Diagnosing Lyme Disease in Children With Neuropsychiatric Illness
Please see comment at end of article
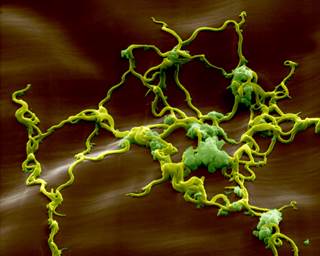
Lyme disease can present with a multitude of symptoms that often mimick other diseases, making differential diagnosis difficult. Neurologic involvement has been reported in up to 15% of untreated Borrelia burgdorferi infection,1 which can be devastating, particularly in children and young adults, who have been reported to be more at risk. According to the US Centers for Disease and Control and Prevention (CDC), Lyme disease is on the rise.2 Each year, at least 300,000 people in the United States are diagnosed with Lyme disease, with the highest infection rates occurring in children age 5 to 10 years.2,3
Lyme neuroborreliosis can affect any part of the nervous system, and there are a wide range of neurologic and psychiatric symptoms that can manifest weeks, months, or even years after the initial infection. For example, memory impairment, irritability, and somnolence have been reported months to years after the initial classic presentation of Lyme disease, and encephalopathy has been reported to occur more than 10 years after the onset of the disease.4,5 The presenting neurologic symptoms, including facial palsy, debilitating fatigue, various levels of cognitive loss, psychiatric symptoms, behavior changes, and learning difficulties have a significant and negative effect on the critical stages of child development, including school attendance and decline in school performance.6,7
Full recovery from Lyme neuroborreliosis can be achieved when the disease is diagnosed promptly and accurately and appropriate treatment is initiated. However, there is a general lack of understanding of Lyme disease among physicians, and Lyme neuroborreliosis is notoriously very difficult to recognize and diagnose in children. Shannon Delaney, MD, MA, director of child and adolescent research and evaluation at the Lyme and Tick-Borne Diseases Research Center at Columbia University Medical Center in New York told Rheumatology Advisor that,
“Neuroborreliosis can be missed because it is not considered in the differential [diagnosis] and because spinal taps are often not [performed] unless a child has very obvious symptoms of encephalitis or meningitis.”
The overlap of symptoms with other neurologic, cognitive, and psychiatric symptoms contributes to the delayed diagnosis or the misdiagnosis. For example, case reports of neuropsychological manifestations of Lyme disease include Tourette syndrome, acute delirium, catatonia, and psychosis.8
Dr Delaney advises that,
“Any child with acute onset neuropsychiatric symptoms, such as [obsessive-compulsive disorder], psychosis, restricted eating, sensory issues, urinary frequency, anxiety, cognitive dysfunction, or extreme fatigue should be given a set of lab tests to rule out typical infectious causes of Pediatric Acute-onset Neuropsychiatric Syndrome/Pediatric Autoimmune Neuropsychiatric Disorder Associated with Streptococcal Infections.”
Dr Delaney added,
“Testing should include a Lyme ELISA [enzyme-linked immunosorbent assay], preferably Borrelia burgdorferi C6 peptide, and a Lyme Western blot to evaluate for exposure to Lyme disease.”
Because symptoms of Lyme neuroborreliosis affect the joints, muscle, and the central and peripheral nervous systems, health professionals from many disciplines, including neurology and psychiatry, need to be able to recognize the clinical presentations, know the essential diagnostic tests, and understand the treatment approach. Erythema migrans is a distinct early presentation of localized Lyme disease,8 and for the experienced physician, this presentation can be sufficient for a clinical diagnosis. Serologic testing at this early disease stage is of limited diagnostic value because of the high incidence of false negative results.
When serologic testing is indicated, the Infectious Diseases Society of America (IDSA) recommend enzyme immunoassay for Lyme-specific antibodies, confirmed with Western immunoblot assay for immunoglobin G; however, many physicians struggle with the correct interpretation of Western blot results.9,10 Dr Delaney cautions,
“Clinicians should be aware that the 2-tier method of testing (ELISA and Western blot), while informative, can have false negative [results] and, less frequently, false positive [results].” Furthermore, although several tests for Lyme disease are available commercially, many are not validated for clinical use, and the CDC strongly warns against their use, as they have been associated with high levels of misdiagnosis.8
The IDSA recommends antibiotics for the treatment of Lyme disease for a period of 10 to 21 days for early disease and 2 to 4 weeks for late disease.9 Despite the recommendations, studies that distinguish the treatment of Lyme disease from that of Lyme neuroborreliosis are lacking.9 In fact, a systematic review that examined antibiotic treatment for Lyme neuroborreliosis in 450 participants included no trials conducted in the United States.11 The review found no clear evidence for the additional efficacy of repeated antibiotics beyond the initial treatment.11
In addition, prolonged use of antibiotics to treat post-Lyme disease symptoms has not been shown to be efficacious and is generally not recommended, as fatalities from Clostridium difficile and Candida parapssilosis have been reported.8
“Clinically, we do recognize that there are a subset of patients who only get better after a repeated course of antibiotics,” said Dr Delaney, adding, “In the future as the science progresses, hopefully, we will be able to make use of blood tests that provide biomarkers indicating who needs additional antibiotic therapy and who needs another approach. This is the age of precision medicine and our goal at Columbia is to help in the identification of these essential biomarkers that will help guide treatment.”
The need for additional research is evident to better define the optimal use of antibiotics for the treatment of Lyme neuroborreliosis.11 The effect of long-term use of antibiotics also deserves attention. Inappropriate antibiotic use can alter the balance of the gut microbiome and may lead to side effects. The effect of long-term antibiotics on the gut microbiome is an area of emerging study and should provide very useful information in the future regarding whether or not the alterations themselves are contributing to ongoing symptoms. Until more research is available to better guide the management of the neurologic manifestations of B burgdorferi infection, it is important that physicians have heightened awareness of Lyme disease. They must also have a clinical suspicion of Lyme neuroborreliosis in children who present with neuropsychiatric illness and must diagnose the disease promptly and provide appropriate treatment, which may include referral for appropriate symptom management.
References
- Marques AR. Lyme neuroborreliosis. Continuum (Minneap Minn). 2015;21(6):1729-1744.
- US Centers for Disease Control and Prevention. Lyme disease. Lyme disease graphs. https://www.cdc.gov/lyme/stats/graphs.html. Updated November 1, 2017. Accessed July 17, 2018.
- US Centers for Disease Control and Prevention. Lyme disease. How many people get Lyme disease? https://www.cdc.gov/lyme/stats/humancases.html. Updated September 30, 2015. Accessed July 17, 2018.
- Bloom BJ, Wyckoff PM, Meissner HC, Steere AC. Neurocognitive abnormalities in children after classic manifestations of Lyme disease. Pediatr Infect Dis J. 1998;17(3):189-196.
- Szer IS, Taylor E, Steere AC. The long-term course of Lyme arthritis in children. N Engl J Med. 1991;325(3):159-163.
- Lyme Disease Action. Neurology and Psychiatry. Involvement of the Central and Peripheral Nervous System. https://www.lymediseaseaction.org.uk/about-lyme/neurology-psychiatry/. Updated November 26, 2016. Accessed July 17, 2018.
- Cameron D. Adolescents with Lyme disease. http://danielcameronmd.com/adolescent-lyme-disease/. 2018. Accessed July 17, 2018.
- Koster MP, Garro A. Unraveling diagnostic uncertainty surrounding Lyme disease in children with neuropsychiatric illness.Child Adolesc Psychiatr Clin N Am. 2018;27(1):27-36.
- Wormser GP, Dattwyler RJ, Shapiro ED, et al. The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis. 2006;43(9):1089-1134.
- Conant JL, Powers J, Sharp G, Mead PS, Nelson CA. Lyme disease testing in a high-incidence state: clinician knowledge and patterns. Am J Clin Pathol. 2018;149(3):234-240.
- Cadavid D, Auwaerter PG, Rumbaugh J, Gelderblom H. Antibiotics for the neurological complications of Lyme disease. Cochrane Database Syst Rev. 2016;12:CD006978.
__________________
**Comment**
A few points of contention:
- While the EM rash IS an early symptom that clinically proves the person has Lyme, many never see or have a rash at all or it is certainly not a “typical” EM rash. Clinicians need education in this.
- Numbers are notoriously low on all things Lyme/MSIDS, including this supposed 15% who have neurologic involvement. Everyone I work with is in this category so I’m either just a lucky-duck or the numbers are far higher in the real world. I suspect the latter.
- Testing for Lyme/MSIDS IS ABYSMAL. Absolutely worthless. It misses over half of all cases. I’m thankful the article states professionals need to be educated because this is a CLINICAL DIAGNOSIS. Anyone who says otherwise is smoking something. Again, clinicians need education.
- Where the article really falls apart is in the treatment section. This article ONLY discusses the IDSA approach which is essentially 21 days of doxycycline despite the presentation. I couldn’t disagree more. If you read the ILADS guidelines, you will discover that treatment is far more complex. There are many who have gotten well or improved dramatically with this approach. The reason for this is numerous: 1) we are typically infected with more than borrelia, necessitating numerous drugs 2) all of these pathogens are stealthy and many are persistent requiring far longer treatment courses than appreciated 3) these pathogens work together to suppress the immune system and complicate the picture requiring numerous treatments
- The Cochrane review of antibiotics for neuro-Lyme mentioned had numerous flaws: none included a placebo control, only ONE was blinded, most were not adequately powered for non-inferiority comparison, they ONLY investigated four antibiotics: penicillin G & ceftriaxone in 4 studies, doxycycline in 3 studies, cefotaxime in two studies, and amoxicillin vs. placebo for only 3 months following initial treatment with IV ceftriaxone. (I consider many of these antibiotics poor choices for Lyme and I’ve never taken two of them. I had to look one up as I’d NEVER even heard of it!) The trials measured efficacy using heterogeneous physician‐ or patient‐reported outcomes, or both. None of the studies reported on the proposed primary outcome, ‘Improvement in a measure of overall disability in the long term (three or more months).’ The quality of adverse event reporting was low. So, as far as I’m concerned this “review” is extremely weak yet it’s presented as evidence that long-term antibiotics do not work. Please see this article for comparison: https://madisonarealymesupportgroup.com/2017/07/09/idsa-founder-used-potent-iv-antibiotics-for-chronic-lyme/ Also, I would not be writing this article without the judicious use of long-term antibiotics.
- It’s interesting that although the author disses long-term antibiotics using the IDSA clap-trap and an extremely weak and flawed review, she did include the quote from Dr. Delaney,
“Clinically, we do recognize that there are a subset of patients who only get better after a repeated course of antibiotics,” said Dr Delaney
Hmmm….that appears to be a cognitive disconnect.
To clear the record: nearly all of us out here in Lymeland HATE taking antibiotics.
We take them because they often work better than other things we’ve tried. They are also more affordable than other many other options.
But, if we could press some magic button, believe me – we would.
I find it interesting that people with acne can take antibiotics forever, yet patients with life-threatening tick-borne illness are told extended antibiotics can give them C-diff, therefore they are bad and shouldn’t be considered. Period.
This disconnect is wholly unacceptable.
