https://www.lymedisease.org/how-to-lift-brain-fog-and-boost-your-immune-system/
How to lift brain fog and boost your immune system
2/9/23
By Lonnie Marcum

Both viruses and bacteria can invade the brain. All too frequently, patients with lingering symptoms following infection complain of “brain fog.”
Brain fog describes the feeling of mental confusion, forgetfulness, memory loss, lack of motivation, inability to focus, and/or difficulty concentrating.
A simple technique known as lymphatic drainage massage may help to clear the fog and boost your immune system at the same time.
Patients with brain fog often report “drawing a blank” when trying to remember the name of a friend, family member or pet; forgetting what they were going to do; or getting lost on the way home or to a familiar location. Brain fog can also be associated with symptoms of anxiety and/or depression.
Prolonged brain fog can be caused by a variety of factors, including sleep disturbance, certain medications, head injury, environmental toxins, inflammation and infection—which is the case in many individuals with “Lyme brain.”
Borrelia burgdorferi (Bb), the bacteria that causes Lyme disease, can infect the brain and nervous system. Neurological symptoms of Lyme disease are a late-stage manifestation of Bb infection called neuroborreliosis.
Neuroborreliosis and Lyme Brain
In 2011, researchers at the University of California, Davis were able to show how Bb invades the lymph nodes within 24 hours after infection. They later discovered how it causes abnormalities in the lymph tissues and impairs the immune system.
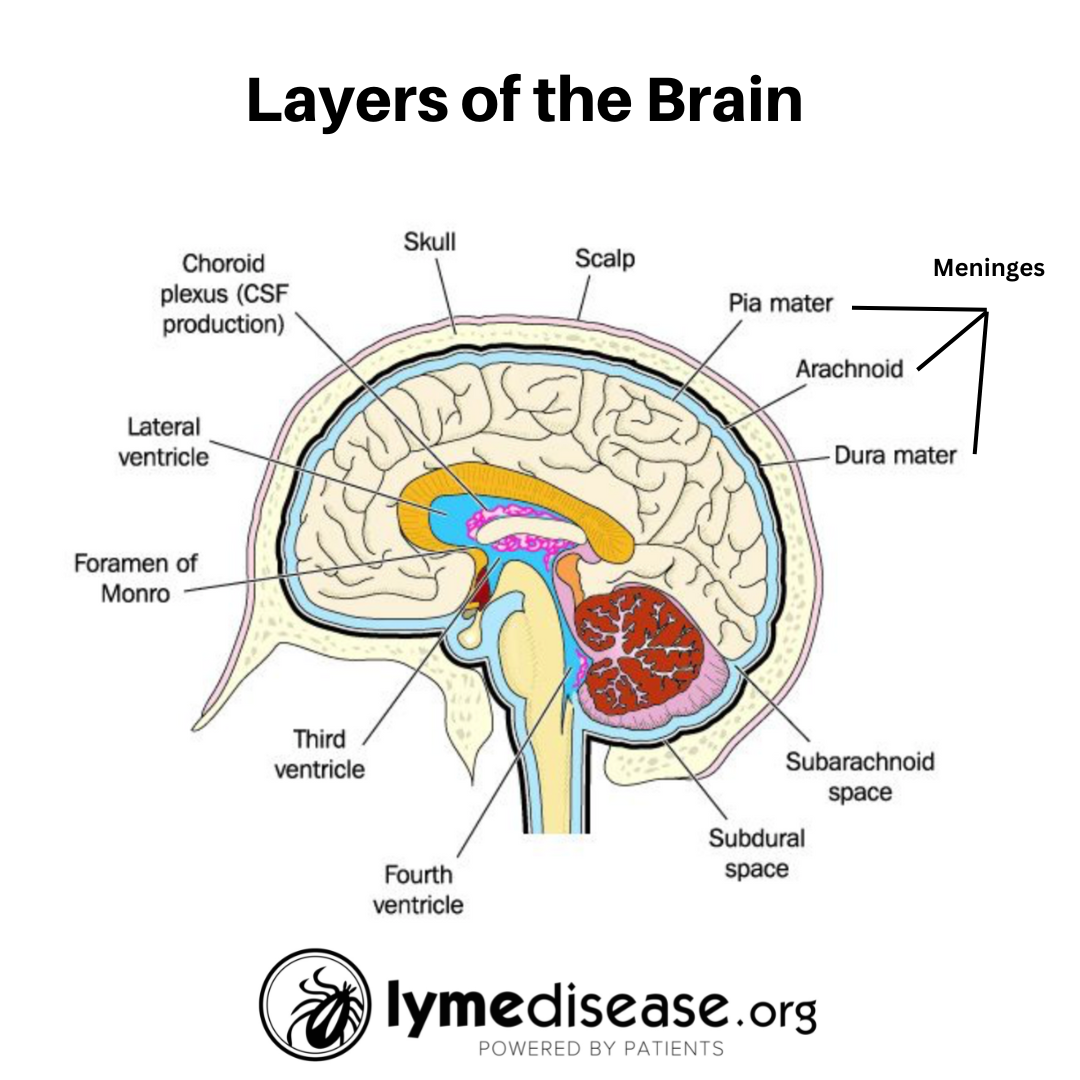
A more recent study suggests that the choroid plexus may play a role in how Borrelia infections affect the nervous system. The choroid plexus is found within the ventricles near the center of the brain. It produces and filters cerebrospinal fluid (CSF), the clear fluid that circulates around the brain and spinal cord.
Another important study from Tulane University found spirochetes that cause Lyme disease in the autopsied brain tissue of a patient who had been aggressively treated with antibiotics. This demonstrated that infection can persist despite antibiotic treatment.
Even if the Borrelia spirochetes don’t completely penetrate the brain, they are frequently present in the meninges. These are three protective layers surrounding the brain and spinal cord. Infection of the meninges is associated with increases in inflammatory cytokines, and meningitis, a swelling of the meninges.
Lyme disease is the most common vector-borne disease in the U.S. and Europe. The spread of Bb to the central nervous system causing Lyme neuroborreliosis occurs in approximately 10–15% of all cases of Lyme disease. In the U.S., one of the most frequent manifestations of Lyme neuroborreliosis is lymphocytic meningitis.
Lyme lymphocytic meningitis is swelling of the meninges with the infiltration of lymphocytes (a type of white blood cell) into the CSF. Symptoms may include fever, headache, neck pain/stiffness, sensitivity to light and cognitive impairment.
Two Circulatory Systems
There are two circulatory systems in our bodies: the cardiovascular system and the lymphatic system.
The cardiovascular system consists of the heart and blood vessels (arteries, veins, capillaries). Basically, arteries carry oxygenated blood and nutrients away from the heart to every tissue in the body, while veins carry used blood back to the heart and lungs in a continuous loop. Capillaries are the small vessels where the arteries and veins connect.
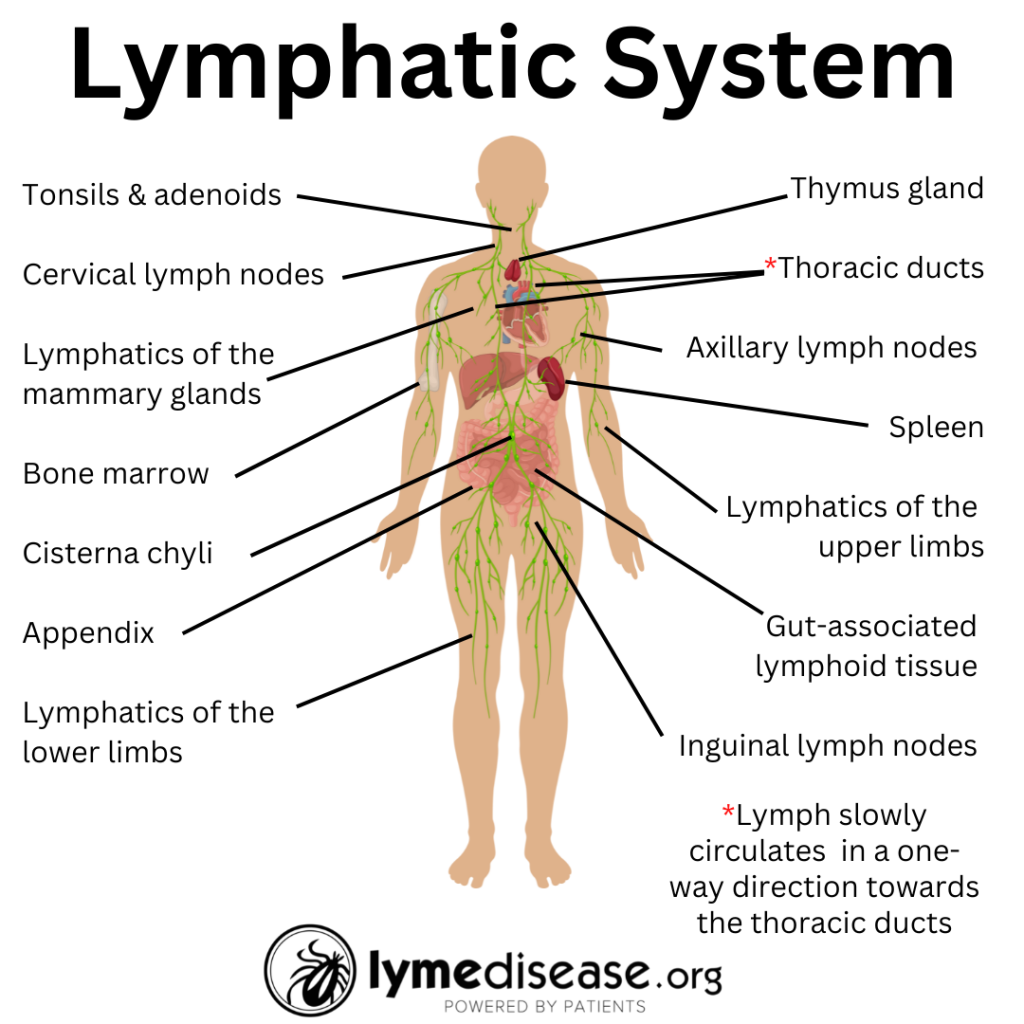
The lymphatic system is a secondary circulatory system. It works separately but in conjunction with the cardiovascular system. When working properly, lymphatics only move in one direction—towards the heart. Included in the lymphatic system are small bean-shaped structures called lymph nodes. Depending on one’s age and sex, there are 400-700 lymph nodes throughout the body with main clusters found in the neck, armpits, chest, abdomen and groin.
Lymph nodes contain life-saving immune cells including:
- T-cells (T-lymphocytes) – play a crucial role in cell-mediated immunity;
- B-cells (B-lymphocytes) – produce antibodies that help fight pathogens;
- Dendritic cells – present antigens to T-cells, activating the immune system;
- Macrophages – engulf and digest foreign matter, cellular debris, and pathogens;
- Natural killer cells – attack abnormal (cancerous) or infected cells;
- Plasma cells – produce and secrete antibodies.
As bacteria and viruses enter the lymph nodes, the immune cells work to identify and remove them. The more fluid that moves through the lymph nodes, the more immune cells will be produced. From there, the waste is filtered out through the liver and kidneys and the lymph is returned to the blood stream in a continuous cycle.
Unlike the cardiovascular system, which is powered by the heart, the lymphatic system lacks a central pump. Thus, it relies on muscle contractions to circulate lymph. To keep lymph moving through the system, you must drink plenty of water and be active enough to move the fluids through the body.
However, many patients with persistent symptoms of Lyme suffer from chronic fatigue, making activity and traditional exercise nearly impossible—which was the case with my daughter.
When my daughter was immobile due to chronic illness, I used three things to help with lymph drainage: passive range of motion exercises, medical grade compression stockings, and manual lymph drainage massage. These were all things I’d been taught as a physical therapist (PT).
Later we worked with a PT who specialized in chronic fatigue syndrome. She helped my daughter design a full body lymph drainage massage technique she continues to use to this day.
[Note: While you can learn to do all these things on your own, I highly recommend scheduling an appointment with a licensed physical therapist to learn the proper technique for each. PT is covered by most insurance.]
Lymphatic drainage for brain health
There is increasing evidence that infection is a risk factor for neurodegenerative diseases. In fact, one of the most common viral infections, Epstein-Barr virus, is now linked to multiple sclerosis.
Whether an infection is active, persistent, dormant, or the dead remnants of previous illness, it can produce inflammatory waste products that the body must try to clear through the circulatory system.
Lymphatic drainage massage is a therapeutic technique that uses gentle, rhythmic strokes to stimulate the flow of lymph fluids in a specific direction through the body.
Whole body lymph drainage massage helps reduce inflammation and remove waste products. It also helps stimulate the immune system and allows the movement of basic hormones needed for rest and healing.
Lymphatic drainage massage is similar to deep cleaning your home. It’s like clearing the cobwebs out of the corners and the dust bunnies out from under the bed. When the lymph nodes are plugged, they slow the flow of lymphatic fluid. Leaving those nodes clogged and swollen impairs the healing process.
Never underestimate the value of keeping the lymphatic system functioning.
The Glymphatic System
In the brain, the lymphatic clearance pathway is called the glymphatic system—a pathway that was only recently discovered.
Maiken Nedergaard is a Danish neuroscientist who works at the University of Rochester Medical Center in New York. In 2012, she first identified the existence of the network of lymphatic vessels in the brain that eliminate toxins via cerebrospinal fluid. Prior to this, no one knew how the brain cleared waste and infections. Nedergaard created the word “glymphatic” to represent the relationship between the glial cells and the lymphatic system of the brain.
Nedergaard discovered that the glymphatic system is responsible for removing byproducts of infection, including amyloid beta. It’s a protein that can build up in the brain and is associated with the onset of Alzheimer’s disease.
The glymphatic system is most active during uninterrupted deep sleep. This is one reason why sleep is so important for overall brain health and why sleep deprivation can exacerbate neurodegenerative diseases.
Head/Neck Lymphatic Self-Massage
[Note: If you have any contraindications listed below, please speak to your doctor before performing this procedure.]
When doing lymphatic drainage massage, you always want to start by opening the lymph valves closest to the heart first, work your way outwards, then back in towards the heart. The first time you do this type of massage I recommend going low and slow — maybe 10 – 20 motions of each of the following steps. Later, if no adverse reactions, you can increase to 50 repetitions of each step.
Step 1. From a comfortable seated position, begin by gently pulsing the lymphatic nodes at the base of your neck, the soft space just above the collarbones. These nodes need to be opened before anything can move down from the head/neck.
Step 2. Move your fingers higher up the neck to the groove just behind your ears. With palms flat, pull the skin gently towards the front and all the way down to the center of your neck where it meets the “V” between the collarbones. (P.S. If your sinuses and/or ears pop and you feel like swallowing, you are doing it right.)
Step 3. Make the “Spock” hand sign. Place your middle and index finger behind the ears and the ring and pinky finger in front of the ears and gently pull downwards.
Step 4. Move your hands around the back of the head/neck to the base of the skull and gently pull forward.
Step 5, 6, and 7 is the first three steps in reverse: Perform steps 3, 2 and 1, pulling all the fluid down towards the collarbones.
This is the video I most frequently use to teach people this simple beginner’s self-drainage massage technique.
Watch:
Other Treatments
- An anti-inflammatory diet, full of high quality proteins, fresh fruits/veggies and fiber, and low in processed foods, sugar, gluten and dairy.
- Vitamin B, vitamin C and vitamin D are also vital to immune health,
- Certain herbs as recommended by Dr. Bill Rawls,
- Epsom salt baths or foot soak. The magnesium helps to calm the nerves
- Saunas and dry brushing also help with lymphatic drainage,
- Movement based upon your tolerance: simple range of motion (moving arms & legs while lying or seated), walking, yoga, swimming, or biking.
- Vagus nerve stimulation regulates the immune system through its connections with immune cells in the spleen, thymus and gut-associated lymphoid tissue (GALT),
- Abdominal massage to help get things moving,
- Other integrative and restorative therapies.
Contraindications
I always recommend speaking to your treating clinician before beginning a new treatment method. Contraindications to lymphatic massage include acute infection, cardiac edema, cancer, blood clots (DVT), bleeding conditions, kidney failure, bronchitis, uncontrolled high blood pressure.
Resources
Find a Lymphology Certified Specialist through LANA.
Training: Manual Lymph Drainage Institute International
Self-help: The Concise Perrin Technique: A Handbook for Patients. By Dr. Raymond Perrin. (A practical companion to The Perrin Technique 2E: How to diagnose and treat CFS/ME and fibromyalgia via the lymphatic drainage of the brain.)
LymeSci is written by Lonnie Marcum, a Licensed Physical Therapist and mother of a daughter with Lyme. She served two terms on a subcommittee of the federal Tick-Borne Disease Working Group. Follow her on Twitter: @LonnieRhea Email her at: lmarcum@lymedisease.org.
References
Adams Y, Clausen AS, Jensen PØ, Lager M, Wilhelmsson P, Henningson AJ, Lindgren PE, Faurholt-Jepsen D, Mens H, Kraiczy P, Kragh KN, Bjarnsholt T, Kjaer A, Lebech AM, Jensen AR. 3D blood-brain barrier-organoids as a model for Lyme neuroborreliosis highlighting genospecies dependent organotropism. iScience. 2022 Dec 19;26(1):105838. doi: 10.1016/j.isci.2022.105838. PMID: 36686395; PMCID: PMC9851883.
Bacyinski A, Xu M, Wang W, Hu J. The Paravascular Pathway for Brain Waste Clearance: Current Understanding, Significance and Controversy. Front Neuroanat. 2017 Nov 7;11:101. doi: 10.3389/fnana.2017.00101. PMID: 29163074; PMCID: PMC5681909.
Bohr T, Hjorth PG, Holst SC, Hrabětová S, Kiviniemi V, Lilius T, Lundgaard I, Mardal KA, Martens EA, Mori Y, Nägerl UV, Nicholson C, Tannenbaum A, Thomas JH, Tithof J, Benveniste H, Iliff JJ, Kelley DH, Nedergaard M. The glymphatic system: Current understanding and modeling. iScience. 2022 Aug 20;25(9):104987. doi: 10.1016/j.isci.2022.104987. PMID: 36093063; PMCID: PMC9460186.
Chikly, Bruno (2004). Silent Waves: Theory and Practice of Lymph Drainage Therapy: An Osteopathic Lympathic Technique. I.H.H. Pub. ISBN 978-0-9700-5302-2.
Chikly BJ. Manual techniques addressing the lymphatic system: origins and development. J Am Osteopath Assoc. 2005 Oct;105(10):457-64. PMID: 16314678.
Elsner RA, Hastey CJ, Olsen KJ, Baumgarth N (2015) Suppression of Long-Lived Humoral Immunity Following Borrelia burgdorferi Infection. PLoS Pathog 11(7): e1004976. doi:10.1371/ journal.ppat.1004976
H Heald A, Perrin R, Walther A, Stedman M, Hann M, Mukherjee A, Riste L. Reducing fatigue-related symptoms in Long COVID-19: a preliminary report of a lymphatic drainage intervention. Cardiovasc Endocrinol Metab. 2022 Apr 12;11(2):e0261. doi: 10.1097/XCE.0000000000000261. PMID: 35441129; PMCID: PMC9010124.
Lotz SK, Blackhurst BM, Reagin KL, Funk KE. Microbial Infections Are a Risk Factor for Neurodegenerative Diseases. Front Cell Neurosci. 2021 Jul 7;15:691136. doi: 10.3389/fncel.2021.691136. PMID: 34305533; PMCID: PMC8292681.
Parthasarathy G, Pattison MB, Midkiff CC. The FGF/FGFR system in the microglial neuroinflammation with Borrelia burgdorferi: likely intersectionality with other neurological conditions. J Neuroinflammation. 2023 Jan 17;20(1):10. doi: 10.1186/s12974-022-02681-x. PMID: 36650549; PMCID: PMC9847051.
Sachdeva S, Persaud S, Patel M, Popard P, Colverson A, Doré S. Effects of Sound Interventions on the Permeability of the Blood–Brain Barrier and Meningeal Lymphatic Clearance. Brain Sciences. 2022; 12(6):742. https://doi.org/10.3390/brainsci12060742
Thompson D, Brissette CA, Watt JA. The choroid plexus and its role in the pathogenesis of neurological infections. Fluids Barriers CNS. 2022 Sep 10;19(1):75. doi: 10.1186/s12987-022-00372-6. PMID: 36088417; PMCID: PMC9463972.
Tunev SS, Hastey CJ, Hodzic E, Feng S, Barthold SW, Baumgarth N. Lymphoadenopathy during lyme borreliosis is caused by spirochete migration-induced specific B cell activation. PLoS Pathog. 2011 May;7(5):e1002066. doi: 10.1371/journal.ppat.1002066. Epub 2011 May 26. PMID: 21637808; PMCID: PMC3102705.