https://www.sciencedaily.com/releases/2018/04/180402171044.htm University of Maryland. ScienceDaily, 2 April 2018.
How a protein helps bacteria outsmart the human immune system
Findings have major implications for tick-borne diseases like Lyme disease
Summary:
New research has uncovered a mechanism by which the bacteria that cause Lyme disease fight innate immune responses, and observed a never-before-seen phenomena demonstrating the bacteria can spring back in the body weeks later. Understanding this type of bacteria, one of only a few pathogens that can actually persist in the body for long periods of time, has major implications for treatment of tick-borne diseases like Lyme disease.
FULL STORY:
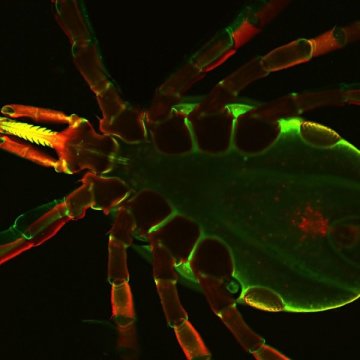
Ixodes scapularis ticks transmit the pathogens of Lyme disease, resulting a multisystem illness in a variety of animals and humans. The image shows bottom side a live Ixodes tick as seen under a confocal immunofluorescence microscope.
Credit: Dr. Utpal Pal, University of Maryland
Researchers have uncovered a mechanism by which the bacteria that cause Lyme disease persist in the human body and fight the body’s early, innate immune responses. Dr. Utpal Pal, Professor in Veterinary Medicine at the University of Maryland (UMD), has been studying the Borrelia burgdorferi bacteria throughout his 12 years with UMD, and his work has already produced the protein marker used to identify this bacterial infection in the body. Now, Dr. Pal has isolated a protein produced by the bacteria that disables one of the body’s first immune responses, giving insight into mechanisms that are largely not understood.
He has also observed a never-before-seen phenomena demonstrating that even without this protein and with the immune system responding perfectly, the bacteria can spring back in the body weeks later. Understanding this type of bacteria, which is among only a few pathogens that can actually persist in the body for long periods of time, has major implications for the treatment of tick-borne diseases like Lyme disease, which is an increasingly chronic and consistently prevalent public health issue.
“Most people don’t realize that they actually are walking around with more bacterial cells in their bodies than their own cells, so we are really bags of bacteria,” explains Pal. “Most are good, but the second your body detects something that is a pathogen and can cause disease, your immune system starts to work.” The body sends a first, nonspecific wave of attack to kill the bacteria detected that doesn’t belong. This happens within a few hours to days. If this doesn’t work, it takes seven to ten days to learn about the enemy and send a large second wave of reinforcements to kill what is left. “Lyme disease is actually caused by your immune system,” explains Pal. “This bacteria wins the first battle, and your body overreacts so much that it causes intense inflammation in all the joints and areas that the bacteria spreads by sending so many reinforcements to kill it. Borrelia is then killed, but the inflammation remains and causes many of your symptoms for Lyme disease. That is why killing Borrelia in the first wave of immunity is so important.”
The Centers for Disease Control and Prevention (CDC) estimate about 300,000 cases of Lyme disease annually in the United States. However, these cases are largely underestimated and reported due to the attention given to mosquito-transmitted diseases like malaria.
“The majority of all vector-borne diseases in the US are actually tick-borne, and 6 of the 15 distinct tick diseases are transmitted by the Ixodes tick we study in our lab,” says Pal. “The symptoms of these diseases present similarly to many other illnesses and are hard to pin down, so they are vastly underreported and an even bigger public health concern locally and globally than people realize.”
Now, chronic Lyme disease is a growing concern. Six to twelve months after traditional antibiotic therapy, many people have non-objective symptoms that return with varying intensity and no current treatment strategy, known as Post-Treatment Lyme Disease Syndrome.
Dr. Pal’s research has shed some light on this issue and paved the way for future research and treatment options by discovering that even without the protein used to beat the first wave of immune defense, infection can reoccur in the body weeks later.
“This means there is a second line of defense for Borrelia just like for our body’s immune system. This had never been observed before and gives us insight into what could be causing these chronic Lyme disease cases,” explains Pal.
Dr. Pal is frequently consulted for his expertise and has written books on this highly versatile bacteria. The federal government has recently put more emphasis on tick-borne disease research and a major public health issue with the passage of the 21st Century Cures Act. As part of this, Dr. Pal was asked to serve on a Tick-Borne Disease Working Group Subcommittee for the U.S. Department of Health & Human Services (DHHS) focused on vaccines and therapeutics for tick-borne diseases, driving future research in the field. Dr. Pal currently holds two concurrent multi-million dollar RO1 grants from the National Institutes of Health (NIH) for this work, only granted for highly important and influential research.
“I am fascinated by Borrelia, and this discovery will open the door for much more work to treat and control important diseases like Lyme disease,” says Pal.
Journal Reference: Quentin Bernard, Alexis A. Smith, Xiuli Yang, Juraj Koci, Shelby D. Foor, Sarah D. Cramer, Xuran Zhuang, Jennifer E. Dwyer, Yi-Pin Lin, Emmanuel F. Mongodin, Adriana Marques, John M. Leong, Juan Anguita, Utpal Pal. Plasticity in early immune evasion strategies of a bacterial pathogen. Proceedings of the National Academy of Sciences, 2018; 201718595 DOI: 10.1073/pnas.1718595115
