Part 2. Anatomy of a serology test system: antigen selection, sensitivity and specificity
(This article continues from the one published at the end of November 2019)
Laboratory confirmation of Borrelia infection in the UK is based around the protocol laid down in 1995 by the Centres for Disease Control (CDC) in the US. The concept developed at this time was that a two-tier systems should be used, where the first-tier test should be a high sensitivity assay, such as an ELISA, followed by a more specific, but less sensitive, immunoblot. It would appear that in the UK, some of the regional hospital laboratories use the DiaSorin Liaison XL auto-analyser as a screening approach. If positive or equivocal, a further patient sample should be sent to the reference laboratory, where the first-tier assay is the C6 ELISA and the second tier is a microarray immunoblot assay (ViraChip from Viramed; Theel et al., 2018), a more robust version of the previous line blot system (itself a replacement for the Western blot.
It would appear that in effect, a three-tier system is operated to provide laboratory confirmation of Lyme disease in some regions of the UK. From the recent PHE meeting held in Liverpool on the 22nd November, an abstract was presented where analysis performed by the Bristol NHS Trust using the DiaSorin methodology, was compared to C6 ELISA results obtained by the RIPL at Porton Down. Out of 3131 tests performed at the Bristol laboratory, 296 samples tested positive for IgM antibodies to Borrelia and 195 tested positive for IgG antibodies.
As the first screening of samples was performed by the Bristol lab., one must assume that the -ve category (for Bristol) in the above table (reproduced from Albur et al., 2019) arrises as a result of the medical professional having enough clinical suspicion of Lyme disease for another blood sample to be tested at Porton Down.
By considering the positive tests in the table above, it would appear that the DiaSorin test is more sensitive for both IgM and IgG detection than the C6 (considerably more so for IgM than IgG). For samples from patients who previously had a negative test result in Bristol, half the samples are now positive with the C6 (74/149) for IgM, and 19.6% of samples that were originally negative at Bristol are now positive for IgG with the C6. These re-test results possibly provide evidence of seroconversion (the development of an antibody response to Borrelia), as the repeat sampling would have been performed at least two weeks after the first, giving more time for an antibody response to develop. This observation suggests that the difference between the two test systems is even more significant in terms of test sensitivity- a difference that favours of the DiaSorin test.
So what might explain the difference in sensitivity between the two test systems? In an attempt to answer this we must return to where we left off in Part 1, namely the effect of antigen selection on sensitivity and specificity.
As discussed in the previous article, as a methodology, serology for Lyme disease screening determines the presence of antibodies to proteins on the outside of the Borrelia microorganism. Antibody detection is achieved by selecting an appropriate antigenic protein (a protein that activates the immune system) on the surface of the microorganism. A traditional approach to find such antigens is to prepare a protein extract from the organism and then to run these proteins on a polyacrylamide gel and perform a Western blot. In this process, proteins from a gel are transferred to nitrocellulose paper (blotted) and the paper is exposed to patient sera. Once excess serum is washed away, a second enzyme-labelled antibody specific to human IgM or IgG is incubated with the paper and after washing off excess, a substrate for the enzyme is added that allows proteins recognised by antibodies in the patient serum to be identified. A typical example of a western blot is shown below.

The Western blot above is from the 1988 paper by Hansen et al. This paper describes the development of a Borrelia ELISA based around the p41 antigen. Proteins are often described by their molecular weight in kDaltons; p41 is flagellin, the major component of the Borrelia flagellum. The p41 protein is highly antigenic and the figure above shows that purified p41 strongly reacts to antibodies in serum from an individual with Lyme disease. Hansen and colleagues then tested how much p41 was needed in comparison to the crude protein extract to give the highest difference between a control serum and serum from a Lyme patient. Their original graph is shown below.

The y-axis shows colour development in the ELISA wells (see Part 1 for outline of ELISA design), whilst the x-axis is the dilution of both protein extract and the p41 protein. To establish the assay with p41 as antigen, a dilution of 3200 was used as this gave the highest differential between 1, values for a control serum and 4, values for serum from a Lyme patient. For the control serum of curve 2, it is clear that there is more non-specific binding with the crude protein extract from the Swedish strain of Borrelia burgdorferi.
This dilution of p41 was then used to coat plastic wells of multi-well plates and these plates were used to test serum from uninfected individuals (controls), from those with symptoms of Lyme disease and from individuals infected with other spirochaetes (that have flagella and thus may cross-react). A section from one of the original figures from the Hansen et al. paper is reproduced below.

In comparison to wells coated withe the total protein extract from Borrelia (left), for p41 as antigen, there is reasonably clear differentiation between controls and patient samples (LMR). Samples from Syphilis-infected individuals (SY1/2) show some cross-reactivity but much less so than for wells coated with the crude protein extract. These studies clearly demonstrate how the choice of antigen changes both sensitivity and specificity. The cut-off, or assay threshold for positivity has to be raised for the crude extract (horizontal line). Due to such a lack of specificity, sensitivity is lost, meaning that many more patients with symptoms of Lyme disease fall below the threshold for positivity.
Whilst p41 would appear to be ideal for fist-tier screening of suspected Lyme cases, the perception of wide ranging cross-reactivity to other organisms meant that throughout the 1990s other Borrelia antigens were considered in preference (the unfortunate dismissal of p41 as a screening antigen will be returned to in Part 3 of this article).
The search for antigens since the the mid 1980s has given rise to a spectrum of antigenic proteins for antibody detection. On the right is a list of proteins identified by Roger Evans and colleagues (2010) from a MedLine search for protein bands on Western blots. From the 1990s onwards, at least 20 companies have developed assay systems based on a number of these proteins.
Returning now to the issue of antigen choice and the difference between the two ‘first-tier’ screening systems used in the UK. The DiaSorin system for IgM detection uses two recombinant antigens, OspC, an outer surface protein that appears to show specificity for IgM detection in the early phase of infection, and the VlsE protein. For IgG, the DiaSorin test system uses a recombinant VlsE alone. In contrast, for both IgM and IgG detection, the C6 of Immumetics uses a short sequence of 25 amino acids corresponding to an invariant region in the protein.

This is not the only difference between the two systems. The DiaSorin LIAISON test uses a chemoluminescent assay format where the second antibody is labelled with a light-emitting probe (see diagram above taken from the paper of Cinquanta et al., 2017). Chemiluminescent immunoassays (CLIA) have the potential for analytical sensitivity many orders of magnitude greater than ELISA (Cinquanta et al., 2017). As described in Part 1 of this article, an increase in sensitivity will decrease the analytical detection limit for antibodies. For Borrelia antibody detection, a decrease in cut-off or working detection limit, will only be realized if by choice of the most appropriate antigen, specificity also increases (the figure concerning p41 detection above is an example of how antigen selection determines specificity, that in turn, determines the assay cut-off and hence clinical sensitivity).
Although both the DiaSorin and C6 tests use the VlsE antigen, DiaSorin use a full length recombinant protein whereas the C6 uses a 25 amino acid sequence of the VlsE protein (Liang et al., 1999). So it would appear that in the UK we have a screening assay for Borrelia that is rather different to the true first-tier test used in the reference laboratory at Porton Down.
From these data provide by the Bristol NHS trust (Table at beginning of this article) it would appear that the DiaSorin CLIA is more sensitive than the C6, especially so for IgM. With respect to further comparison of assay systems, a significant study was published last year by Pegalajar-Jurado et al. The CDC recommended two tier-test paradigm of ELISA, EIA (enzyme immunoassay) or CLIA before an immunoblot, was compared to a first-tier with an EIA or CLIA followed by a second tier with a similar type of assay. These algorithms are described in the figure below (taken from Pegalajar-Jurado et al., 2018).
This study used well characterised samples from the CDC (Molins et al., 2016) and made comparisons of several assay types including the DiaSorin CLIA and the C6 from Immumetics. Although complex, the major table from this study is reproduced in its entirety below.
Whilst the distinction between IgM and IgG positivity has not been made in the above table, it of high significance that particularly for Early Lyme disease with EM, the MTTT algorithm outperforms the STTT algorithm for all assay combinations. Also significant, is the inclusion of data from the DiaSorin VlsE/C6 combination showing no loss in specificity, as noted by the control samples tested.
Currently testing within some regions of the UK conforms to the VlsE/C6 algorithm with the exception that the DiaSorin CLIA for VlsE is performed several weeks before a repeat test with the C6 at the reference laboratory. Also, samples that are positive with the C6 in reference laboratory at Porton Down, are re-tested with the ViraChip system. This three-tier algorithm doesn’t fit into either the MTTT or the STTT paradigm.
So what can we conclude from all this?
Primarily, a review of the current serological testing paradigm for Lyme disease within the UK is urgently needed.
Although data provided by the Bristol NHS trust suggest that the DiaSorin CLIA in UK format is more sensitive than the C6, it is essential that further studies are conducted where the same serum samples are tested in both assay systems (DiaSorin CLIA and C6). Whilst data provided by Pegalajar-Jurado and colleagues (2018) suggest that the VlsE/C6 MTTT algorithm is more effective than the STTT algorithm for early laboratory diagnosis of Lyme disease, we cannot make the same assumption for a UK cohort of samples/patients. The same format of study as reported by Pegalajar-Jurado and colleagues must be conducted in the UK.
Also, it is not know whether all suspected cases of Lyme disease are tested within the local hospital trust and therefore give rise to a three-tier protocol (DiaSorin CLIA, followed some weeks later by a C6 and a Virotech Line blot). Unless it is experimentally investigated, it cannot be assumed that a three-tier protocol will give the same overall sensitivity as a two-tier protocol.
Centers for Disease Control and Prevention. (1995) Recommendations for test performance and interpretation from the Second National Conference on Serologic Diagnosis of Lyme Disease. MMWR Morb Mortal Wkly Rep 44:590 –591
Theel ES, Sorenson M, Grangera D. (2018) Evaluation of a Novel Microarray Immunoblot Assay for Detection of IgM- and IgG-Class Antibodies to Borrelia burgdorferi. J. Clin. Microbiol 56 (11) e00992-18
Albur M, Hamilton F, MacGregor K (2019) Serodiagnosis of Lyme disease: Cheese and Chalk or Peas in a Pod? Lyme and tick-born disease research in the UK. PHE conference. Liverpool, 21-22nd November 2019
Hansen K, Hindersson P, Pedersen NS (1988) Measurement of Antibodies to the Borrelia burgdorferi Flagellum Improves Serodiagnosis in Lyme Disease. J Clin Microbiol. 26 (2): 338-346
Evans R, Mavin S, McDonagh S, Chatterton JM, Milner R, Ho-Yen DO. (2010) More specific bands in the IgG western blot in sera from Scottish patients with suspected Lyme borreliosis. J. Clinical Pathol. Doi:10.1136/jcp.2010.076307
Cinquanta L, Fontana DE, Bizzaro N (2017) Chemiluminescent immunoassay technology: what does it change in autoantibody detection? Autoimmun Highlights 8:9 https://doi.org/10.1007/s13317-017-0097-2
Liang FT, Alvarez AL, Gu Y, Nowling JM, Ramamoorthy R, Philipp MT (1999) An Immunodominant Conserved Region Within the Variable Domain of VlsE, the Variable Surface Antigen of Borrelia burgdorferi. J Immunol November 163 (10) 5566-5573
Pegalajar-Jurado A, Schriefer ME, Welch RJ, Couturier MR, MacKenzie T, Clark RJ, Ashton LV, Delorey MJ, C Molinsa CR. (2018) Evaluation of Modified Two-Tiered Testing Algorithms for Lyme Disease Laboratory Diagnosis Using Well-Characterized Serum Samples. Journal of Clinical Microbiology 56 (8) e01943-17
Molins CR, Delorey MJ, Sexton C, Schriefer ME. (2016). Lyme borreliosis serology: performance with several commonly used laboratory diagnostic tests and a large resource panel of well-characterized patient samples. J Clin Microbiol 54:2726–2734. https://doi.org/10.1128/JCM .00874-16
Branda JA, Strle K, Nigrovic LE, Lantos PM, Lepore TJ, Damle NS, Ferraro MJ, Steere AC. 2017. Evaluation of modified 2-tiered serodiagnostic testing algorithms for early Lyme disease. Clin Infect Dis 64:1074–1080. https://doi.org/10.1093/cid/cix043.
_________________
Go here for part 1: https://www.linkedin.com/pulse/borrelia-detection-lyme-disease-chris-newton/











 want to know if it’s still active through blood work. Or, if you have a mysterious chronic disease that might be caused by Lyme-Borreliosis and/or its co-infections, the blood work could tell you if your illness is due to Lyme disease. Right?
want to know if it’s still active through blood work. Or, if you have a mysterious chronic disease that might be caused by Lyme-Borreliosis and/or its co-infections, the blood work could tell you if your illness is due to Lyme disease. Right? different people but a weaker positive may have different interpretations. This is one reason it is recommended to use a Lyme-literate lab such as Igenex.
different people but a weaker positive may have different interpretations. This is one reason it is recommended to use a Lyme-literate lab such as Igenex. 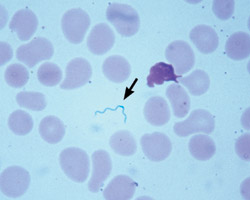 6. Borrelia exists sparsely in the blood. This is the reason it is difficult to test for it directly and an antibody panel is used. PCR tests look for DNA directly in the blood but only detect a small number of cases.
6. Borrelia exists sparsely in the blood. This is the reason it is difficult to test for it directly and an antibody panel is used. PCR tests look for DNA directly in the blood but only detect a small number of cases.
 There are times when it becomes impossible to determine whether someone’s health problems are due to Lyme-borreliosis infection or not.
There are times when it becomes impossible to determine whether someone’s health problems are due to Lyme-borreliosis infection or not.