Study Shows Diminished Pathogen-specific Antibody Production in Coinfected Mice Contributing to Persistent Infection
https://www.ncbi.nlm.nih.gov/pubmed/30619263
Age-Related Differential Stimulation of Immune Response by Babesia microti and Borrelia burgdorferi During Acute Phase of Infection Affects Disease Severity.
Abstract
Lyme disease is the most prominent tick-borne disease with 300,000 cases estimated by CDC every year while ~2,000 cases of babesiosis occur per year in the United States. Simultaneous infection with Babesia microti and Borrelia burgdorferi are now the most common tick-transmitted coinfections in the U.S.A., and they are a serious health problem because coinfected patients show more intense and persisting disease symptoms. B. burgdorferi is an extracellular spirochete responsible for systemic Lyme disease while B. microti is a protozoan that infects erythrocytes and causes babesiosis. Immune status and spleen health are important for resolution of babesiosis, which is more severe and even fatal in the elderly and splenectomized patients.
Therefore, we investigated the effect of each pathogen on host immune response and consequently on severity of disease manifestations in both young, and 30 weeks old C3H mice.
At the acute stage of infection, Th1 polarization in young mice spleen was associated with increased IFN-γ and TNF-α producing T cells and a high Tregs/Th17 ratio. Together, these changes could help in the resolution of both infections in young mice and also prevent fatality by B. microti infection as observed with WA-1 strain of Babesia. In older mature mice, Th2 polarization at acute phase of B. burgdorferi infection could play a more effective role in preventing Lyme disease symptoms. As a result, enhanced B. burgdorferi survival and increased tissue colonization results in severe Lyme arthritis only in young coinfected mice. At 3 weeks post-infection, diminished pathogen-specific antibody production in coinfected young, but not older mice, as compared to mice infected with each pathogen individually may also contribute to increased inflammation observed due to B. burgdorferi infection, thus causing persistent Lyme disease observed in coinfected mice and reported in patients.
Thus, higher combined proinflammatory response to B. burgdorferi due to Th1 and Th17 cells likely reduced B. microti parasitemia significantly only in young mice later in infection, while the presence of B. microti reduced humoral immunity later in infection and enhanced tissue colonization by Lyme spirochetes in these mice even at the acute stage, thereby increasing inflammatory arthritis.
Key Quote: “Our findings recognize that microbial infections in patients suffering from TBDs do not follow the one microbe, one disease Germ Theory as 65% of the TBD patients produce immune responses to various microbes.”
Another problem:
83% of all commercial tests focus only on Lyme (borrelia), despite the fact we are infected with more than one microbe.
https://madisonarealymesupportgroup.com/2018/11/17/investigating-disease-severity-in-an-animal-model-of-concurrent-babesiosis-lyme-disease/ These findings suggest that B. Burgdorferi coinfection attenuates parasite growth while B. Microti presence exacerbates Lyme Disease-like symptoms in mice.
https://madisonarealymesupportgroup.com/2017/05/01/co-infection-of-ticks-the-rule-rather-than-the-exception/ Our study reveals high pathogen co-infection rates in ticks, raising questions about possible co-transmission of these agents to humans or animals, and their consequences to human and animal health. We also demonstrated high prevalence rates of symbionts co-existing with pathogens, opening new avenues of enquiry regarding their effects on pathogen transmission and vector competence.
https://madisonarealymesupportgroup.com/2018/10/11/babesia-found-in-patient-with-persistent-symptoms-following-lyme-treatment/ Because the Ixodes scapularis tick can harbour and transmit multiple parasites simultaneously, the possibility of coinfection should be considered in any patient not responding to appropriate initial medical therapy.
To date, ticks can transmit 18 and counting pathogens – ALL as devastating as Lyme: https://madisonarealymesupportgroup.com/2017/07/01/one-tick-bite-could-put-you-at-risk-for-at-least-6-different-diseases/
https://madisonarealymesupportgroup.com/2017/10/28/lyme-wars-part-5-coinfections/ (Click on NBC link for new story. Approx 5 Min.) All tests came back negative. Don’t be fooled. This stuff ISN’T RARE! Dr. Phillips discusses how Bartonella isn’t even on the radar and is often confused with Lyme as symptoms overlap greatly.


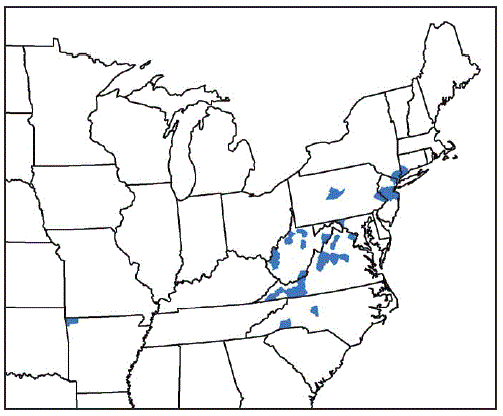 * Benton County, Arkansas; Fairfield County, Connecticut; Washington County, Maryland; Bergen, Hunterdon, Mercer, Middlesex, Monmouth, Somerset, and Union Counties, New Jersey; Davidson, Polk, and Rutherford Counties, North Carolina; Richmond, Rockland, and Westchester Counties, New York; Bucks and Centre Counties, Pennsylvania; Albemarle, Augusta, Carroll, Fairfax, Giles, Grayson, Louisa, Page, Pulaski, Rockbridge, Russell, Scott, Smyth, Staunton City, Warren, and Wythe Counties, Virginia; Cabell, Hardy, Lincoln, Mason, Marion, Monroe, Putnam, Ritchie, Taylor, Tyler, Upshur Counties, West Virginia.
* Benton County, Arkansas; Fairfield County, Connecticut; Washington County, Maryland; Bergen, Hunterdon, Mercer, Middlesex, Monmouth, Somerset, and Union Counties, New Jersey; Davidson, Polk, and Rutherford Counties, North Carolina; Richmond, Rockland, and Westchester Counties, New York; Bucks and Centre Counties, Pennsylvania; Albemarle, Augusta, Carroll, Fairfax, Giles, Grayson, Louisa, Page, Pulaski, Rockbridge, Russell, Scott, Smyth, Staunton City, Warren, and Wythe Counties, Virginia; Cabell, Hardy, Lincoln, Mason, Marion, Monroe, Putnam, Ritchie, Taylor, Tyler, Upshur Counties, West Virginia.