Massage is one of the oldest and simplest forms of medical care used to promote general well-being and ease pain and anxiety. Your skin is your largest sensory organ and specialized receptors in the dermis, the second layer of skin, react to external stimuli such as heat, cold and pressure by sending messages through your nervous system to your brain that stimulate the release of endorphins.
Endorphins promote relaxation and a sense of well-being, relieve pain and reduce levels of stress chemicals such as cortisol and noradrenaline, thereby slowing your heart rate, respiration and metabolism, and lowering your blood pressure.
Deeper, more vigorous massage stimulates blood circulation to improve the supply of oxygen and nutrients to body tissues and helps your lymphatic system flush away waste products. It eases tense and knotted muscles and stiff joints, improving mobility and flexibility.
Massage is also said to increase activity of the vagus nerve, one of 10 cranial nerves that affects the secretion of food absorption hormones, heart rate and respiration.
It has proven to be an effective therapy for a variety of health conditions — particularly stress-related tension, which can play a significant role in the development of both psychological and physical health problems. Here, I review six areas where massage has been shown to produce beneficial results: pain, mental health, inflammation, immune function, muscle spasms and flexibility.
Massage Therapy for Pain Relief
Pain is an extremely common problem — so much so, deaths from opioid addiction are at an all-time high, killing an estimated 47,600 Americans in 2017 alone.1 As of June 2017, opioids became the leading cause of death among Americans under the age of 50. Massage is just one of many alternative pain treatments that can be helpful.
A systematic review and meta-analysis2 published in 2016 included 60 high-quality and seven low-quality studies that looked into the use of massage for various types of pain, including muscle and bone pain, headaches, deep internal pain, fibromyalgia and spinal cord pain.
The review revealed massage therapy relieves pain better than getting no treatment at all, and when compared to other pain treatments such as acupuncture and physical therapy, massage therapy still proved beneficial.
More specifically, studies have shown massage therapy can relieve pain associated with:
• Tension headaches and migraines3,4 — In one study,5 participants who received two 30-minute traditional massages for five weeks reported a decrease in the frequency of migraine attacks compared to controls who did not receive massage therapy. They also had fewer sleep disturbances and testing revealed an increase in serotonin.
In another,6 the effect of Thai massage — which focuses on compression, stretching, pulling and rocking motions7 — was assessed on patients with either chronic tension headaches or migraines.
Participants received either ultrasound treatment or three Thai massage sessions per week for three weeks. Those receiving Thai massage reported an increase in pain pressure threshold, while those in the ultrasound group experienced a decrease. Both groups had a significant reduction in migraine intensity.
• Labor pain — According to Rebecca Dekker, who has a Ph.D. in nursing and founded Evidence Based Birth, one hypothesis for how massage works to reduce pain is the gate control theory.8“Gentle, or nonpainful massage, can act on the Gate Control Method by flooding the body with pleasant sensations so that the brain does not perceive the painful sensations as much,” she says.
Intense, deep massage, on the other hand, is thought to act via diffuse noxious inhibitory control. “The idea is that the stimulation from painful massage is so intense that it stimulates the brain to release its own natural pain-relieving hormones called endorphins.
Your body is then flooded with endorphins that help you perceive less pain from contractions,” Dekker says, adding, “Researchers also think that massage might work by decreasing cortisol, or stress hormones and increasing levels of serotonin and dopamine in your brain.”
• Fibromyalgia — The National Fibromyalgia and Chronic Pain Association recommends massage for fibromyalgia pain, noting it can ease symptoms.9
A systematic review and meta-analysis10 of nine randomized controlled trials involving 404 patients looking at the effects of massage therapy for fibromyalgia concluded “Massage therapy with duration ≥5 weeks had beneficial immediate effects on improving pain, anxiety and depression in patients with FM [fibromyalgia]. Massage therapy should be one of the viable complementary and alternative treatments for FM.”
• Cancer pain — According to the Australian Cancer Council,11 massage therapy can be helpful for relieving side effects associated with conventional cancer treatment, citing evidence showing massage can reduce pain, fatigue, nausea, anxiety and depression in cancer patients.
The Council notes that while some worry cancer may spread through massage, such fears are unfounded, and light massage “can safely be given to people at all stages of cancer,” as “the circulation of lymph — from massage or other movement — does not cause cancer to spread.”
A scientific paper12 discussing massage therapy for cancer patients published in Current Oncology in 2007 also noted that massage is “very safe” and that “complications are rare … Adverse effects were associated mainly with massage delivered by laypeople and with techniques other than Swedish massage.”
One of the largest observational studies13 on massage and cancer was done at the Memorial Sloan-Kettering Cancer Center in New York City, which evaluated symptom scores for pain, fatigue, stress and anxiety, nausea and depression among 1,290 cancer patients. Patients had the option of three styles of massage: Swedish, light touch and foot massage. Findings revealed “Symptom scores declined in severity by approximately 50%. Swedish and light touch massage were found to be superior to foot massage.”
• Back pain — A number of studies also support the use of massage for back pain. Among them:
◦ A 2017 study reported that 49.4% of patients with persistent lower back pain who received 10 massage sessions over a 12-week period were clinically improved at 12 weeks, and of those, 75% were still clinically improved at 24 weeks.14
◦ A 2011 study15 concluded massage therapy (one hour of weekly sessions for 10 weeks) “may be effective for treatment of chronic back pain, with benefits lasting at least six months.” Both relaxation and structural massage were helpful, providing about the same amount of benefit.
◦ A 2016 study16 evaluating the effect of Thai massage on patients with upper back pain lasting at least three months found the treatment significantly decreased muscle tension and pain intensity at the end of the treatment session.
◦ A 2016 meta-analysis by the Cochrane Library looking at 25 trials, a majority of which were funded by nonprofit organizations, concluded massage was better than inactive controls for acute, sub-acute and chronic low back pain. When it came to function, massage was effective for sub-acute and chronic pain but not acute cases.
◦ A 2007 study17 found patients who had low back pain for at least six months who received 30-minute massages twice a week for five weeks reported less pain, depression, anxiety and sleep disturbance than controls who received relaxation therapy instead.
Frequency and Dosage Matter for Certain Types of Pain
Some people experience immense relief from massage, anecdotally speaking, while others do not. The difference might come down to the dose. Researchers from the Group Health Research Institute in Seattle looked into the optimal massage dose for people with chronic neck pain.18
Study participants received 30-minute massages two or three times a week, or 60-minute massages one, two or three times weekly. A control group received no massages.
Compared with the no-massage group, those who got massages three times a week were nearly five times more likely to report a significant improvement in function and more than twice as likely to report a significant decrease in pain.
The best pain-relief results were obtained by those who received 60-minute massages two or three times a week. It appears that longer massages worked best for neck pain, as did multiple treatments a week, especially during the first four weeks.
If you try massage therapy and find you’re not getting relief, you may want to try increasing the dose and frequency. There are other variables that impact massage effectiveness as well, such as the technique used and the skill level of the massage therapist.
When choosing a massage therapist, ask your holistic health care provider to recommend a certified massage therapist who is experienced in the type of pain relief you’re seeking.
Massage Therapy for Mental Health
Another area where massage therapy can be helpful is in the treatment of stress, anxiety and depression, including stress experienced by dementia patients. As mentioned, massage affects your nervous system through the nerve endings in your skin, which stimulates the release of “feel good” endorphins that help induce a sense of relaxation and well-being.
A 2015 study19 found Thai massage significantly reduces a stress marker called salivary alpha-amylase (sAA), suggesting it “may have a modest effect on stress reduction.” The American Massage Therapy Association also cites a number of studies20 showing massage helps ease stress, lowering heart rate, blood pressure21 and cortisol levels.
Studies22,23 looking at psychological states specifically have also demonstrated massage results in lower scores on the perceived stress scale, the POMS depression scale and the anxiety state scale.
A meta-analysis24 looking at massage therapy in depressed patients concluded “Massage therapy is significantly associated with alleviated depressive symptoms.” Similarly, a proof-of-concept randomized controlled study25 assessing the effects of Swedish massage on patients with generalized anxiety disorder found two weekly sessions for six weeks to be an effective treatment.
Massage May Help Quell Inflammation
The benefits of massage therapy for pain relief are established enough that it’s commonly used during physical therapy and rehabilitation from injury.
In one study,26 researchers took muscle biopsies from study participants who had received massage therapy or no treatment for exercise-induced muscle damage. According to the authors, massage therapy reduced inflammation and promoted mitochondrial biogenesis in the skeletal muscle.
The study is not without detractors,27 however, who have pointed out its flaws. Still, there’s reason to suspect that massage does have a beneficial impact on inflammation, as pain and inflammation tend to go hand in hand.28 By lowering one, you lower the other, and as discussed above, there’s plenty of evidence supporting the claim that massage can ease pain.
Other research29 from Cedars-Sinai Medical Center in Los Angeles, which I’ll discuss again further below, has also found Swedish massage decreased levels of several interleukins, which play a role in inflammation. According to the authors:
“Preliminary data suggest that a single session of Swedish Massage Therapy produces measurable biologic effects. If replicated, these findings may have implications for managing inflammatory and autoimmune conditions.”
Timing of Massage Therapy May Affect Pain Relief and Inflammation
Timing of treatment may be of the essence here. As noted by licensed massage therapist Amy Bradley Radford in an article in Massage Magazine:30
“If pain is a signal for inflammation to start, then you must limit how much pain you give someone in higher levels of inflammation, or you just feed the fire … There are two ways massage therapists can approach inflammation: directly and indirectly, and which way we choose depends on each client’s ability to heal …
Some clients’ bodies … can heal from pain well through deeper work, stretching or trigger-point therapy.Then there are others … in which that same treatment completely backfires, with the person having to go through days of pain and recovery after the treatment. What is the difference? … The answer is that Client B has more pain and inflammation …
This can present a difficult paradox for the therapist, as the client in more pain typically wants you to ‘work out those knots’ so that he can feel better … If a client has to recover from bodywork instead of feeling immediately better from that appointment, then whatever work was applied put her body into more pain and inflammation, and she did not have the energy to meet the new, additional demand created by the massage …
If your client comes in at a pain level of eight and after the session he is at a three, what does that tell you? That whatever treatment you offered actually gave energy back to the body by reducing pain and therefore inflammation. The energy to heal was offered and received.
This process has a basis in Chinese medicine, which seeks to balance the body by shifting energy, or chi. The important part is that pain decreased and energy demand went down, creating a surplus of energy to fight inflammation or to be given to the area in greatest need of healing.”
This appears to be sensible advice worth keeping in mind by patients and massage therapists alike. If your pain is worse immediately after your session, you may need either a lighter form of massage, or you may need to wait a bit before you get another treatment. As a general rule, the effects of massage therapy tend to be rather rapid, so if you feel pain relief at the end of the session, chances are your inflammation level has been positively impacted.
Massage Therapy Boosts Immune Function
Lymphatic massage31 is characterized by long, gentle, rhythmic strokes performed with light pressure to increase the flow of lymph through your body, thereby aiding the removal of toxins.
By increasing circulating lymphocytes, a form of white blood cells that are especially prevalent in the lymphatic system and fight off infections and disease, lymphatic massage also helps boost your immune function.
Research32 confirming this was published by scientists at Cedars-Sinai Medical Center in Los Angeles. According to the authors:
“Compared to light touch, Swedish Massage Therapy caused a large effect size decrease in AVP [arginine-vasopressin], and a small effect size decrease in CORT [cortisol] … Massage increased the number of circulating lymphocytes … Swedish Massage Therapy decreased IL-4, IL-5, IL-10, and IL-13 levels relative to baseline measures.”
As mentioned earlier, this study concluded that, if findings are able to be replicated, Swedish massage may turn out to be a valuable adjunct in the management of inflammatory and autoimmune conditions.
Two Additional Areas Where Massage Therapy Is Useful
Last but not least, two other areas where massage therapy is useful is in the treatment of spasms or cramps, and to improve flexibility. Injured and overworked muscles have a tendency to spasm and cramp, causing pain and discomfort.
Massage therapy, in this case neuromuscular massage, which involves deeper pressure, can help relax and soften these muscles to prevent spasms and cramping.33
Similarly, by easing stiff muscles and joints, massage therapy can help improve flexibility and range of motion.34 This may be especially beneficial for those who suffer from arthritis or muscle injuries. As noted in one systematic review and meta-analysis35 on the effectiveness of massage on the range of motion of the shoulder:
“Massage therapy is one of the complementary and alternative intervention for improving the functional status for patients who had impaired shoulder function in physical therapy clinics.
It relieves the muscle hardness by applying mechanical pressure on the affected area using the hands, and improves the range of motion of the joints.
In addition, it improves the excitability of the nerves in the muscle fiber and inhibits muscle pain. Massage therapy is also known to improve edema by promoting blood circulation within the muscle, and helps remove fatigue substances.”
_________________
Lyme/MSIDS patients would stick a needle in their eye if they thought it would help relieve their pain. Please consider massage therapy.





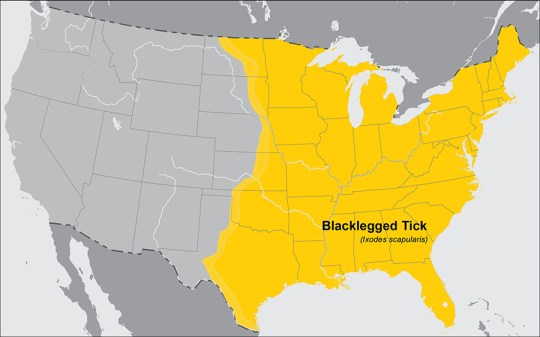


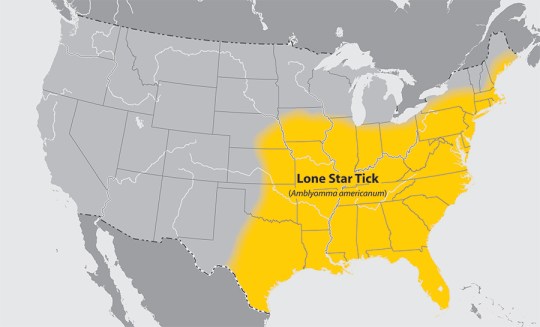
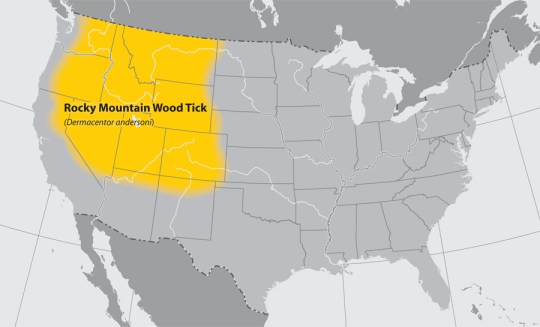
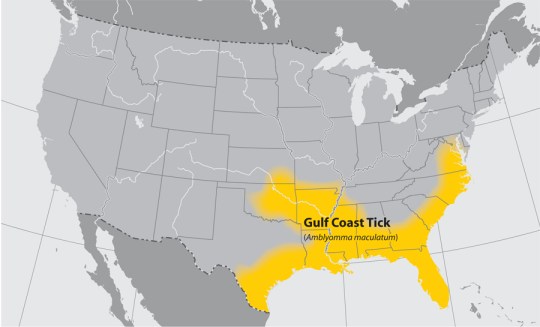
 Tick distribution maps found:
Tick distribution maps found: 
 James Lindsey at Ecology of Commanster, CC BY-SA 3.0, h
James Lindsey at Ecology of Commanster, CC BY-SA 3.0, h