8 Reasons Why The Standard Western Blot Is A Poor Diagnostic Indicator of Lyme – and tips for making sense of your lab result
This post was inspired by one of my practitioner-students who is in the process of both healing her own Lyme disease and co-infections, and learning how to be the best resource and guide for her own patients.
It is confusing for everyone, including health professionals, that the diagnostic testing for Lyme disease is so poor, and often meaningless.
If you’ve had a tick bite you might be wondering if you contracted Lyme and want to take the blood test to see if infection shows up. If you’ve had Lyme in the past and been treated, but still have remaining health issues, you may  want to know if it’s still active through blood work. Or, if you have a mysterious chronic disease that might be caused by Lyme-Borreliosis and/or its co-infections, the blood work could tell you if your illness is due to Lyme disease. Right?
want to know if it’s still active through blood work. Or, if you have a mysterious chronic disease that might be caused by Lyme-Borreliosis and/or its co-infections, the blood work could tell you if your illness is due to Lyme disease. Right?
It’s vitally important to know what the CDC’s standard Western Blot test for Lyme is good for, and what it is not. Unfortunately, it’s not good for much, but there are some key indicators that can be useful.
First, here are 8 reasons why it is such a poor diagnostic tool:
1. Poor test sensitivity. The CDC standard western blot (SWB) is not as sensitive as blots done by companies that specialize in testing tick borne disease, such as Igenex, and misses approximately 50% of cases (statistics vary, but it’s a lot!). False negative are common, often moreso in people who are very sick. Blots performed by Lyme specialty labs are more sensitive, however there are still a percentage of false negatives, especially in the late stages of the disease.
2. Diagnostic criteria. Even if a patient tests positive for a highly specific Borrelia band (bands 18, 23, 31, 34, 37, 39, 83 and 94) indicating exposure, a test will still be considered negative.
The CDC created a high standard for medical reporting of Lyme disease cases for tracking and statistical use that requires at least 2 bands of IgM or at least 5 bands of IgG to qualify for a positive result. Their standard was not intended to become doctor’s diagnostic guideline, yet it was adopted by the Infectious Disease Society of America’s (IDSA’s) guideline and has been.
3. Interpretation of the test is subjective. A test result depends on the skill of the technician who reads it. Different people can come up with different results. A strong positive on a band will likely be read the same by  different people but a weaker positive may have different interpretations. This is one reason it is recommended to use a Lyme-literate lab such as Igenex.
different people but a weaker positive may have different interpretations. This is one reason it is recommended to use a Lyme-literate lab such as Igenex.
4. All antibody bands are not created equal! SWB surveillance for IgG includes 5 that are non-specific to Borrelia, and several that could only be attributed to Borrelia (and it excludes 3 others that are Borrelia specific). There is definitely room for improving the standard lab test for Lyme disease, simply by using more of the Borrelia-specific bands. Igenex testing includes two more Borrelia specific bands than the SWB.
5. Different antibody bands may become positive during different stages of the infection. It is common that the first antibodies to appear is for band 41, yet it is non-specific and would be called “negative”. Weeks, months or years later, if re-tested, different antibodies (bands) may appear, and there may be more or fewer bands that show up.
This depends on many factors, including the stage of disease, the health or decline of the immune system, what treatments you have received, and more.
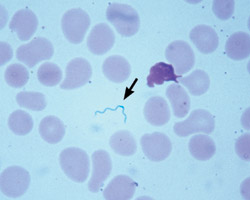 6. Borrelia exists sparsely in the blood. This is the reason it is difficult to test for it directly and an antibody panel is used. PCR tests look for DNA directly in the blood but only detect a small number of cases.
6. Borrelia exists sparsely in the blood. This is the reason it is difficult to test for it directly and an antibody panel is used. PCR tests look for DNA directly in the blood but only detect a small number of cases.
Yet an antibody test only works well when the microbe is visible to the immune system, and can generate antibodies against it. Lyme-borreliosis and the other stealth co-infections have numerous survival techniques of immune system evasion, including techniques for cloaking themselves and disrupting the body’s natural immune system response.
7. Failure to generate antibodies. An antibody test also only works if a person’s immune system is strong enough to generate an antibody response. Late stage patients or immune compromised patients may not mount an appropriate antibody response.
8. Species Variation. There are 5 known subspecies, and over 100 strains of Borrelia in the US and 300 worldwide (source: http://www.ILADS.org), yet the SWB only tests bands for 1 subspecies of Borrelia burgdorferi; specialized testing labs such as IGENEX test for only two. Ideally, the testing would be region-specific.
That was a lot of information to take in, so here are 3 main points to take away, to help you self-advocate and navigate the Lyme diagnosis maze:
- If you are dealing with an acute case of Lyme disease or a recent bite, know that any Lyme test given before 6 weeks out is not likely to be accurate, since it takes that long for your body to generate the antibodies to the bands that the Western Blot tests for.

- I didn’t waste any time discussing the ELISA test for Lyme disease in this article – and don’t waste any of your time with this lab! For numerous reasons, it is even less accurate than the Western Blot for detecting Lyme-Borreliosis.
- If your Lyme Western Blot came back negative, and you are a little or a lot sick, it is meaningless. You may very well still have Lyme disease. Try 6-8 weeks of a natural antimicrobial protocol, and re-test. You will be more likely to show antibodies at this time (but it’s not a guarantee).
- Always ask for a copy of your blood work, and look at the test results yourself. If you have one of the Lyme Borreliosis-specific bands that are positive (again, that’s bands 18, 23, 31, 34, 37, 39, 83 and 94) – even just 1! – even though the CDC (and therefore most doctors) would call it negative, this is a clear positive diagnostic indicator of Lyme disease.
- Keep in mind that what you’re suffering from could be a different stealth pathogen, such as Babesia or Bartonella, which require a different lab test, and are also notoriously difficult to detect.
 There are times when it becomes impossible to determine whether someone’s health problems are due to Lyme-borreliosis infection or not.
There are times when it becomes impossible to determine whether someone’s health problems are due to Lyme-borreliosis infection or not.
The good news is, from the holistic medical perspective you can still recover your health and your life through treatment that is based on your symptom presentation and the restoration of your energy, immunity and vitality – regardless of whether you ever determine the cause. The question then becomes, do you want a diagnosis, OR DO YOU WANT TO GET BETTER?
If you are confused about whether or not you have Lyme, a co-infection, or other complex chronic disease, call us at 845-687-6211 or email info@uprootinglyme.com to set up an in-person or virtual holistic Lyme consultation at reasonable rates. We’ll help you interpret your labs and co-create a strategic holistic treatment plan. Navigating Lyme disease is confusing, and confusion can cost you time and money that could be spent on getting the treatment you need. Contact us now!
____________________
**Comment**
Great article with many valid points. CDC 2-tiered testing is virtually worthless and the required arbitrary and stringent antibody levels are asinine. For a quote on this:
“setting arbitrary level of antibodies to diagnose a disease that has not been amenable to Koch’s postulates seems open to question. By the same token, ignoring antibody results unless they meet arbitrary levels seems suspect. The vast majority of patients in this series showed some WB antibody exposure, but many did not meet the arbitrary limits set….in our present state of knowledge, the diagnosis of chronic Lyme disease is a clinical one. Many of the patients in this series have suffered serious ‘hurts’ when they have been told that they could not have LD because their WB did not meet arbitrary limits.” Dr. Waisbren https://madisonarealymesupportgroup.com/2017/07/09/idsa-founder-used-potent-iv-antibiotics-for-chronic-lyme/
I’ve been in discussion with a PhD who is researching Lyme testing. He feels, as do I, that testing should initially cast a wide net with follow up testing being more specific; however, just the opposite is true with current testing. He also questions the CDC insistence that p41 is too non-specific to use.
According to microbiologist Tom Greer p41 is the flagellin protein of all spirochetes and is usually the first to appear after a Bb infection. Western Blot explained by Grier
For another great read on testing: https://madisonarealymesupportgroup.com/2018/09/12/lyme-testing-problems-solutions/
Please remember that this testing is ONLY for Lyme disease and will NOT pick up coinfections. The tests for those, as stated in this article, are just as abysmal.
A trained Lyme literate doctor is experienced in understanding the symptoms of all of these pathogens and will diagnose you clinically. They understand the limitations of testing. The Horowitz questionnaire has been validated and is a much better indicator of infection: https://madisonarealymesupportgroup.com/wp-content/uploads/2016/01/symptomlist.pdf If you suspect you are infected, print this out, fill it out, and take it with you to your first appointment. Avoid mainstream medicine if at all possible as they are truly in the dark ages with all things tick-borne.
