General Symptom Questionnaire-30 (GSQ-30): A Brief Measure of Multi-System Symptom Burden in Lyme Disease
https://www.frontiersin.org/articles/10.3389/fmed.2019.00283/full
The General Symptom Questionnaire-30 (GSQ-30): A Brief Measure of Multi-System Symptom Burden in Lyme Disease
Introduction: The multi-system symptoms accompanying acute and post-treatment Lyme disease syndrome pose a challenge for time-limited assessment. The General Symptom Questionnaire (GSQ-30) was developed to fill the need for a brief patient-reported measure of multi-system symptom burden. In this study we assess the psychometric properties and sensitivity to change of the GSQ-30.
Materials and Methods: 342 adult participants comprised 4 diagnostic groups: Lyme disease (post-treatment Lyme disease syndrome, n = 124; erythema migrans, n = 94); depression, n = 36; traumatic brain injury, n = 51; healthy, n = 37. Participants were recruited from clinical research facilities in Massachusetts, Maryland, and New York. Validation measures for the GSQ-30 included the Patient Health Questionnaire-4 for depression and anxiety, visual analog scales for fatigue and pain, the Sheehan Disability Scale for functional impairment, and one global health question. To assess sensitivity to change, 53 patients with erythema migrans completed the GSQ-30 before treatment and 6 months after 3 weeks of treatment with doxycycline.
Results: The GSQ-30 demonstrated excellent internal consistency (Cronbach α = 0.95). The factor structure reflects four core domains: pain/fatigue, neuropsychiatric, neurologic, and viral-like symptoms. Symptom burden was significantly associated with depression (rs = 0.60), anxiety (rs = 0.55), pain (rs = 0.75), fatigue (rs = 0.77), functional impairment (rs = 0.79), and general health (rs = −0.58). The GSQ-30 detected significant change in symptom burden before and after antibiotic therapy; this change correlated with change in functional impairment. The GSQ-30 total score significantly differed for erythema migrans vs. three other groups (post-treatment Lyme disease syndrome, depression, healthy controls).
The GSQ-30 total scores for traumatic brain injury and depression were not significantly different from post-treatment Lyme disease syndrome.
Conclusions and Relevance: The GSQ-30 is a valid and reliable instrument to assess symptom burden among patients with acute and post-treatment Lyme disease syndrome and is sensitive in the detection of change after treatment among patients with erythema migrans. The GSQ-30 should prove useful in clinical and research settings to assess multi-system symptom burden and to monitor change over time. The GSQ-30 may also prove useful in future precision medicine studies as a clinical measure to correlate with disease-relevant biomarkers.
_______________
**Comment**
The good thing about this is it clearly shows that there is a significant change in symptom burden after antibiotic therapy. In other words – the proof is in the pudding. If you treat this properly, patients will improve. This should shut the IDSA/CDC up, but it won’t.
Unfortunately they decided to keep the CDC/IDSA “Post Treatment Lyme Disease Syndrome” moniker rather than deal with persistent infection. Until this issue is laid to rest, research will be skewed and authorities will not treat this appropriately. There’s over 700-peer reviewed articles showing the persistence of Lyme disease: Peer-Reviewed Evidence of Persistence of Lyme:MSIDS copy
Another good thing this shows is the seriousness of symptoms that patients can be left with – the total scores aren’t significantly different from those with traumatic brain injury or depression. The symptoms are very, very real and very, very serious.
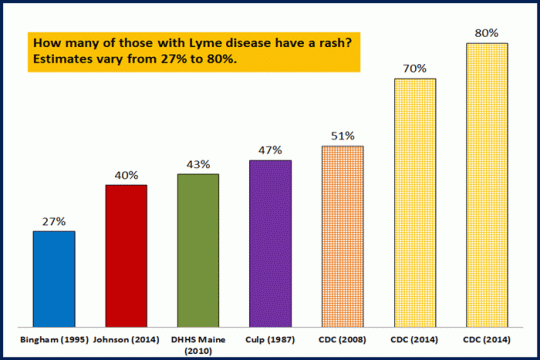
Please remember that those with the EM rash is highly variable: https://madisonarealymesupportgroup.com/2019/02/22/why-mainstream-lyme-msids-research-remains-in-the-dark-ages/
It is a bit of a head-scratcher as to why the authors felt compelled to do this study when a validated symptom questionnaire already exists: https://madisonarealymesupportgroup.com/2017/09/05/empirical-validation-of-the-horowitz-questionnaire-for-suspected-lyme-disease/
https://madisonarealymesupportgroup.com/wp-content/uploads/2016/01/symptomlist.pdf
This symptom checklist is far more accurate than any serology testing at this point. Doctors would be wise to utilize it. There are also checklists for Babesia and Bartonella as well:

 Brian A. Fallon
Brian A. Fallon Nevena Zubcevik3,4,
Nevena Zubcevik3,4,  Clair Bennett
Clair Bennett Shreya Doshi
Shreya Doshi Alison W. Rebman
Alison W. Rebman Ronit Kishon
Ronit Kishon James R. Moeller
James R. Moeller Nadlyne R. Octavien
Nadlyne R. Octavien John N. Aucott
John N. Aucott