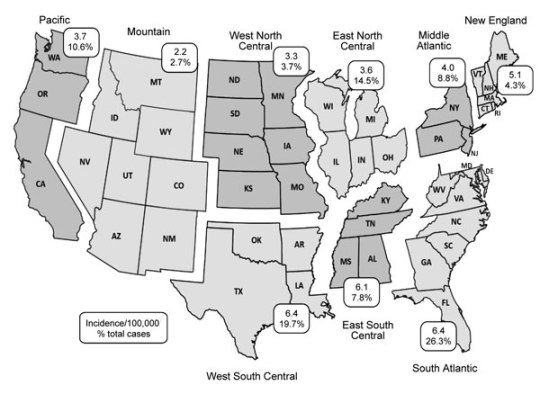
https://wwwnc.cdc.gov/eid/article/22/10/16-0115-f2 Figure 2. Geographic distribution of cat-scratch disease by US census division, United States, 2005–2013. Rates are reported as average incidence per 100,000 population per year. During the study period, there were <10 cases in Alaska and <10 cases in Hawaii. https://wwwnc.cdc.gov/eid/article/22/10/16-0115_article
http://www.northcarolinahealthnews.org/2016/12/19/north-carolina-ranks-as-high-risk-zone-for-cat-scratch-disease/ By Thomas Goldsmith
“North Carolina cat owners who have a child between 5 and 9 are among groups with the highest national household risk of cat scratch disease.
CDC guidelines recommend that owners keep cats inside at all times as part of guidelines to reduce incidence of cat scratch disease.
That was among the takeaways from a talk by Centers for Disease Control epidemiologist Christina Nelson, who presented results from the paper, “Cat Scratch Disease in the United States: Sinking Our Claws into the Data,” at the One Medicine conference this month at Research Triangle Park.
‘Efforts should target cat owners in the South, with children in the household, and/or people with immunocompromised conditions,’ Nelson said when talking about ways to combat the disease.
Cat scratch fever, or bartonella, as it’s known to scientists, attracts a lot of attention, perhaps because three of 10 American households have cats, perhaps because of its mention in a risque 1970s rock song, Nelson said. No matter the reason, an edition of Emerging Infectious Diseases in which the Nelson’s article on the disease ran attracted the largest number of online visits in the academic journal’s history.
Cat scratch disease often runs its course within two to four months, but related disorders can require antibiotics or other treatment.
The disease is caused by the spread of the bacterium Bartonella henselae through cat fleas, then to humans via animals’ scratches and sometimes bites. Primary symptoms include fever and enlargement of lymph nodes near the scratch site, but other manifestations can include swelling of the retina or Parinaud oculoglandular syndrome (swollen eye accompanying swollen nodes) as well as bone, brain or heart infections, according to the paper.
Because physicians are not required to report cat scratch disease to public health authorities, Nelson and colleagues examined diagnoses based on an insurance industry resource, Truven Health MarketScan. The database details diagnoses of company-insured employees and their families. That meant people over 65, insured by Medicare, were not included.
‘There were about 35 million people involved,’ Nelson said. ‘It’s an enormous database.’
They found more than 500 inpatients and more than 12,500 outpatients are treated for cat scratch disease annually.
Among the findings of the study:
With an incidence of 6.1-6.4 per 100,000 population, North Carolina lies in the geographic region, the South Atlantic, with the highest U.S. incidence of cat scratch disease. More than one in four U.S. cases occurs in this region.
An average of 4.5 patients out of 100,000 received outpatient treatment for the disease; 19 patients out of 100,000 required inpatient treatment, for an average of three days.
Children age 5 to 9 accounted for the highest incidence of cat scratch fever cases — 9 outpatient cases and .4 inpatient cases per 100,000.
Females made up more than six in 10 outpatients and 55.6 percent of inpatients.
Mean cost of care per inpatient was $244, with inpatient treatment and followup costing $13,663. Overall disease costs nationally were nearly $10 million.
Nelson noted that researchers were puzzled by an increase in cat scratch disease cases in January. Attendees at the RTP conference immediately suggested an answer.“Christmas kittens!” they chorused.
Among the things the study did not say: That people can get the disease from kissing cats.
Nonetheless, news outlets took the CDC study and ran with it, in some cases, a bit too far. NPR had to run a correction: noting that people cannot get the disease from kissing cats.
‘This is incorrect. People can get the disease if an infected cat licks a scratch or wound,’ the correction read.
How to keep incidence down
Speakers at the conference suggested using the Healthy Pets Healthy People site as a resource for dealing with cat scratch disease.
The CDC suggested these means to reduce incidence:
People bitten by cats should Immediately clean the bite with soap and water
People, especially those with weakened immune systems, should wash their hands with soap and water after playing with cats.
Because kittens less than a year old are more likely to harbor the bacterium, people who have weakened immune systems should adopt cats older than one year.
People shouldn’t play with or pet feral cats.
Cats shouldn’t be allowed to lick open wounds.
Cats should have nails trimmed, use vet-approved flea products, and be checked regularly with a flea comb.
Cats should stay indoors to reduce exposure to fleas and to avoid fights with flea-infected animals.
‘Some shelters will not adopt a cat out unless the owners pledge never to let the cat outside,’ audience member Marcia Herman-Giddens, a Triangle area teacher and researcher, noted during a discussion period.CSD belongs to the disease group Bartonellosis
‘Bartonellosis is a group of emerging infectious diseases caused by bacteria belonging to the Bartonella genus.
Bartonella includes at least 22 named species of bacteria that are mainly transmitted by carriers (vectors), including fleas, lice, or sandflies. Both domestic and wild animals can be infected with Bartonella species by these vectors.
Among the Bartonella species, at least 14 have been implicated in diseases that can be transmitted from animals to people (zoonotic disease). Of these zoonotic species, several may be transmitted to humans by companion animals (dogs and cats), typically through a bite or scratch.’
Source: National Organization for Rare Disorders
http://www.columbia-lyme.org/patients/tbd_bartonella.html “Bartonella are also found in numerous arthropods, biting flies, and ticks. The evidence for ticks as vectors is circumstantial but fairly strong. Recent studies in both the United States and Europe have found that Ixodes ticks harbor B. henselae in addition to Borrelia, Babesia and Anaplasma organisms; in fact, a 2004 PCR analysis of I. Scapularis ticks in New Jersey discovered that a higher percentage of ticks were infected with B. henselae than any of these other pathogens. In addition, B. henselae has been detected in the spinal fluid of patients co-infected with Borrelia burgdorferi, the agent of Lyme disease.”
For more on Bartonella:
https://madisonarealymesupportgroup.com/2016/01/03/bartonella-treatment/ (Treatment)
https://madisonarealymesupportgroup.com/2016/08/09/a-bartonella-story/
https://madisonarealymesupportgroup.com/2016/02/08/new-bartonella-species/
https://madisonarealymesupportgroup.com/2015/07/23/understanding-bartonella/ (Webinar by Galaxy Labs and leading Bart expert Dr. Breitschwerdt, DVM and B. Robert Mozayeni, MD.
https://madisonarealymesupportgroup.com/2016/04/24/gardasil-and-bartonella/
