generations, proving that alcohol is a risk factor for domestic abuse, assault, and even murder. Far less work has been done on marijuana, in part because advocates have stigmatized anyone who raises the issue. But studies showing that marijuana use is a significant risk factor for violence have quietly piled up. Many of them weren’t even designed to catch the link, but they did. Dozens of such studies exist, covering everything from bullying by high school students to fighting among vacationers in Spain.
In most cases, studies find that the risk is at least as significant as with alcohol. A 2012 paper in the Journal of Interpersonal Violence examined a federal survey of more than 9,000 adolescents and found that marijuana use was associated with a doubling of domestic violence; a 2017 paper in Social Psychiatry and Psychiatric Epidemiology examined drivers of violence among 6,000 British and Chinese men and found that drug use—the drug nearly always being cannabis—translated into a five-fold increase in violence.
Today that risk is translating into real-world impacts. Before states legalized recreational cannabis, advocates said that legalization would let police focus on hardened criminals rather than marijuana smokers and thus reduce violent crime. Some advocates go so far as to claim that legalization has reduced violent crime. In a 2017 speech calling for federal legalization, U.S. Senator Cory Booker said that “states [that have legalized marijuana] are seeing decreases in violent crime.” He was wrong.
The first four states to legalize marijuana for recreational use were Colorado and Washington in 2014 and Alaska and Oregon in 2015. Combined, those four states had about 450 murders and 30,300 aggravated assaults in 2013. Last year, they had almost 620 murders and 38,000 aggravated assaults—an increase of 37 percent for murders and 25 percent for aggravated assaults, far greater than the national increase, even after accounting for differences in population growth.
Knowing exactly how much of the increase is related to cannabis is impossible without researching every crime. But police reports, news stories, and arrest warrants suggest a close link in many cases. For example, last September, police in Longmont, Colorado, arrested Daniel Lopez for stabbing his brother Thomas to death as a neighbor watched. Daniel Lopez had been diagnosed with schizophrenia and was “self-medicating” with marijuana, according to an arrest affidavit.
In every state, not just those where marijuana is legal, cases like Lopez’s are far more common than either cannabis or mental illness advocates acknowledge. Cannabis is also associated with a disturbing number of child deaths from abuse and neglect—many more than alcohol, and more than cocaine, methamphetamines, and opioids combined—according to reports from Texas, one of the few states to provide detailed information on drug use by perpetrators.
These crimes rarely receive more than local attention. Psychosis-induced violence takes particularly ugly forms and is frequently directed at helpless family members. The elite national media prefers to ignore the crimes as tabloid fodder. Even police departments, which see this violence up close, have been slow to recognize the trend, in part because the epidemic of opioid overdose deaths has overwhelmed them.
So the black tide of psychosis and the red tide of violence are rising steadily, almost unnoticed, on a slow green wave.
For centuries, people worldwide have understood that cannabis causes mental illness and violence—just as they’ve known that opiates cause addiction and overdose. Hard data on the relationship between marijuana and madness dates back 150 years, to British asylum registers in India. Yet 20 years ago, the United States moved to encourage wider use of cannabis and opiates.
In both cases, we decided we could outsmart these drugs—that we could have their benefits without their costs. And in both cases we were wrong. Opiates are riskier, and the overdose deaths they cause a more imminent crisis, so we have focused on those. But soon enough the mental illness and violence that follow cannabis use will also be too widespread to ignore.
Whether to use cannabis, or any drug, is a personal decision. Whether cannabis should be legal is a political issue. But its precise legal status is far less important than making sure that anyone who uses it is aware of its risks. Most cigarette smokers don’t die of lung cancer. But we have made it widely known that cigarettes cause cancer, full stop. Most people who drink and drive don’t have fatal accidents. But we have highlighted the cases of those who do.
We need equally unambiguous and well-funded advertising campaigns on the risks of cannabis. Instead, we are now in the worst of all worlds. Marijuana is legal in some states, illegal in others, dangerously potent, and sold without warnings everywhere.
But before we can do anything, we—especially cannabis advocates and those in the elite media who have for too long credulously accepted their claims—need to come to terms with the truth about the science on marijuana. That adjustment may be painful. But the alternative is far worse, as the patients at Mid-Hudson Forensic Psychiatric Institute—and their victims—know.
Alex Berenson is a graduate of Yale University with degrees in history and economics. He began his career in journalism in 1994 as a business reporter for the Denver Post, joined the financial news website TheStreet.com in 1996, and worked as an investigative reporter for The New York Times from 1999 to 2010, during which time he also served two stints as an Iraq War correspondent. In 2006 he published The Faithful Spy, which won the 2007 Edgar Award for best first novel from the Mystery Writers of America. He has published ten additional novels and two nonfiction books, The Number: How the Drive for Quarterly Earnings Corrupted Wall Street and Corporate Americaand Tell Your Children: The Truth About Marijuana, Mental Illness, and Violence.







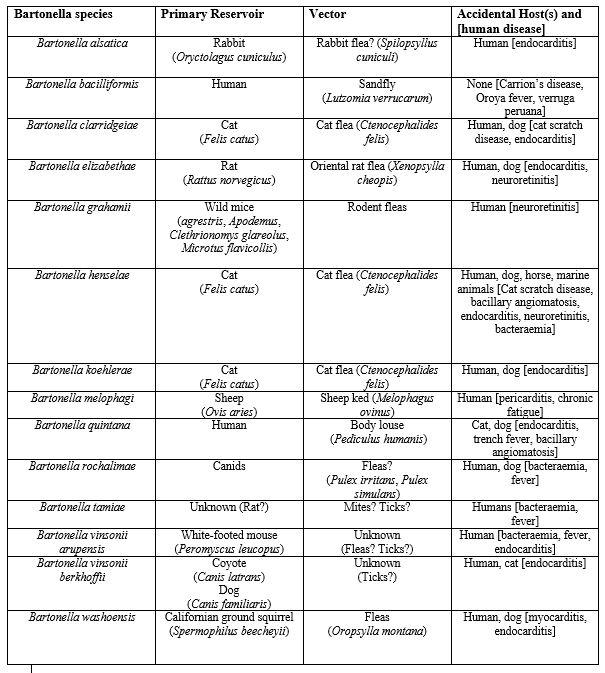
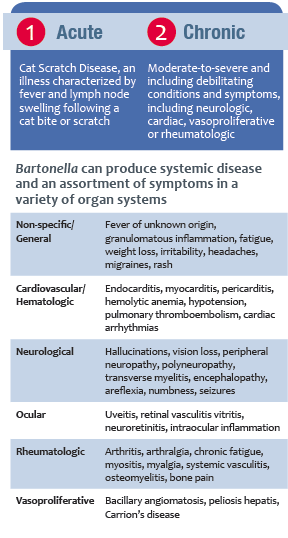 Despite these findings, reported cases are often focused on acute infections, such as CSD, Trench Fever, and Carrion’s disease, that show typical clinical signs making them easier to diagnose. Acute infections are likely to be diagnosed and treated quickly, but the story is different for chronically ill patients that are atypical or asymptomatic.
Despite these findings, reported cases are often focused on acute infections, such as CSD, Trench Fever, and Carrion’s disease, that show typical clinical signs making them easier to diagnose. Acute infections are likely to be diagnosed and treated quickly, but the story is different for chronically ill patients that are atypical or asymptomatic.


 southeastern United States, have
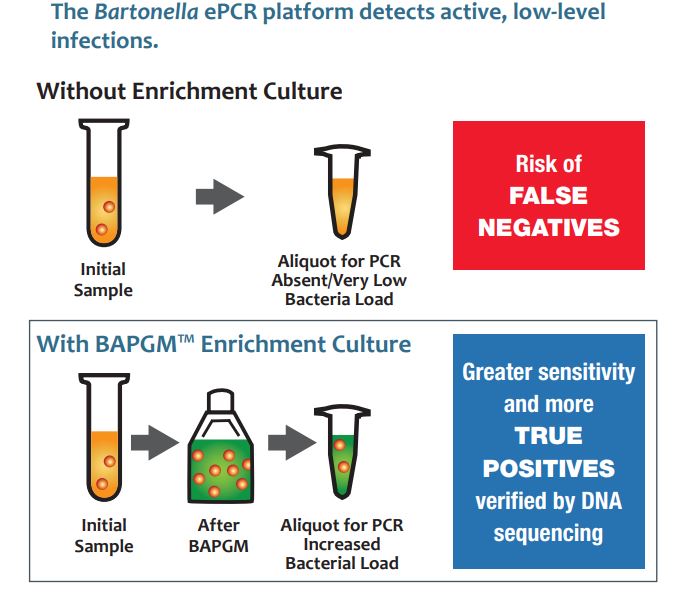
southeastern United States, have  medium based on insect cell growth requirements has shown increased growth for multiple species. Successfully matching the strict growth requirements for Bartonella species makes it more likely to isolate and detect them. Patented BAPGM (Bartonella Alphaproteobacteria growth medium) is used in combination with PCR at Galaxy Diagnostics to maximize sensitivity.
medium based on insect cell growth requirements has shown increased growth for multiple species. Successfully matching the strict growth requirements for Bartonella species makes it more likely to isolate and detect them. Patented BAPGM (Bartonella Alphaproteobacteria growth medium) is used in combination with PCR at Galaxy Diagnostics to maximize sensitivity.