https://www.lymedisease.org/lyme-sci-dont-assume-your-symptoms-mean-covid-could-be-lyme-disease/
LYME SCI: Don’t assume your symptoms mean COVID. Could be Lyme disease.
April 5, 2021
By Lonnie Marcum

As the COVID-19 pandemic continues, there are reports of some unintended consequences, including delayed or missed diagnosis of Lyme disease.
The initial symptoms of Lyme disease can be very similar to COVID-19, with generalized “flu-like symptoms” including fever, chills, sweats, headache, fatigue, muscle and joint pain.
In a recently published case study, a previously healthy 67-year-old man developed sudden onset flu-like symptoms after working outdoors in rural Pennsylvania. He was seen in an urgent care facility and suspected of having COVID-19. He was diagnosed with “viral-like illness” and sent home to await test results.
Negative COVID test. Now what?
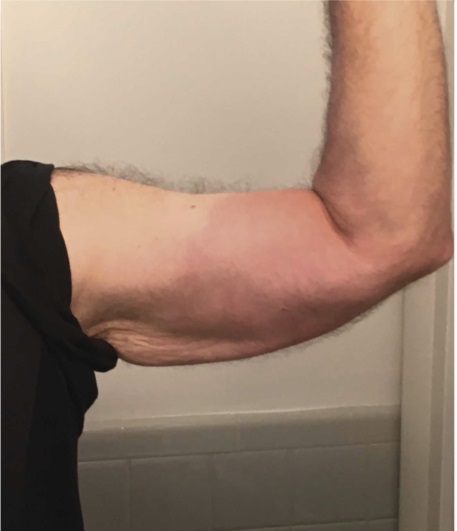
The COVID-19 test was negative, and over the next six weeks many of the patient’s flu-like symptoms resolved. However, he developed a skin rash. A dermatologist diagnosed him with an “insect bite” and ordered a test for Lyme disease, which came back positive.
We know from previous studies that delays in treatment for Lyme disease by as little as 30 days are associated with patients having persistent symptoms.
In our own MyLymeData published research, over 84% of Lyme patients were not properly diagnosed within the first four months of illness when antibiotics are most effective.
In this case, after a week of oral doxycycline, the patient developed several neurological symptoms including double vision, neck stiffness and pronounced fatigue. He was diagnosed with sixth nerve palsy and switched to oral cefuroxime.
It appears that the initial six-week delay in treatment resulted in disseminated Borrelia burgdorferi infection and neuroborreliosis. (Note: In Lyme disease, sixth cranial nerve palsy is not as common as seventh nerve facial palsy—also known as Bell’s palsy)
Once meningitis was ruled-out (by MRI and negative cerebral spinal fluid test), the patient was switched back to a higher dose of oral doxycycline for an additional four weeks.
At his follow-up appointment, the patient reported continuing insomnia, anxiety, fatigue, brain fog, and slight double vision.
Could earlier treatment have avoided neuro symptoms?
The patient says, “In my case, once the rash was observed, Lyme disease was considered to be the cause of my illness. However, the rash did not take place until more than five weeks after the initial symptoms were encountered. Had Lyme disease been considered in the first stages, perhaps treatments would have prevented the neurological/vision problems that developed later.”
The authors of the case study state, “Although COVID-19 has overlapping symptoms with other conditions, the need to exclude COVID-19 infection should not distract the clinician from simultaneous evaluation for infectious diseases that will benefit from early diagnosis and prompt treatment.”
This spring, millions of Americans will seek out testing for COVID-19 due to sudden onset of flu-like symptoms. When those tests come back negative, I sincerely hope their doctor will consider the possibility that they may have contracted Lyme or another tick-borne disease.
LymeSci is written by Lonnie Marcum, a Licensed Physical Therapist and mother of a daughter with Lyme. In 2019-2020, she served on a subcommittee of the federal Tick-Borne Disease Working Group. Follow her on Twitter: @LonnieRhea Email her at: lmarcum@lymedisease.org .
References
Cheryl B. Novak, Verna M. Scheeler, John N. Aucott, “Lyme Disease in the Era of COVID-19: A Delayed Diagnosis and Risk for Complications”, Case Reports in Infectious Diseases, vol. 2021, Article ID 6699536, 4 pages, 2021. https://doi.org/10.1155/2021/6699536
Hirsch AG, Poulsen MN, Nordberg C, Moon KA, Rebman AW, Aucott JN, Heaney CD and Schwartz BS (2020) Risk Factors and Outcomes of Treatment Delays in Lyme Disease: A Population-Based Retrospective Cohort Study. Front. Med. 7:560018. doi: 10.3389/fmed.2020.560018
Johnson L, Aylward A, Stricker RB. Healthcare access and burden of care for patients with Lyme disease: a large United States survey. Health Policy. 2011 Sep;102(1):64-71. Available from: http://www.ncbi.nlm.nih.gov/pubmed/21676482.